MS Phenotypes: Why the Current Classification System May Be Failing Patients
Key Takeaways
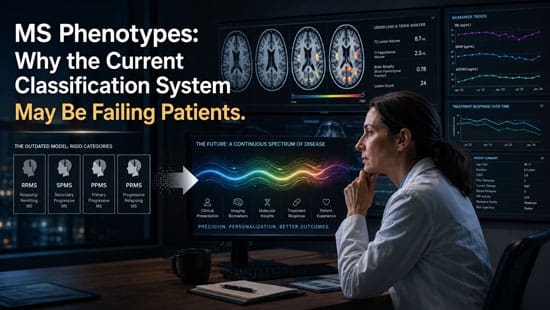
The traditional classification system for multiple sclerosis, established in 1996 by the United States National Multiple Sclerosis Society, continues to shape clinical practice, therapeutic decision making, and clinical trial design nearly three decades later. This framework categorized multiple sclerosis into four clinical phenotypes: relapsing remitting multiplef sclerosis, secondary progressive multiple sclerosis, primary progressive multiple sclerosis, and progressive relapsing multiple sclerosis. At the time, this structure provided an important foundation for understanding disease evolution and standardizing communication among clinicians and researchers. However, advances in neuroimaging, immunology, molecular biology, and biomarker research have increasingly exposed the limitations of this clinically based model.
The original classification system was derived largely from observable clinical patterns and expert consensus rather than objective biological evidence. Disease categorization relied heavily on visible symptoms such as relapses, disability progression, and patterns of neurological decline. While clinically practical, this approach assumed that disease activity could be adequately inferred from external manifestations alone. Contemporary evidence now demonstrates that this assumption is fundamentally incomplete. Multiple sclerosis is not a disease defined solely by episodic relapses or progressive disability, but rather a biologically heterogeneous and continuously evolving neuroinflammatory condition characterized by overlapping pathological processes occurring simultaneously within the central nervous system.
One of the most significant shortcomings of the current phenotype based system is its inability to detect or adequately represent the substantial proportion of disease progression that occurs independently of overt clinical relapses. Emerging evidence suggests that as much as 90 percent of neurological deterioration in multiple sclerosis may occur through mechanisms unrelated to clinically apparent attacks. This phenomenon, often referred to as progression independent of relapse activity, highlights the disconnect between visible symptoms and underlying tissue injury. As a result, many patients categorized as clinically stable continue to accumulate irreversible neuroaxonal damage despite the absence of obvious disease activity.
This discrepancy has major implications for patient care. Reliance on relapse frequency and overt disability progression often delays recognition of disease worsening and contributes to suboptimal treatment decisions. Patients who appear stable according to traditional clinical criteria may in fact experience ongoing inflammatory and neurodegenerative activity that remains undetected using conventional assessment methods. Consequently, the current classification system risks underestimating disease burden and delaying escalation to more effective therapies.
Recent advances in biomarker research are fundamentally reshaping understanding of multiple sclerosis biology. Biomarkers such as serum neurofilament light chain have emerged as highly sensitive indicators of neuroaxonal injury, providing measurable evidence of ongoing brain and spinal cord damage even during periods of clinical remission. Elevated serum neurofilament levels correlate with disease activity, lesion burden, brain atrophy, and long term disability progression, offering a dynamic and objective measure of tissue injury that extends beyond traditional clinical observation.
Similarly, advanced magnetic resonance imaging techniques have revealed pathological processes previously invisible to routine imaging approaches. Paramagnetic rim lesions, identified using susceptibility sensitive imaging sequences, are increasingly recognized as markers of chronic active inflammation within the central nervous system. These lesions reflect persistent innate immune activation and smoldering inflammatory activity that can continue for years, contributing to gradual neurological decline. Importantly, such pathological changes may occur in patients classified within any traditional phenotype category, further challenging the notion that relapsing and progressive forms of multiple sclerosis represent distinct biological entities.
Current evidence increasingly supports the concept that inflammatory activity, demyelination, neurodegeneration, remyelination failure, and compartmentalized immune responses coexist throughout the disease continuum. Rather than occurring sequentially, these processes interact dynamically from the earliest stages of disease. Smoldering inflammation and neurodegenerative changes may begin long before clinical symptoms become apparent, suggesting that irreversible tissue injury is already underway during so called preclinical phases of multiple sclerosis. This recognition underscores the urgent need for earlier detection strategies and proactive intervention before significant neurological reserve is lost.
The implications of these discoveries extend beyond disease classification into the broader philosophy of multiple sclerosis management. The traditional model of categorizing patients into rigid subtypes increasingly appears scientifically outdated and clinically insufficient. Instead, many experts now advocate for a transition toward biologically informed, personalized frameworks that characterize disease according to underlying mechanisms rather than outward clinical appearance alone. Such an approach would integrate imaging biomarkers, molecular markers, immunological profiling, and measures of neurodegeneration to generate a more accurate representation of disease activity and prognosis.
This shift toward precision medicine has the potential to transform therapeutic decision making. Rather than applying standardized treatment algorithms based on phenotype labels, clinicians may increasingly tailor interventions according to individual biological signatures, rates of neuroaxonal injury, inflammatory burden, and risk of progression. Biomarker driven approaches could allow earlier identification of aggressive disease, more accurate monitoring of treatment response, and timely escalation of therapy before irreversible disability accumulates.
At the same time, this evolving framework presents important challenges. Standardization of biomarker interpretation, accessibility of advanced imaging technologies, integration of molecular diagnostics into routine care, and validation of new classification models remain ongoing areas of research. Additionally, redefining multiple sclerosis according to biological processes will require substantial adaptation in clinical trial design, regulatory frameworks, and medical education.
Nevertheless, the growing body of evidence strongly suggests that the future of multiple sclerosis care lies in moving beyond rigid categorical definitions toward a more comprehensive understanding of disease biology. The transition from symptom based classification to biomarker informed characterization represents a fundamental paradigm shift in neurology. In this emerging model, treatment decisions are guided not solely by what clinicians can observe externally, but by a deeper understanding of the pathological processes occurring within the brain and spinal cord. As biomarker science and neuroimaging technologies continue to advance, this biology driven approach offers the possibility of earlier intervention, more individualized care, and ultimately improved long term outcomes for patients living with multiple sclerosis.
The Current MS Phenotype Classification System Explained
Relapsing-Remitting MS (RRMS) Definition
Approximately 85% of individuals receive an initial MS diagnosis with the relapsing-remitting form. This ms phenotype manifests through distinct episodes of neurological symptoms, termed relapses or exacerbations, that persist for at least 24 hours. Between these episodes, patients experience periods of partial or complete recovery known as remissions. The inflammatory process drives these relapses, characterized by new focal neurologic signs caused by demyelination in the central nervous system. MS average age of onset typically falls within the 20s and 30s, with women affected twice as frequently as men.
During remission periods, symptoms may partly or completely resolve, though relapses can leave lasting effects. Around half of all relapses produce lingering problems despite recovery. The body’s ability to repair myelin damage diminishes with successive relapses, leading to accumulation of disability even between acute episodes. MRI scans during active disease reveal new and gadolinium-enhancing lesions that correspond with inflammatory infiltrates and blood-brain barrier disruption.
Secondary Progressive MS (SPMS) Definition
Most patients with relapsing-remitting disease eventually transition to secondary progressive MS, where neurologic function declines independent from clinically apparent relapses. The median time from initial symptoms to SPMS conversion reaches approximately 20 years in untreated individuals, though this ranges from 1 to 51 years. Before disease-modifying therapies became available, roughly 60-70% of RRMS patients transformed into SPMS within 20-25 years. Contemporary treatment approaches have reduced this conversion rate and extended the time to progression.
SPMS presents as insidious disability worsening that continues regardless of relapse activity. However, patients with SPMS can still experience relapses superimposed on the progressive course. The inflammation that characterizes RRMS gradually lessens over time in SPMS, yet disease activity persists. Clear clinical, imaging, immunologic, or pathologic criteria marking the transition from RRMS to SPMS have not been established, creating diagnostic challenges for clinicians attempting to identify this conversion point.
Primary Progressive MS (PPMS) Definition
Primary progressive MS affects approximately 10-15% of the MS population and follows a distinct trajectory from disease onset. Neurologic dysfunction accumulates steadily from the first symptom appearance without the early relapses that define RRMS. The condition affects men and women equally, contrasting with the female predominance seen in relapsing forms. Patients typically receive diagnosis between ages 37 and 43 years, older than the typical RRMS presentation.
Motor deficits and sensory impairments with myelopathy patterns constitute the most common initial manifestations, frequently coupled with bowel and bladder dysfunction. Less than 30% of PPMS patients experience distinct relapses throughout their disease course. MRI findings show fewer and smaller brain lesions compared to RRMS, though spinal cord lesions appear more frequently. Gadolinium-enhancing lesions occur much less commonly, reflecting reduced inflammatory activity. In contrast, diffuse brain and spinal cord atrophy develops more extensively and progresses faster than in relapsing forms.
The 1996 Framework and Its Original Purpose
The original ms clinical phenotypes emerged from an international survey of MS clinicians that utilized clinical information alone to describe four subtypes of ms: relapsing-remitting, primary progressive, secondary progressive, and progressive-relapsing. This standardized classification system aimed to provide consistent terminology for communication between clinicians and researchers studying ms disease course patterns.
The framework developers acknowledged the need for future modifications as imaging modalities and biomarkers advanced. By 2013, experts revised these descriptors to incorporate disease activity measures based on clinical relapses, disability progression, and MRI findings. The revision eliminated progressive-relapsing MS as a separate category and introduced activity modifiers for all clinical phenotypes of ms. These changes reflected growing recognition that the original distinctions among subtypes remained imprecise and failed to capture integrated clinical and imaging assessments.
Why Clinical Phenotypes Fail to Capture MS Disease Biology
Symptoms Don’t Reflect Underlying Pathology
Current ms phenotypes group patients based on similar clinical presentations although they might have different underlying disease-driving pathologic processes. The classification remains agnostic to key pathologic processes including cortical demyelination, chronic perilesional white matter inflammation, neuroaxonal degeneration, and remyelination. Disease activity measured through clinical relapses and MRI lesions provides incomplete information about inflammatory activity and fails to adequately account for neurodegenerative disease progression.
Silent MS activity occurs without visible symptoms, detectable only through brain imaging. Indeed, studies observed cognitive deterioration amongst patients achieving NEDA-3 status despite absence of relapses, disability progression, or radiological activity. In up to 90% of people with relapsing MS, disability progression happens without relapses, despite treatment. This phenomenon, termed progression independent of relapse activity, demonstrates that clinical symptoms poorly correlate with underlying biological processes.
Multiple Disease Processes Occur Simultaneously
Several pathologic processes can be at play to differing degrees at once and have similar clinical manifestations. Inflammatory processes, both acute and compartmentalized within the central nervous system, occur alongside neurodegeneration, oxidative stress, mitochondrial dysfunction, and remyelination failure to different degrees throughout ms disease course rather than in a predictable sequence. These processes vary markedly between patients currently classified in the same disease categories and may even be present before clinical manifestations appear.
Chronic active lesions, characterized by slowly expanding inflammation with paramagnetic rim patterns, represent ongoing disease activity that traditional phenotyping cannot distinguish from quiescent lesions. Subpial cortical injury and periventricular thalamic damage occur through smoldering processes independent of focal relapse biology.
Patients Switch Between Phenotypes
The conversion of relapsing-remitting to secondary progressive MS represents a gradual process rather than a sharp threshold determined by event-based measures. An interim period of several years duration may exist between RRMS and clearly established SPMS. SPMS represents a retrospective diagnosis, with mean duration of diagnostic uncertainty reaching 2.9 years. In 70% of cases, SPMS diagnosis was only established when EDSS reached 6.0 or higher.
Approximately 30-50% of untreated RRMS patients convert to SPMS within 10-15 years after disease onset. However, this transition point lacks clear clinical, imaging, immunologic, or pathologic criteria, creating diagnostic challenges for determining when conversion occurs.
Age and MS Disease Course Misconceptions
Aging and MS share many overlapping symptoms including slower movement, reduced stamina, memory changes, and muscle stiffness. The nervous system’s ability to compensate for old MS-related damage may decline over time, making longstanding symptoms feel worse even without new disease activity. This phenomenon, called pseudo-progression, occurs when symptoms worsen but no new inflammation or relapse exists.
Biological aging closely links to MS progression patterns. Muscles already affected by MS may weaken faster with age-related muscle loss, while balance problems become more noticeable as reflexes slow. These overlapping factors make distinguishing between normal aging and MS progression challenging even for experienced clinicians.
Emerging Biomarkers Revealing the True Nature of MS
Serum Neurofilament Light Chain (sNfL) Levels
Neurofilament light chain reflects neuroaxonal loss and serves as a marker of neuronal damage released during injury or disease. This structural protein becomes detectable in peripheral blood following axonal injury, with elevated sNfL levels indicating active neuroaxonal damage. The correlation between sNfL and gadolinium-enhancing lesions demonstrates its value as a disease activity marker, though specificity exceeds sensitivity. In one analysis, only 28% to 43% of patients with active lesions showed sNfL elevation, despite specificity ranging from 82% to 92%.
The temporal relationship between sNfL elevation and radiological activity reveals important limitations. Peak sNfL increases occur an average of two months after the first gadolinium-enhancing lesion appears on MRI. Elevations averaging 32% were observed within three months following the appearance of enhancing lesions. Furthermore, sNfL captures acute inflammation associated with relapses and new MRI lesions rather than the lower-grade inflammation responsible for progressive disability.
Age-adjusted z-scores above 1.5 predict three times the risk for disease activity in the following year. Higher baseline sNfL levels correlate with increased odds of reaching EDSS scores of 6.0 or higher over eight years, with patients in the highest baseline category worsening at an annual EDSS rate of 0.16. Persistently high sNfL despite treatment associates with worse MRI outcomes at four years.
MRI Findings: Paramagnetic Rim Lesions and Chronic Active Lesions
Paramagnetic rim lesions on susceptibility-weighted MRI sequences indicate unresolved inflammation at demyelinated white matter lesion peripheries. These lesions appear as dark ring-like structures reflecting iron accumulation in microglia. At least one PRL on brain MRI demonstrates 90% specificity and 86% sensitivity for diagnosing MS in adults presenting for evaluation. A threshold of two or more PRLs increases specificity to 95% but reduces sensitivity to 59%.
Chronic active lesions constitute 20% to 40% of white matter lesions and exhibit persistent low-level inflammation with axonal damage and demyelination. The iron-laden activated microglia forms a paramagnetic rim visible through susceptibility-weighted imaging. The number of PRLs increases throughout ms disease course and correlates with cognitive impairment, disability, and progression across all ms clinical phenotypes. Patients with four or more PRLs face substantially higher odds of disability worsening. Each additional year reduction in symptom duration increases PRL detection odds by 28%.
Brain Volume Loss and Thalamic Atrophy Measurements
Brain atrophy rates in MS patients reach 0.5% to 1.35% annually, substantially exceeding the 0.1% to 0.3% observed in healthy adults. Thalamic volume measures 16.8% lower in MS populations compared to controls. This regional atrophy shows moderate to strong correlations with cognitive performance across all domains, with correlation coefficients ranging from 0.506 to 0.724. Every unit decrease in baseline thalamus volume increases odds of disability progression over five years by 2.4-fold.
The Gap Between Biological Activity and Clinical Symptoms
Smoldering disease encompasses chronic pathobiological processes beyond focal inflammation that lead to clinical worsening and begins before clinical symptom development. Patients exhibit disability accrual despite absence of new or enlarging T2-weighted or T1-weighted lesions. Active inflammation and demyelination persist in the central nervous system of patients with terminal or end-stage MS. The emerging consensus recognizes that patients with all subtypes of ms share the same fundamental pathology, with inflammatory and neurodegenerative processes occurring simultaneously.
From Categories to Spectrum: The Biological Phenotyping Approach
Disease Activity Markers vs Clinical Relapses
Active disease encompasses both clinical relapses and new or enlarging inflammatory central nervous system lesions detected on MRI. However, biological disease activity extends beyond these observable events. Patients at baseline with clear relapses demonstrated median sNfL of 14.6 pg/mL compared to 9.5 pg/mL in those with other causes. This distinction reveals how fluid biomarkers capture ongoing neuroaxonal injury independent of clinical presentation. In contrast to relapse-based assessments, progression independent of relapse activity affects up to 87% of patients despite relatively early ms disease course with mean duration of approximately six years.
Smoldering MS and Subclinical Progression
Smoldering processes reflect chronic pathobiological mechanisms beyond focal inflammation, characterized by slowly expanding chronic active lesions, ongoing axonal degeneration, and widespread microglial activation. Analysis of 7,562 brain lesions from 182 post-mortem cases revealed that 57% were chronic active lesions. Active or chronic active lesions appeared in 78% of cases across all clinical phenotypes of ms. For this reason, smoldering represents an umbrella term encompassing compartmentalized inflammation and neurodegenerative mechanisms rather than purely non-inflammatory processes.
The Functional Reserve Model
At disease onset, patients possess varying degrees of reserve, conceptualized as the dynamic availability of cerebral resources supporting functional capacity. Baseline reserve depletes through deleterious factors while protective factors preserve it. Larger intracranial volume, a proxy for neuronal and synaptic count, reduces risk for cognitive or physical decline. This model explains why persons with similar disease burden exhibit vastly different functional outcomes, with subclinical disease potentially progressing for years while high functional reserve masks lesion effects.
Early-Stage vs Late-Stage Inflammatory Patterns
The transition to progressive ms disease course appears age-dependent, with the age of transition remaining around the forties despite lower conversion percentages. Clinical features become less inflammatory with age, showing decreased relapses and new MRI lesions while progressive risk increases proportionally.
How the Current System Impacts Patient Care and Treatment Decisions
Delayed Diagnosis Due to Rigid Criteria
Diagnostic delay affects 52.7% of patients, with median time between first clinical symptoms and diagnosis reaching 4.4 months. Physician-dependent factors account for roughly one quarter of delays, with 15.1% of patients receiving false negative diagnoses from neurologists. Even relatively short delays associate with unfavorable outcomes, including greater EDSS scores, increased lesion numbers on brain MRI, and elevated neurofilament light chain levels at diagnosis. Progression is often diagnosed based on ambulation difficulties, which can be arbitrary and may cause essential changes in care to be postponed.
Treatment Selection Based on Outdated Categories
Current disease-modifying treatments predominantly reduce relapses, making the distinction between relapsing-remitting and progressive courses useful for identifying patients who respond to therapies. Inasmuch as treatment efficacy varies by phenotype, siponimod and rituximab demonstrate effectiveness in active progressive but not in nonactive progressive patients. Notwithstanding these distinctions, the classification considers only white matter lesion formation while remaining agnostic to cortical demyelination, chronic perilesional inflammation, and neuroaxonal degeneration.
Clinical Trial Design Limitations
MS randomized controlled trials traditionally focus on homogenous populations, often restricted to ages 18-55 years, weakening external validity. Average treatment effects do not account for medical comorbidities, social determinants of health, or genetic differences. According to conventional trial design, subgroup analyzes suffer from smaller sample sizes with lower statistical power.
The Need for Individualized Treatment Approaches
MS heterogeneity demands personalized treatment approaches. Identifying reliable biomarkers and disease subtypes requires expensive, sophisticated technologies. Equally important, demographic, clinical, and radiographic covariates including sex, race, age at onset, disease duration, MRI lesion burden, and disability level warrant consideration when selecting therapies.
The traditional MS phenotype classification system fails to capture the complex biological reality of disease progression. Clinical symptoms poorly correlate with underlying pathological processes including compartmentalized inflammation, neurodegeneration, and smoldering disease activity. As a result, patients face delayed diagnosis and suboptimal treatment selection based on outdated categorical distinctions. Emerging biomarkers such as serum neurofilament light chain, paramagnetic rim lesions, and brain atrophy measurements reveal disease biology beyond what clinical observation detects. The field must transition from rigid phenotypic categories toward individualized, biomarker-driven treatment approaches. All things considered, this paradigm shift represents essential progress in addressing MS heterogeneity and improving patient outcomes across the disease spectrum.
FAQs
Q1. What are the four main types of multiple sclerosis? The four main classifications are relapsing-remitting MS (RRMS), which affects about 85% of patients initially; secondary progressive MS (SPMS), which many RRMS patients eventually develop; primary progressive MS (PPMS), affecting 10-15% of patients with steady progression from onset; and progressive-relapsing MS, though this last category was eliminated in the 2013 revision of the classification system.
Q2. Why is the current MS classification system considered inadequate? The current system groups patients based on clinical symptoms rather than underlying biological processes. It fails to capture the complexity of MS because multiple disease processes occur simultaneously, symptoms don’t reflect actual pathology, and patients can switch between phenotypes. Additionally, the system cannot detect “smoldering” disease activity that progresses without visible symptoms.
Q3. What are paramagnetic rim lesions and why are they important? Paramagnetic rim lesions (PRLs) are chronic active lesions visible on specialized MRI scans that indicate ongoing inflammation at the edges of demyelinated areas. They appear as dark ring-like structures and are highly specific for MS diagnosis. The presence of PRLs correlates with cognitive impairment, disability progression, and worse outcomes across all MS types, making them valuable biomarkers for disease activity.
Q4. How does serum neurofilament light chain help monitor MS disease activity? Serum neurofilament light chain (sNfL) is a blood biomarker that reflects active nerve damage in MS. Elevated levels indicate ongoing neuroaxonal injury and correlate with MRI lesion activity and relapses. Higher baseline sNfL levels predict increased risk of disability progression, making it useful for monitoring disease activity and treatment response beyond what clinical symptoms alone can reveal.
Q5. What is the difference between MS progression and normal aging symptoms? MS progression and normal aging share overlapping symptoms including slower movement, memory changes, and muscle stiffness, making them difficult to distinguish. Age-related changes can worsen existing MS symptoms without new disease activity—a phenomenon called pseudo-progression. The nervous system’s declining ability to compensate for old MS damage over time can make longstanding symptoms feel worse even when no new inflammation is occurring.

References
[2] – https://www.hopkinsmedicine.org/health/conditions-and-diseases/multiple-sclerosis-ms/relapsing-remitting-multiple-sclerosis
[3] – https://www.neurology.org/doi/10.1212/WNL.0000000000012323
[4] – https://www.mssociety.org.uk/about-ms/types-of-ms/relapsing-remitting-ms
[5] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12405697/
[6] – https://pmc.ncbi.nlm.nih.gov/articles/PMC11787267/
[7] – https://www.nationalmssociety.org/understanding-ms/what-is-ms/types-of-ms/secondary-progressive-ms
[8] – https://pmc.ncbi.nlm.nih.gov/articles/PMC11354232/
[9] – https://www.mssociety.org.uk/about-ms/types-of-ms/primary-progressive-ms
[10] – https://consultqd.clevelandclinic.org/lets-move-from-categorizing-ms-by-clinical-phenotype-to-underlying-disease-mechanisms
[11] – https://pmc.ncbi.nlm.nih.gov/articles/PMC3523020/
[12] – https://practicalneurology.com/diseases-diagnoses/ms-immune-disorders/evaluating-heterogeneous-treatment-effects-in-pursuit-of-personalized-multiple-sclerosis-care/33141/
[13] – https://pmc.ncbi.nlm.nih.gov/articles/PMC8793117/
[14] – https://www.sciencedirect.com/science/article/abs/pii/S0166223623002655
[15] – https://www.thelancet.com/journals/ebiom/article/PIIS2352-3964(24)00005-7/fulltext
[16] – https://www.sciencedirect.com/science/article/abs/pii/S2211034825002925
[17] – https://consultqd.clevelandclinic.org/could-serum-neurofilament-light-chain-level-help-guide-ms-management
[18] – https://practicalneurology.com/diseases-diagnoses/ms-immune-disorders/progressive-multiple-sclerosis-functional-anatomic-and-biologic-tools-to-assess-disability-progression-and-improve-patient-outcomes/33143/
[19] – https://www.nationalmssociety.org/news-and-magazine/news/study-shows-blood-test-in-helping-predict-future-ms
[20] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12185222/
[21] – https://consultqd.clevelandclinic.org/paramagnetic-rim-lesions-for-ms-diagnosis-at-first-presentation
[22] – https://www.jmcp.org/doi/10.18553/jmcp.2025.24294
[23] – https://www.sciencedirect.com/science/article/pii/S0035378726004972
[24] – https://pubmed.ncbi.nlm.nih.gov/17875909/
[25] – https://www.frontiersin.org/journals/neurology/articles/10.3389/
fneur.2020.00606/full
[26] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12112593/
[27] – https://pmc.ncbi.nlm.nih.gov/articles/PMC6719722/
[28] – https://pmc.ncbi.nlm.nih.gov/articles/PMC8058428/
[29] – https://www.neurologylive.com/view/ms-classification-and-impact-on-care
[30] – https://pmc.ncbi.nlm.nih.gov/articles/PMC9427000/
[31] – https://www.neurologyletters.com/article_170305.html
Recent Articles


Integrative Perspectives on Cognition, Emotion, and Digital Behavior

Sleep-related:
Longevity/Nutrition & Diet:
Philosophical / Happiness / Social:
Other:
Modern Mind Unveiled
Developed under the direction of David McAuley, Pharm.D., this collection explores what it means to think, feel, and connect in the modern world. Drawing upon decades of clinical experience and digital innovation, Dr. McAuley and the GlobalRPh initiative translate complex scientific ideas into clear, usable insights for clinicians, educators, and students.
The series investigates essential themes—cognitive bias, emotional regulation, digital attention, and meaning-making—revealing how the modern mind adapts to information overload, uncertainty, and constant stimulation.
At its core, the project reflects GlobalRPh’s commitment to advancing evidence-based medical education and clinical decision support. Yet it also moves beyond pharmacotherapy, examining the psychological and behavioral dimensions that shape how healthcare professionals think, learn, and lead.
Through a synthesis of empirical research and philosophical reflection, Modern Mind Unveiled deepens our understanding of both the strengths and vulnerabilities of the human mind. It invites readers to see medicine not merely as a science of intervention, but as a discipline of perception, empathy, and awareness—an approach essential for thoughtful practice in the 21st century.
The Six Core Themes
I. Human Behavior and Cognitive Patterns
Examining the often-unconscious mechanisms that guide human choice—how we navigate uncertainty, balance logic with intuition, and adapt through seemingly irrational behavior.
II. Emotion, Relationships, and Social Dynamics
Investigating the structure of empathy, the psychology of belonging, and the influence of abundance and selectivity on modern social connection.
III. Technology, Media, and the Digital Mind
Analyzing how digital environments reshape cognition, attention, and identity—exploring ideas such as gamification, information overload, and cognitive “nutrition” in online spaces.
IV. Cognitive Bias, Memory, and Decision Architecture
Exploring how memory, prediction, and self-awareness interact in decision-making, and how external systems increasingly serve as extensions of thought.
V. Habits, Health, and Psychological Resilience
Understanding how habits sustain or erode well-being—considering anhedonia, creative rest, and the restoration of mental balance in demanding professional and personal contexts.
VI. Philosophy, Meaning, and the Self
Reflecting on continuity of identity, the pursuit of coherence, and the construction of meaning amid existential and informational noise.
Keywords
Cognitive Science • Behavioral Psychology • Digital Media • Emotional Regulation • Attention • Decision-Making • Empathy • Memory • Bias • Mental Health • Technology and Identity • Human Behavior • Meaning-Making • Social Connection • Modern Mind
Video Section 

