Skin of Color Dermatology: Why Current Medical Guidelines Are Leaving Patients Behind

Key Takeaways
Contemporary dermatology practice continues to demonstrate significant limitations in the diagnosis and management of conditions in patients with darker skin tones, contributing to measurable disparities in clinical outcomes. As individuals with skin of color currently represent approximately 40.9 percent of the United States population, with projections indicating an increase to nearly 59.5 percent by 2060, the need for equitable and inclusive dermatologic care has become increasingly urgent. Despite this demographic shift, gaps in medical education, diagnostic frameworks, and clinical research persist, limiting the ability of clinicians to provide accurate, timely, and culturally competent care.
A major contributing factor to these disparities lies in the underrepresentation of darker skin tones in medical education. Analyses of dermatology textbooks and teaching materials reveal that only 16 to 24 percent of clinical images depict conditions in darker skin. This lack of visual and experiential exposure has direct consequences for clinical competency, with nearly half of practicing dermatologists reporting inadequate training in recognizing and managing dermatologic conditions in patients with black skin. Since many dermatologic diagnoses rely heavily on visual pattern recognition, insufficient exposure during training can lead to missed or delayed diagnoses in clinical practice.
Diagnostic tools and scoring systems further compound these challenges. Many commonly used clinical assessment frameworks, including erythema based scoring systems, rely on the visualization of redness as a marker of inflammation. This approach is less reliable in darker skin tones, where inflammation may present with subtle color changes such as hyperpigmentation, violaceous hues, or textural alterations rather than overt erythema. Similarly, the Fitzpatrick skin type classification, although widely used, was originally developed to assess ultraviolet sensitivity rather than to capture the full spectrum of skin diversity. Its application in clinical decision making is therefore limited when used as a proxy for race, ethnicity, or disease presentation. These limitations can result in underestimation of disease severity, delayed intervention, and suboptimal treatment outcomes.
Disparities in melanoma outcomes provide a particularly concerning illustration of these systemic shortcomings. Although melanoma incidence is lower in Black populations compared with White populations, outcomes are significantly worse. Melanoma in patients with black skin presents with more advanced disease (16% vs. 5%) and shows dramatically lower five-year survival rates (66.2% vs. 90.1%) compared with White patients. Correspondingly, five year survival rates are substantially lower, at approximately 66.2 percent for Black patients versus 90.1 percent for White patients. These differences are largely attributed to delayed detection, atypical presentation patterns such as acral lentiginous melanoma, and reduced access to early diagnostic evaluation. The lack of clinician familiarity with how melanoma manifests in darker skin further exacerbates these delays.
Research disparities also play a critical role in perpetuating inequities. A relatively small proportion of dermatology studies report participant race or ethnicity, with estimates suggesting that only about 18 percent include such data. In melanoma research, the lack of diversity is even more pronounced, with approximately 96.5 percent of study participants identified as White. This lack of representation limits the generalizability of findings, restricts understanding of disease variation across populations, and impedes the development of tailored therapeutic strategies. As a result, evidence based guidelines may not adequately reflect the needs of diverse patient populations.
Addressing these challenges requires a coordinated and systemic approach. Medical education must be restructured to include comprehensive representation of skin conditions across the full spectrum of skin tones, supported by diverse image databases and clinical training opportunities. Diagnostic frameworks should be refined to incorporate features that are relevant to darker skin, moving beyond reliance on erythema to include pigmentation changes, lesion morphology, and patient reported symptoms. In parallel, research efforts must prioritize inclusive study design, standardized reporting of demographic data, and targeted investigation into conditions that disproportionately affect patients with skin of color.
Culturally competent care also represents a critical component of improving outcomes. Clinicians must be equipped to understand not only the biological variations in disease presentation but also the social, structural, and access related factors that influence health outcomes. Building trust, improving patient education, and addressing barriers to care are essential elements of an equitable dermatologic practice.
In summary, the current gaps in dermatology practice related to skin of color reflect broader systemic limitations in education, diagnostics, and research. These shortcomings contribute directly to delayed diagnoses, misclassification of disease severity, and poorer clinical outcomes. As the population becomes increasingly diverse, the imperative to modernize dermatologic care becomes more urgent. Advancing equity will require sustained investment in education, innovation in diagnostic approaches, and a commitment to inclusive research that ensures all patients receive accurate and effective care.
The Gap in Medical Education and Training
Limited exposure to darker skin conditions in medical school
Medical students receive minimal training on how cutaneous pathology presents across different skin tones. Visual diagnostic skills and pattern recognition in various skin types remain necessary for accurate diagnoses, yet students demonstrate lower competency in diagnosing dermatologic manifestations in darker skin compared with lighter skin. This educational deficiency begins at the earliest stage of medical training, where students encounter limited exposure to dermatology within the general medical school curriculum.
Analysis of dermatology lectures at medical schools reveals stark disparities in skin tone representation. In the first place, examination of four pre-clerkship lectures showed light/white skin accounted for 59.5% of all images, medium/brown skin types represented only 16.1%, and dark/black skin comprised 24.4%. Among 109 dermatologic conditions covered, 32% included images from only one skin tone, typically light/white skin, while merely 16% featured images of all three skin types.
Inadequate representation in dermatology textbooks
Dermatology textbooks demonstrate persistent underrepresentation of darker skin tones. Analysis shows the percentage of images depicting dark skin ranged from 4% to 18% across major textbooks. Many dermatology textbooks contained zero images of dark skin presenting with common conditions such as acne, psoriasis, or dermatitis. This lack of diverse representation in educational resources contributes to unequal early recognition of diseases across different skin types.
Images of skin of color remain underrepresented in American Academy of Dermatology annual meetings, medical textbooks, medical school curricular materials, and web-based medical resources. The limited representation of skin of color in medical education constitutes a longstanding issue in dermatology training. Although some diseases more common in skin of color populations receive adequate representation, diseases affecting both skin of color and non-skin of color patients equally show poor representation.
Comparison of current textbooks with those from 15 years prior revealed little progress. This educational gap carries direct clinical consequences, as the lack of brown and black images in dermatologic medical education may contribute to unequal early recognition of diseases, ultimately resulting in delayed or incorrect diagnosis, improper treatment, and increased morbidity and mortality for patients with skin of color.
Lack of specialized training programs
Published studies demonstrate gaps in knowledge regarding skin of color dermatology among medical students, residents, and attending physicians. These deficiencies extend to both diagnosis and treatment. The insufficiency of dermatologic training in skin of color creates knowledge gaps with notable implications for patient care.
Meanwhile, specialized programs have emerged to address these educational deficits. The American Academy of Dermatology developed a comprehensive Skin of Color Curriculum serving as a complete in-patient and out-patient curriculum for diagnosis and effective treatment of skin of color conditions. The curriculum targets dermatology residents and practicing dermatologists primarily, with medical students rotating through dermatology services as a secondary audience. Programs at institutions including UCSF and the University of Pennsylvania work with residents and medical students to teach principles of caring for patients seeking care through dedicated skin of color programs.
How Current Diagnostic Tools Fail Patients with Skin of Color
Classification systems and diagnostic tools used in dermatology demonstrate fundamental flaws when applied to darker skin types, creating measurable disparities in clinical outcomes.
Problems with the Fitzpatrick scale
The Fitzpatrick Skin Type classification represents the most commonly used skin tone assessment system in dermatologic practice. Developed in 1975, this scale originally categorized White patients’ skin tones based on propensity to burn or tan in response to sun exposure. The system initially included only four categories focused on white skin, with brown and black skin types (V and VI) added as an afterthought. Consequently, the scale has been criticized for its Eurocentric bias and insufficient representation of global skin color diversity.
The subjective nature of Fitzpatrick assessments creates inconsistencies in clinical documentation. Among 92 patient charts reviewed, only 36.96% had Fitzpatrick Skin Type consistently documented across multiple notes, while 30.43% showed conflicting types documented. Self-reporting of skin color using the scale proves less accurate than trained dermatologist assessment and excludes the majority of Black people who self-report. The scale reports that type V and VI skin “usually or always tans, never or rarely burns,” categorizations that are wholly inaccurate. Studies demonstrate sunburn among darker skin occurs much more commonly than previously thought.
Dermatologists have begun calling for alternatives to the Fitzpatrick scale, including the Roberts Skin Type Classification System and Taylor Hyperpigmentation Scale, which incorporate hyperpigmentation and scarring data. The colorimetric scale offers objective measurements using CIELAB color space values, providing a data-driven approach that reduces misclassification risks.
Erythema-based scoring systems underestimate severity
Clinician-reported outcome measures for inflammatory skin diseases rely heavily on erythema as a primary indicator of disease activity. Tools including the Investigator’s Global Assessment, Eczema Area and Severity Index, and Psoriasis Area and Severity Index depend on erythema visibility. Erythema can be visually obscured in patients with darker skin pigmentation due to increased melanin content, limiting these tools’ accuracy in assessing disease severity.
Inflammatory skin diseases can appear milder in patients with darker skin tones, even when severity is comparable to or greater than in lighter-skinned individuals. Erythema does not always appear as redness on darker skin tones; it often presents as violaceous coloring. This visual masking contributes to underdiagnosis and misclassification, particularly in atopic dermatitis where erythema serves as a heavily weighted criterion.
Visual diagnostic challenges in black skin
Common skin changes including pallor, cyanosis, and jaundice are not easily detectable when assessing patients with dark skin tones. In patients with Fitzpatrick types V or VI, skin injury or inflammation does not appear as erythema but may present as hyperpigmentation or darker coloring than surrounding skin. Cyanosis may present circumorally as grayish or white, while pallor associated with anemia appears as paleness in the conjunctiva and mucosa rather than on limb skin.
Dermatologists accurately characterized approximately 38% of skin condition images overall, but only 34% of images showing darker skin. General practitioners demonstrated similar accuracy decreases with darker skin. Dermatologists were also less likely to refer darker skin images of cutaneous T-cell lymphoma for biopsy.
Machine learning bias in skin cancer detection
Dermatological datasets demonstrate massive underrepresentation of darker skin tones. Among 21 databases containing 106,950 images, only 2,436 had skin type recorded. Of these, only 10 images showed brown skin and one showed dark brown or black skin. No images represented individuals with African, African-Caribbean, or South Asian backgrounds.
Algorithms trained predominantly on light-skinned individuals perform worse on brown and black skin. Prediction models trained on datasets with over 80% light-skinned individuals could not identify patients with skin of color. Generative AI models demonstrate similar bias, with 89.8% of generated images depicting light skin across four leading platforms.
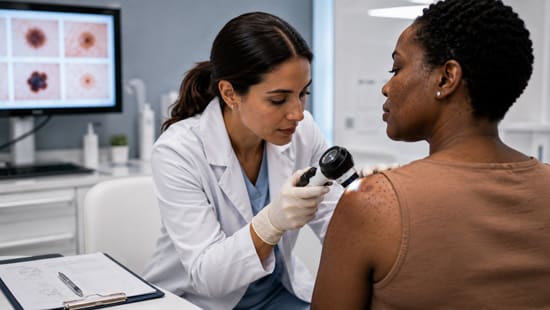
Common Black Skin Conditions Being Misdiagnosed or Missed
Misdiagnosis and delayed detection of dermatologic conditions in patients with darker skin produce measurable disparities in morbidity and mortality across multiple disease states.
Delayed melanoma detection in darker skin
Black patients with melanoma demonstrate a five-year survival rate of only 70% compared to 92% for white patients. Disproportionately high melanoma mortality rates in patients with skin of color may be driven by a lack of representation and data. Acral lentiginous melanoma poses particular challenges in individuals with skin of color, with African, Hispanic, and Asian individuals presenting with thicker, more advanced tumors at diagnosis. These populations encounter limited access to dermatologic care, under-recognition of melanoma presentation in darker skin types, and socioeconomic barriers leading to delayed diagnosis and treatment. Black men have a 26% higher rate of death than white men, which may be due to later stages of diagnosis.
Mycosis fungoides presenting differently
Mycosis fungoides, the most common primary cutaneous T-cell lymphoma, demonstrates increased incidence in Black patients with distinct clinical presentations. White patients presented with erythema of lesions in 90.4% of cases while Black patients showed erythema in only 28.8% of cases. In addition, hypopigmented lesions appeared in 51.4% of Black patients compared to 3.4% of white patients, with hyperpigmentation present in 53.4% versus 15.8% respectively. Black patients were diagnosed nine years younger than white patients, were predominantly female, and had worse overall survival. Hypopigmented mycosis fungoides, found predominantly in Black patients (59 of 62 cases), was associated with 100% ten-year survival compared to 51.8% in patients without this variant.
Atopic dermatitis severity underestimation
Atopic dermatitis affects up to 20% of Black children compared to 16% of white children. Black and Hispanic children tend to develop more severe cases compared to white children and are more likely to miss school because of their condition. Owing to difficulty identifying erythema in darker skin tones, severe cases may not be diagnosed or treated adequately in children with deep pigmentation. After adjusting for the redness score in the oSCORAD scale, Black children were found to have six times greater risk of severe atopic dermatitis compared to white children.
Psoriasis appearance variations
Psoriasis plaques appear as light to dark brown, purple, or gray on dark skin tones rather than the characteristic pink to red seen on lighter skin. African American patients experience more extensive disease involvement, reporting 3 to 10 palms of involvement compared to 1 or 2 palms for Caucasian patients. Mean baseline body surface area affected was 28.07% in Caucasians, 31.71% in African Americans, 32.69% in Hispanic/Latinos, and 41.35% in Asians. Dyspigmentation remains a common concern, with plaques resolving to hyper- or hypopigmented patches that may take 3 to 12 months to resolve.
Why Clinical Trials Don’t Represent the Full Spectrum of Skin Colors
Research participation patterns reveal profound gaps in dermatology clinical trial enrollment that directly impact treatment development for patients with darker skin types.
Racial demographics of dermatology research participants
Analysis of United States dermatology guidelines demonstrates that 61% did not include skin of color keywords. Examination of patient diversity in studies supporting American Academy of Dermatology treatment guidelines for cutaneous malignancies revealed only 45 of 248 references with patient-level data reported race or ethnicity, representing 18.1% of total studies. White or Caucasian populations dominated these references, with 25 of 45 studies reporting exclusively white samples. Population-based cohorts showed melanoma, cutaneous squamous cell carcinoma, and basal cell carcinoma cases comprised 96.5%, 90.0%, and 90.0% white patients respectively.
Comparison to census data reveals persistent underrepresentation. While Black or African American individuals constitute 13.6% of the population, they comprised only 7.9% of total participants across analyzed studies. This underrepresentation persisted even when accounting for disease prevalence rates. American Indian or Alaskan Native populations and individuals identifying as two or more races also showed marked underrepresentation. Hispanic or Latino individuals represented 18.9% of census data but only 14.1% of trial participants in studies reporting ethnicity.
Missing data on treatment efficacy for darker skin types
The limited diversity in research samples creates knowledge gaps regarding treatment efficacy. A systematic review analyzing 626 published randomized controlled trials found only 60% reported data on race and ethnicity, with 74% of participants being White. Psoriasis studies demonstrated particularly poor diversity, with only 12.1% including at least 20% non-White participants. Moreover, inclusion of minority groups remained unchanged over the past decade for dermatology clinical trials.
Barriers to minority enrollment in studies
Multiple obstacles prevent diverse participation in dermatology research. Mistrust stemming from historical and systemic factors creates skepticism about medical research within certain communities. Accessibility challenges including location, transportation, and financial constraints further limit participation. Most counties with Black, Hispanic, and Native American majorities offer no access to dermatologists, fueling disparities in both care quality and research enrollment. Additionally, lack of awareness about available trials restricts participation opportunities.
What Needs to Change: Building Better Guidelines for All Skin Types
Systemic reforms across medical education, clinical practice, and healthcare delivery remain necessary to address disparities in skin of color dermatology.
Expanding medical education resources
The Skin of Color Society provides educational videos and mentorship programs connecting early-career dermatologists with experts. Organizations have developed inclusive image databases including The Full Spectrum of Dermatology atlas, which distributed 17,000 print copies globally and offers 1,300 high-quality images across 140 conditions. VisualDx maintains approximately one-third of its images as Fitzpatrick types IV-VI. Medical schools incorporating skin of color lectures improved student diagnostic accuracy on darker skin presentations.
Developing culturally competent care practices
The 5As Social Care Framework adapted for dermatology includes Awareness of social risk factors, Assistance through standardized screening, Adjustment of clinical practices, Alignment of insurance policies, and Advocacy for policy change. Only 17% of non-academic dermatology practices accept Medicaid, despite nearly 60% of Medicaid enrollees being people of color. Cultural competency training addresses language barriers, with 12% of Hispanic patients reporting communication difficulties.
Increasing diversity in the dermatology workforce
The AAD’s Pathways initiative aims to increase Black, Latino, and Indigenous dermatology residents from 100 to 250 by 2027. Black and Hispanic dermatologists represent only 3% of practicing dermatologists, disproportionate to population demographics.
Creating inclusive diagnostic criteria
Development of alternatives to erythema-based scoring systems and Fitzpatrick scale modifications address diagnostic limitations in darker skin types.
Improving access to dermatologic care
Community screening programs targeting skin of color populations identified five suspicious skin cancers among 170 participants, with 95% identifying as African American, Asian, or Hispanic.
Addressing disparities in skin of color dermatology requires coordinated action across multiple domains. Medical education must incorporate diverse skin tone representation in textbooks and curricula. Diagnostic tools need recalibration beyond erythema-based assessments and Fitzpatrick scale limitations. Clinical trials must prioritize enrollment of underrepresented populations to establish treatment efficacy across all skin types.
Given that patients with darker skin comprise a growing majority of the population, these changes cannot wait. Dermatology departments should implement specialized training programs immediately. Practitioners must recognize that conditions present differently across skin tones. Without a doubt, closing these gaps will require sustained commitment from academic institutions, professional organizations, and individual clinicians dedicated to equitable patient outcomes.
FAQs
Q1. Why do patients with darker skin have worse outcomes for melanoma? Patients with darker skin experience significantly lower five-year survival rates for melanoma (66.2% compared to 90.1% in White patients) primarily due to delayed detection and more advanced disease at diagnosis. This stems from limited training on how melanoma presents in darker skin, underrepresentation in medical education materials, and diagnostic tools that don’t account for how skin conditions appear differently across various skin tones.
Q2. What are the main problems with the Fitzpatrick skin type scale? The Fitzpatrick scale was originally developed in 1975 for White patients based on sun exposure response, with darker skin types added later as an afterthought. It has significant limitations including Eurocentric bias, subjective assessments that lead to inconsistent documentation, and inaccurate categorizations (claiming darker skin “never burns” when sunburn actually occurs more commonly than previously thought). Many dermatologists now advocate for alternative classification systems.
Q3. How does atopic dermatitis present differently in Black children? Atopic dermatitis affects up to 20% of Black children and tends to be more severe than in white children, yet it’s often underdiagnosed. The condition is harder to identify in darker skin because erythema (redness) is difficult to see due to increased melanin. When adjustments are made for the redness score, Black children show six times greater risk of severe atopic dermatitis compared to white children.
Q4. Why are clinical trials for dermatology treatments not representative of all skin colors? Only 18% of studies supporting dermatology treatment guidelines report race or ethnicity data, and when they do, participants are predominantly White (often 90-96% in skin cancer studies). Black individuals are underrepresented even when accounting for disease prevalence. Barriers include mistrust from historical factors, accessibility challenges, lack of awareness about trials, and the fact that most counties with Black, Hispanic, and Native American majorities have no access to dermatologists.
Q5. What changes are being made to improve dermatology care for patients with skin of color? Several initiatives are underway including the AAD’s Pathways program to increase Black, Latino, and Indigenous dermatology residents, development of inclusive image databases like The Full Spectrum of Dermatology atlas with 1,300 images across 140 conditions, specialized training curricula for residents, and community screening programs. Medical schools incorporating skin of color lectures have shown improved student diagnostic accuracy on darker skin presentations.
References
[2] – https://www.cureus.com/articles/415478-diagnostic-disparities-in-erythema-visibility-a-call-to-redefine-inflammatory-assessment-in-diverse-skin-tones.pdf
[3] – https://www.theguardian.com/society/2021/nov/09/ai-skin-cancer-diagnoses-risk-being-less-accurate-for-dark-skin-study
[4] – https://pubmed.ncbi.nlm.nih.gov/36069854/
[5] – https://pmc.ncbi.nlm.nih.gov/articles/PMC4255694/
[6] – https://my.clevelandclinic.org/health/articles/24941-how-psoriasis-affects-black-people-and-people-of-color
[7] – https://www.ama-assn.org/public-health/health-equity/dermatology-health-disparities-can-be-skin-deep
[8] – https://libguides.urmc.rochester.edu/c.php?g=1254851
[9] – https://nextstepsinderm.com/derm-topics/the-full-spectrum-of-dermatology-a-growing-resource-for-inclusive-dermatologic-care/
[10] – https://jddonline.com/articles/impact-of-increasing-skin-of-color-representation-in-pre-clerkship-dermatology-curriculum-S1545961625P8874X
[11] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12626340/
[12] – https://nursing.ceconnection.com/files/SkinAssessmentinPatientswithDarkSkinTone-1710365262888.pdf;jsessionid=D8258F3315A12169D196798C06E49E9C
[13] – https://news.mit.edu/2024/doctors-more-difficulty-diagnosing-diseases-images-darker-skin-0205
[14] – https://www.curemelanoma.org/blog/making-ai-work-for-people-of-color-diagnosing-melanoma-and-other-skin-cancers
[15] – https://www.probiologists.com/article/racial-underrepresentation-in-dermatological-datasets-leads-to-biased-machine-learning-models-and-inequitable-healthcare
[16] – https://pubmed.ncbi.nlm.nih.gov/40668069/
[17] – https://naacp.org/resources/addressing-misdiagnosis-melanoma-black-men
[18] – https://acsjournals.onlinelibrary.wiley.com/doi/full/10.1002/cncy.22229
[19] – https://skin.substack.com/p/melanoma-misdiagnosis-why-patients
[20] – https://pmc.ncbi.nlm.nih.gov/articles/PMC10981557/
[21] – https://www.healio.com/news/allergy-asthma/20230822/challenges-remain-in-diagnosing-treating-skin-of-color-with-atopic-dermatitis
[22] – https://nationaleczema.org/blog/the-science-of-eczema-on-darker-skin/
[23] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12090960/
[24] – https://www.healio.com/news/dermatology/20230424/dermatological-clinical-trials-lack-racial-ethnic-diversity
[25] – https://www.pharmacytimes.com/view/experts-highlight-the-need-for-greater-diversity-in-dermatological-clinical-research
[26] – https://www.ajmc.com/view/underscoring-the-diversity-issue-in-dermatology-clinical-trials-therapeutics-and-care-management
[27] – https://dermatrials.medicine.iu.edu/blogs/diversity-in-dermatology-clinical-trials
[28] – https://www.visualdx.com/blog/addressing-racial-health-disparities-in-dermatology-adapting-the-5as-social-care-framework/
[29] – https://www.panfoundation.org/wp-content/uploads/2024/03/State-of-Patient-Access-Focus-Brief-Patients-of-Color-PAN-Foundation.pdf
[30] – https://www.aad.org/news/pathways-inclusivity-in-dermatology-launch
[31] – https://www.dermatologytimes.com/view/improving-representation-of-skin-of-color-in-dermatology
[32] – https://www.froedtert.com/stories/advancing-health-equity-dermatology-through-community-outreach-and-partnerships
Recent Articles


Integrative Perspectives on Cognition, Emotion, and Digital Behavior

Sleep-related:
Longevity/Nutrition & Diet:
Philosophical / Happiness / Social:
Other:
Modern Mind Unveiled
Developed under the direction of David McAuley, Pharm.D., this collection explores what it means to think, feel, and connect in the modern world. Drawing upon decades of clinical experience and digital innovation, Dr. McAuley and the GlobalRPh initiative translate complex scientific ideas into clear, usable insights for clinicians, educators, and students.
The series investigates essential themes—cognitive bias, emotional regulation, digital attention, and meaning-making—revealing how the modern mind adapts to information overload, uncertainty, and constant stimulation.
At its core, the project reflects GlobalRPh’s commitment to advancing evidence-based medical education and clinical decision support. Yet it also moves beyond pharmacotherapy, examining the psychological and behavioral dimensions that shape how healthcare professionals think, learn, and lead.
Through a synthesis of empirical research and philosophical reflection, Modern Mind Unveiled deepens our understanding of both the strengths and vulnerabilities of the human mind. It invites readers to see medicine not merely as a science of intervention, but as a discipline of perception, empathy, and awareness—an approach essential for thoughtful practice in the 21st century.
The Six Core Themes
I. Human Behavior and Cognitive Patterns
Examining the often-unconscious mechanisms that guide human choice—how we navigate uncertainty, balance logic with intuition, and adapt through seemingly irrational behavior.
II. Emotion, Relationships, and Social Dynamics
Investigating the structure of empathy, the psychology of belonging, and the influence of abundance and selectivity on modern social connection.
III. Technology, Media, and the Digital Mind
Analyzing how digital environments reshape cognition, attention, and identity—exploring ideas such as gamification, information overload, and cognitive “nutrition” in online spaces.
IV. Cognitive Bias, Memory, and Decision Architecture
Exploring how memory, prediction, and self-awareness interact in decision-making, and how external systems increasingly serve as extensions of thought.
V. Habits, Health, and Psychological Resilience
Understanding how habits sustain or erode well-being—considering anhedonia, creative rest, and the restoration of mental balance in demanding professional and personal contexts.
VI. Philosophy, Meaning, and the Self
Reflecting on continuity of identity, the pursuit of coherence, and the construction of meaning amid existential and informational noise.
Keywords
Cognitive Science • Behavioral Psychology • Digital Media • Emotional Regulation • Attention • Decision-Making • Empathy • Memory • Bias • Mental Health • Technology and Identity • Human Behavior • Meaning-Making • Social Connection • Modern Mind
Video Section 

