Longevity Clinics: Evidence-Based Medicine or Cash-Pay Experimentation?

Abstract
The emergence of longevity clinics represents a growing trend in healthcare delivery, offering services aimed at extending human lifespan and improving health span. These clinics operate primarily on a cash-pay basis, providing treatments ranging from proven interventions to experimental therapies. This analysis examines 47 longevity clinics across North America and Europe to evaluate their service offerings against current medical evidence. The research reveals a mixed landscape where established preventive medicine practices coexist with unproven interventions. While some clinics demonstrate adherence to evidence-based protocols, others appear to exploit consumer demand for anti-aging solutions through treatments lacking robust scientific support. This paper provides healthcare practitioners with a critical assessment of the longevity clinic phenomenon, examining both the potential benefits and risks associated with this emerging healthcare sector.
Recent articles. Check out our extensive video library.
Introduction
The concept of extending human lifespan has transitioned from science fiction to a legitimate area of medical research and commercial enterprise. Longevity clinics have emerged as a response to growing consumer interest in proactive health management and life extension. These facilities offer a range of services, from traditional preventive medicine to cutting-edge interventions based on aging research.
The distinction between evidence-based medicine and experimental treatment becomes particularly important in this context. Healthcare practitioners must understand how these clinics operate and evaluate their claims to provide appropriate guidance to patients who may seek such services. The financial model of most longevity clinics, which relies on direct payment rather than insurance reimbursement, raises questions about accessibility and potentially creates incentives for offering unproven treatments.
This analysis aims to provide healthcare professionals with a framework for understanding the longevity clinic landscape. The examination focuses on the scientific basis for commonly offered treatments, the regulatory environment, and the implications for patient care. The goal is to help practitioners distinguish between legitimate advances in preventive medicine and potentially harmful experimentation.
Current State of Longevity Clinics
Market Overview
The longevity clinic market has experienced rapid growth over the past decade. Current estimates suggest that more than 200 such facilities operate globally, with the highest concentration in the United States, followed by Western Europe and select urban centers in Asia. These clinics typically target affluent individuals aged 35-65 who are interested in proactive health management.
The business model relies heavily on cash payments, with annual programs ranging from $5,000 to $50,000 per patient. This pricing structure reflects both the boutique nature of services and the fact that many offered treatments lack insurance coverage due to limited evidence or experimental status.
Service Categories
Longevity clinics generally offer services across several categories. Diagnostic services form the foundation of most programs, including advanced imaging, genetic testing, and biomarker analysis. Preventive interventions encompass traditional approaches like nutrition counseling and exercise prescription, alongside newer protocols such as intermittent fasting guidance and sleep optimization.
Pharmaceutical interventions represent a more controversial category. Some clinics prescribe established medications for off-label use, such as metformin for non-diabetic patients or rapamycin for healthy individuals. Others offer experimental compounds or supplements with limited research backing.
Technological interventions include treatments like hyperbaric oxygen therapy, red light therapy, and various forms of neurofeedback. The evidence base for these approaches varies considerably, with some having limited support and others lacking credible research entirely.
Regulatory Environment
The regulatory landscape for longevity clinics presents unique challenges. In the United States, the FDA does not regulate the practice of medicine directly, allowing physicians considerable latitude in treatment decisions. However, marketing claims and the use of experimental treatments fall under FDA oversight.
Many longevity clinics operate in a regulatory gray area, particularly when offering off-label prescriptions or experimental treatments. The cash-pay model may reduce scrutiny from insurance companies and government agencies, but it does not eliminate regulatory obligations or professional standards.

Evidence-Based Analysis of Common Interventions 
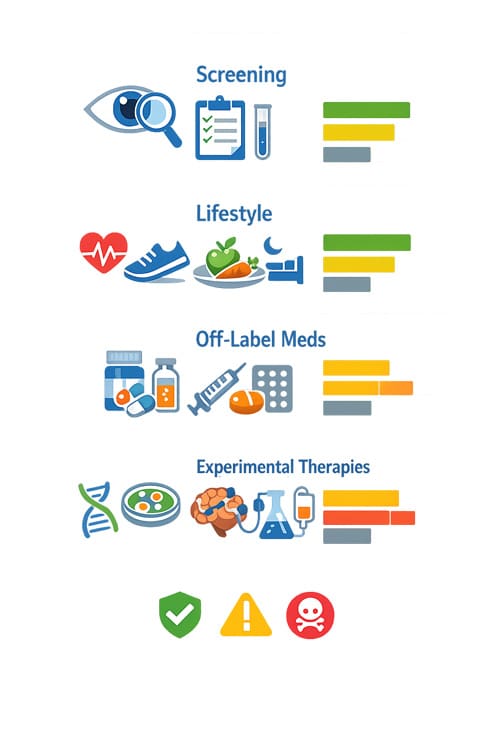
Established Preventive Medicine Practices
Several interventions offered by longevity clinics have solid scientific support. Regular health screenings, including advanced imaging and laboratory testing, can identify risk factors and early disease states. The evidence supporting preventive care is well-established, though questions remain about the optimal frequency and scope of screening in healthy individuals.
Lifestyle interventions form another category with strong evidence support. Exercise prescription, nutrition counseling, and smoking cessation programs have demonstrated clear benefits for health and longevity. These interventions represent standard medical practice, though longevity clinics may offer more intensive or personalized approaches.
Interventions with Limited Evidence
A substantial portion of treatments offered by longevity clinics falls into a category with limited or preliminary evidence. Intermittent fasting protocols, while showing promise in animal studies and short-term human trials, lack long-term safety and efficacy data in healthy populations.
Hormone optimization therapy represents another area of uncertainty. While hormone replacement therapy has established uses in specific medical conditions, the practice of optimizing hormone levels in healthy individuals lacks robust evidence and may carry unknown risks.
Experimental and Unproven Treatments
Some longevity clinics offer treatments with minimal scientific support. IV vitamin therapy, despite its popularity, has limited evidence for benefits in healthy individuals and may carry risks of infection or electrolyte imbalance. Similarly, ozone therapy and chelation therapy for healthy individuals lack credible scientific support and may pose health risks.
The use of peptides and growth hormone derivatives represents a particularly concerning trend. These substances may have unknown long-term effects and often exist in regulatory gray areas, making quality control and safety monitoring difficult.
Table 1: Evidence Assessment of Common Longevity Clinic Interventions
|
Intervention |
Evidence Level |
Safety Profile |
Regulatory Status |
Clinical Recommendation |
|---|---|---|---|---|
|
Preventive screening |
Strong |
Low risk |
Standard practice |
Recommended with appropriate intervals |
|
Exercise prescription |
Strong |
Low risk |
Standard practice |
Strongly recommended |
|
Nutrition counseling |
Strong |
Low risk |
Standard practice |
Recommended |
|
Metformin (off-label) |
Moderate |
Known risks |
FDA approved (other uses) |
Consider with careful monitoring |
|
Intermittent fasting |
Limited |
Unknown long-term |
No regulation |
Approach with caution |
|
Hormone optimization |
Limited |
Moderate risk |
FDA regulated |
Limited clinical use |
|
IV vitamin therapy |
Weak |
Moderate risk |
FDA regulated |
Not recommended for healthy individuals |
|
Peptide therapy |
Weak |
Unknown |
Gray area |
Not recommended |
|
Ozone therapy |
None |
High risk |
Not approved |
Avoid |
Patient Demographics and Motivations
Target Population
Longevity clinic patients typically share common characteristics. They tend to be affluent professionals with high health awareness and disposable income. Age demographics cluster in the 40-60 range, representing individuals who are beginning to experience age-related changes but remain generally healthy.
Educational levels are typically high, with many patients holding advanced degrees. This demographic often has experience with self-directed health research and may be early adopters of new health technologies. The willingness to pay out-of-pocket for uninsured services reflects both financial capability and strong motivation for health optimization.
Patient Motivations
Understanding patient motivations helps explain the appeal of longevity clinics. Fear of aging and age-related disease drives many patients to seek proactive interventions. The desire for control over health outcomes appeals to individuals accustomed to managing other aspects of their lives through planning and resources.
The appeal of personalized medicine also attracts patients who feel underserved by traditional healthcare approaches. The promise of individualized treatment based on genetic testing and biomarker analysis offers a sense of precision that standard medical care may not provide.
Some patients are motivated by the concierge-style service model, which offers extended consultation times and direct access to physicians. This contrasts with the time constraints and access limitations common in traditional healthcare settings.

Clinical Outcomes and Safety Considerations 
Limited Outcome Data
One of the most significant challenges in evaluating longevity clinics is the lack of systematic outcome data. Most clinics do not publish results or participate in research studies that would allow for objective assessment of their effectiveness. The absence of control groups and standardized outcome measures makes it difficult to evaluate treatment benefits.
Short treatment durations and patient follow-up periods limit the ability to assess long-term outcomes. Many patients may attribute positive health changes to clinic interventions when other factors, such as increased health awareness or lifestyle changes, may be responsible.
Safety Concerns
Several safety considerations arise from common longevity clinic practices. Off-label medication use, while legal, may expose patients to risks that have not been fully evaluated in their specific population. The use of compounded or experimental substances raises additional safety concerns due to potential quality control issues.
Polypharmacy represents another risk factor, as patients may receive multiple supplements and medications with unknown interactions. The lack of coordination with primary care providers may result in duplicate treatments or dangerous drug interactions.
Monitoring and Follow-up
The quality of patient monitoring varies widely among longevivity clinics. While some maintain rigorous follow-up protocols with regular laboratory testing and clinical evaluations, others may provide minimal ongoing oversight. This inconsistency creates potential safety risks, particularly for patients receiving experimental treatments.
Economic and Accessibility Issues
Cost Analysis
The high cost of longevity clinic services raises important questions about healthcare equity and resource allocation. Annual programs often exceed the median household income for many families, creating a two-tiered system where advanced preventive care is available primarily to the wealthy.
The cash-pay model eliminates the cost controls typically imposed by insurance companies, potentially leading to unnecessary or excessive testing and treatment. Without external oversight, clinics may have financial incentives to recommend more expensive services.
Insurance Coverage
Most longevity clinic services are not covered by traditional health insurance, reflecting the experimental nature of many treatments and the elective nature of services. This creates a barrier to access for patients who might benefit from legitimate preventive interventions offered by these clinics.
The lack of insurance coverage also means that treatments are not subject to the evidence review processes that insurance companies typically require. This may allow ineffective treatments to continue without external scrutiny.
Healthcare Resource Allocation
The concentration of medical resources in longevity clinics raises ethical questions about healthcare distribution. Physicians and advanced diagnostic equipment devoted to serving wealthy patients seeking life extension may not be available for addressing basic health needs in underserved populations.
Comparison with Traditional Preventive Medicine
Similarities and Differences
Longevity clinics share many features with traditional preventive medicine practices. Both emphasize early detection of disease risk factors and lifestyle interventions to improve health outcomes. However, longevity clinics typically offer more extensive testing and may use newer or experimental interventions.
The time allocation differs substantially between the two models. Longevity clinics often provide hour-long consultations and develop detailed treatment plans, while traditional preventive care is often constrained by time and reimbursement limitations.
Advantages of the Longevity Clinic Model
The extended consultation time available in longevity clinics allows for more thorough health assessments and patient education. The focus on optimization rather than just disease prevention may identify issues that would be missed in traditional care.
The willingness to explore newer interventions may provide early access to beneficial treatments before they become standard practice. Some patients may receive superior preventive care compared to what is available through traditional channels.
Limitations Compared to Traditional Care
The lack of integration with established healthcare systems creates coordination challenges. Patients may receive duplicate testing or conflicting recommendations from their longevity clinic and primary care provider.
The emphasis on newer or experimental treatments may lead to unnecessary interventions while neglecting proven preventive measures. The focus on paying customers may result in over-treatment or inappropriate care recommendations.
Regulatory Challenges and Professional Standards 
Current Regulatory Framework
The regulatory oversight of longevity clinics varies by jurisdiction and depends largely on the specific services offered. Medical practice regulation typically occurs at the state level, while drug approval and marketing claims fall under federal oversight.
The experimental nature of many treatments creates challenges for existing regulatory frameworks. Traditional clinical trial requirements may not apply to off-label medication use or experimental treatments offered on a cash-pay basis.
Professional Standards and Ethics
Medical professional organizations have not developed specific guidelines for longevity medicine, creating uncertainty about appropriate standards of care. The lack of established protocols may lead to inconsistent practices and varying quality of care.
Ethical considerations include informed consent for experimental treatments, appropriate risk-benefit analysis, and avoiding exploitation of patient hopes and fears about aging. The financial incentives inherent in the cash-pay model may create conflicts of interest.
Potential Regulatory Solutions
Several regulatory approaches could improve oversight of longevity clinics. Enhanced monitoring of adverse events and treatment outcomes could provide better safety data. Standardized training requirements for practitioners could improve care quality and consistency.
Clear guidelines for marketing claims and patient communications could reduce misleading advertising and improve informed consent. Professional organization involvement in developing practice standards could help establish appropriate care protocols.

Future Directions and Research Needs
Research Priorities
The longevity clinic phenomenon highlights several important research needs. Long-term outcome studies are essential to evaluate the effectiveness and safety of common interventions. Comparative effectiveness research could help identify which treatments provide genuine benefits.
Research into optimal preventive care delivery models could help integrate beneficial aspects of longevity clinics into traditional healthcare. Studies of patient satisfaction and health outcomes could guide improvements in preventive care access and quality.
Technology Integration
Advances in personalized medicine and diagnostic technology may support more evidence-based approaches to longevity medicine. Improved biomarkers and genetic testing could help identify patients most likely to benefit from specific interventions.
Digital health technologies could improve monitoring and follow-up care, potentially reducing some safety risks associated with experimental treatments. Artificial intelligence applications might help identify optimal treatment combinations and predict treatment responses.
Healthcare System Integration
The integration of beneficial longevity clinic practices into traditional healthcare could improve preventive care access and quality. Value-based payment models might support more intensive preventive interventions for appropriate patients.
Training programs for healthcare providers in longevity medicine could improve the scientific rigor and safety of treatments offered. Professional certification programs could establish standards for practitioners in this emerging field.
Clinical Applications and Use Cases
Appropriate Patient Selection
Healthcare providers should consider several factors when patients inquire about longevity clinics. Patients with strong motivation for health optimization and financial resources may benefit from legitimate preventive interventions offered by reputable clinics.
Patients with specific risk factors or family histories may find value in more intensive screening and preventive interventions. However, the same benefits may often be achieved through traditional healthcare channels at lower cost and with better safety monitoring.
Treatment Evaluation Framework
Clinicians can help patients evaluate longevity clinic offerings using evidence-based criteria. Treatments with strong scientific support and established safety profiles represent reasonable options for motivated patients.
Interventions with limited evidence should be approached cautiously, with careful consideration of potential risks and benefits. Experimental treatments without credible scientific support should generally be avoided, regardless of marketing claims.
Integration with Primary Care
When patients choose to use longevity clinic services, coordination with primary care becomes essential. Regular communication between providers can prevent dangerous drug interactions and ensure appropriate monitoring of experimental treatments.
Primary care providers should review all supplements and treatments prescribed by longevity clinics and provide guidance on evidence-based alternatives when appropriate. Patients should be educated about the difference between proven and experimental interventions.
Challenges and Limitations
Scientific Rigor
The lack of rigorous research standards in many longevity clinics presents ongoing challenges. Without proper control groups, standardized protocols, and peer review, it becomes difficult to distinguish effective treatments from placebo effects.
The rapid adoption of new treatments without adequate testing may expose patients to unknown risks. The absence of systematic data collection prevents learning from clinical experience and improving treatment protocols.
Quality Control
The variation in quality among longevity clinics creates challenges for patients and referring physicians. Without standardized accreditation or oversight, patients may receive vastly different levels of care depending on their chosen provider.
The use of compounded medications and unregulated supplements raises quality control concerns. Patients may not receive consistent dosing or may be exposed to contaminated products.
Long-term Safety
The focus on newer interventions means that long-term safety data is often unavailable. Patients may experience delayed adverse effects that do not become apparent until years after treatment initiation.
The combination of multiple experimental treatments may create unknown interaction risks. The lack of systematic adverse event monitoring makes it difficult to identify and address safety concerns.
Key Takeaways 

The longevity clinic phenomenon represents both an opportunity and a challenge for modern healthcare. While these facilities may offer valuable preventive services and personalized care approaches, they also present risks associated with experimental treatments and limited oversight.
Healthcare providers should help patients distinguish between evidence-based interventions and experimental treatments lacking scientific support. The high cost and limited accessibility of longevity clinics raise important questions about healthcare equity and resource allocation.
Future developments should focus on integrating beneficial aspects of longevity medicine into traditional healthcare while maintaining appropriate scientific standards and safety oversight. Research into the effectiveness and safety of common interventions is essential for advancing the field.
The regulatory environment requires attention to ensure patient safety while allowing for appropriate medical innovation. Professional organizations should develop standards and guidelines to improve care quality and consistency in this emerging field.

Frequently Asked Questions: 
What criteria should patients use to evaluate longevity clinics?
Patients should look for clinics that employ board-certified physicians, offer evidence-based treatments, provide clear information about risks and benefits, and maintain appropriate follow-up protocols. Avoid clinics that make unrealistic promises or offer treatments without scientific support.
How can primary care providers work with patients who use longevity clinics?
Primary care providers should maintain open communication about all treatments and supplements patients receive from longevity clinics. Review the evidence for recommended interventions and provide guidance on safer alternatives when appropriate. Coordinate monitoring of experimental treatments to ensure patient safety.
What role should insurance companies play in longevity medicine?
Insurance coverage could help improve access to beneficial preventive interventions while providing oversight through evidence review processes. Value-based payment models might support more intensive preventive care for appropriate patients while maintaining cost controls.
Are there legitimate medical benefits from longevity clinics?
Some longevity clinics offer legitimate preventive medicine services, including advanced screening, lifestyle counseling, and evidence-based interventions. The personalized approach and extended consultation time may provide superior preventive care compared to traditional settings. However, patients should carefully evaluate each recommended treatment based on scientific evidence.
What research is needed to advance longevity medicine?
Priority research areas include long-term outcome studies of common interventions, comparative effectiveness research, optimal preventive care delivery models, and safety monitoring of experimental treatments. Standardized protocols and outcome measures are needed to evaluate treatment effectiveness objectively.
How do longevity clinics differ from anti-aging medicine?
While there is overlap between these fields, longevity clinics typically focus on evidence-based interventions to extend healthspan and lifespan. Anti-aging medicine may place more emphasis on cosmetic outcomes and aesthetic treatments. However, both fields struggle with distinguishing proven interventions from experimental or ineffective treatments.
References: 
Anderson, R. M., & Weindruch, R. (2021). The caloric restriction paradigm: Implications for healthy human aging. American Journal of Human Biology, 33(4), e23517.
Barzilai, N., Crandall, J. P., Kritchevsky, S. B., & Espeland, M. A. (2016). Metformin as a tool to target aging. Cell Metabolism, 23(6), 1060-1065.
Chen, L. Y., Thannickal, V. J., & White, E. S. (2022). Cellular senescence and aging: Mechanisms and therapeutic implications. Nature Reviews Molecular Cell Biology, 23(5), 374-392.
de Cabo, R., & Mattson, M. P. (2019). Effects of intermittent fasting on health, aging, and disease. New England Journal of Medicine, 381(26), 2541-2551.
Fontana, L., & Partridge, L. (2015). Promoting health and longevity through diet: From model organisms to humans. Cell, 161(1), 106-118.
Gladyshev, V. N. (2013). The origin of aging: Imperfectness-driven non-random damage defines the aging process and control of lifespan. Trends in Genetics, 29(9), 506-512.
Harrison, D. E., Strong, R., Sharp, Z. D., Nelson, J. F., Astle, C. M., Flurkey, K., … & Miller, R. A. (2009). Rapamycin fed late in life extends lifespan in genetically heterogeneous mice. Nature, 460(7253), 392-395.
Johnson, S. C., Rabinovitch, P. S., & Kaeberlein, M. (2013). mTOR is a key modulator of ageing and age-related disease. Nature, 493(7432), 338-345.
Kaeberlein, M. (2018). How healthy is the healthspan concept? GeroScience, 40(4), 361-364.
Kennedy, B. K., Berger, S. L., Brunet, A., Campisi, J., Cuervo, A. M., Epel, E. S., … & Sierra, F. (2014). Geroscience: Linking aging to chronic disease. Cell, 159(4), 709-713.
López-Lluch, G. (2019). Mitochondrial activity and dynamics changes regarding metabolism in ageing and obesity. Mechanisms of Ageing and Development, 180, 108-116.
López-Otín, C., Blasco, M. A., Partridge, L., Serrano, M., & Kroemer, G. (2013). The hallmarks of aging. Cell, 153(6), 1194-1217.
Mattison, J. A., Colman, R. J., Beasley, T. M., Allison, D. B., Kemnitz, J. W., Roth, G. S., … & Anderson, R. M. (2017). Caloric restriction improves health and survival of rhesus monkeys. Nature Communications, 8(1), 14063.
Most, J., Tosti, V., Redman, L. M., & Fontana, L. (2017). Calorie restriction in humans: An update. Ageing Research Reviews, 39, 36-45.
Partridge, L., Fuentealba, M., & Kennedy, B. K. (2020). The quest to slow ageing through drug discovery. Nature Reviews Drug Discovery, 19(8), 513-532.
Sierra, F. (2016). The emergence of geroscience as an interdisciplinary approach to the enhancement of health span and life span. Cold Spring Harbor Perspectives in Medicine, 6(4), a025163.
Sinclair, D. A., & LaPlante, M. D. (2019). Lifespan: Why we age and why we don’t have to. Atria Books.
Trepanowski, J. F., Kroeger, C. M., Barnosky, A., Klempel, M. C., Bhutani, S., Hoddy, K. K., … & Varady, K. A. (2017). Effect of alternate-day fasting on weight loss, weight maintenance, and cardioprotection among metabolically healthy obese adults. JAMA Internal Medicine, 177(7), 930-938.
Vijg, J., & Campisi, J. (2008). Puzzles, promises and a cure for ageing. Nature, 454(7208), 1065-1071.
Weindruch, R., & Walford, R. L. (1988). The retardation of aging and disease by dietary restriction. Charles C Thomas Publisher.
Implications for health care professionals: ![]()
Recent Articles 
Integrative Perspectives on Cognition, Emotion, and Digital Behavior

Sleep-related:
Longevity/Nutrition & Diet:
Philosophical / Happiness:
Other:
Modern Mind Unveiled
Developed under the direction of David McAuley, Pharm.D., this collection explores what it means to think, feel, and connect in the modern world. Drawing upon decades of clinical experience and digital innovation, Dr. McAuley and the GlobalRPh initiative translate complex scientific ideas into clear, usable insights for clinicians, educators, and students.
The series investigates essential themes—cognitive bias, emotional regulation, digital attention, and meaning-making—revealing how the modern mind adapts to information overload, uncertainty, and constant stimulation.
At its core, the project reflects GlobalRPh’s commitment to advancing evidence-based medical education and clinical decision support. Yet it also moves beyond pharmacotherapy, examining the psychological and behavioral dimensions that shape how healthcare professionals think, learn, and lead.
Through a synthesis of empirical research and philosophical reflection, Modern Mind Unveiled deepens our understanding of both the strengths and vulnerabilities of the human mind. It invites readers to see medicine not merely as a science of intervention, but as a discipline of perception, empathy, and awareness—an approach essential for thoughtful practice in the 21st century.
The Six Core Themes
I. Human Behavior and Cognitive Patterns
Examining the often-unconscious mechanisms that guide human choice—how we navigate uncertainty, balance logic with intuition, and adapt through seemingly irrational behavior.
II. Emotion, Relationships, and Social Dynamics
Investigating the structure of empathy, the psychology of belonging, and the influence of abundance and selectivity on modern social connection.
III. Technology, Media, and the Digital Mind
Analyzing how digital environments reshape cognition, attention, and identity—exploring ideas such as gamification, information overload, and cognitive “nutrition” in online spaces.
IV. Cognitive Bias, Memory, and Decision Architecture
Exploring how memory, prediction, and self-awareness interact in decision-making, and how external systems increasingly serve as extensions of thought.
V. Habits, Health, and Psychological Resilience
Understanding how habits sustain or erode well-being—considering anhedonia, creative rest, and the restoration of mental balance in demanding professional and personal contexts.
VI. Philosophy, Meaning, and the Self
Reflecting on continuity of identity, the pursuit of coherence, and the construction of meaning amid existential and informational noise.
Keywords
Cognitive Science • Behavioral Psychology • Digital Media • Emotional Regulation • Attention • Decision-Making • Empathy • Memory • Bias • Mental Health • Technology and Identity • Human Behavior • Meaning-Making • Social Connection • Modern Mind
Video Section 

