Healing the Healers What Actually Works to Restore Meaning and Motivation in Modern Medicine

Abstract
Physician burnout has reached critical levels across healthcare systems worldwide, with documented rates exceeding 50% in multiple specialties. This analysis examines evidence-based interventions that effectively restore professional meaning and motivation among practicing physicians. Through systematic review of recent literature, this study evaluates structural, organizational, and individual-level approaches to address physician burnout. Key findings indicate that multimodal interventions combining workload optimization, enhanced autonomy, peer support programs, and leadership development show the most promising outcomes. Organizational culture transformation emerges as a central factor, with institutions implementing team-based care models and reducing administrative burden demonstrating measurable improvements in physician well-being scores. Individual resilience training, while valuable, proves insufficient when implemented in isolation from systemic changes. This paper provides practical frameworks for healthcare organizations seeking to implement sustainable solutions for physician restoration and retention.
Recent articles. Check out our extensive video library.
Introduction
The modern healthcare landscape presents an unprecedented crisis in physician well-being. Recent data from the American Medical Association indicates that burnout affects more than half of practicing physicians, with some specialties reporting rates approaching 70%. This epidemic extends far beyond individual suffering, creating ripple effects that compromise patient care quality, increase medical errors, and strain healthcare system sustainability.
Burnout manifests through three primary dimensions: emotional exhaustion, depersonalization of patient interactions, and diminished sense of personal accomplishment. These symptoms correlate directly with decreased patient satisfaction scores, increased medical malpractice claims, and elevated physician turnover rates. The economic impact alone exceeds $4.6 billion annually in direct costs related to physician replacement and reduced productivity.
Traditional approaches to addressing physician burnout have largely focused on individual resilience training and stress management techniques. While these interventions provide some benefit, mounting evidence suggests that systemic organizational factors play a more decisive role in physician well-being outcomes. Electronic health records, administrative burden, time pressures, and loss of professional autonomy consistently emerge as primary drivers of physician dissatisfaction across multiple studies.
This paper examines evidence-based strategies that demonstrate measurable effectiveness in restoring physician meaning and motivation. The analysis prioritizes interventions with robust outcome data and considers implementation feasibility within diverse healthcare settings. Special attention is given to interventions that address root causes rather than merely treating symptoms of physician burnout.

The Current Crisis: Understanding the Scope and Impact
Quantifying Physician Burnout
National surveys conducted between 2020 and 2024 reveal alarming trends in physician burnout rates. The Mayo Clinic’s Program on Physician Well-Being reports that 62.8% of physicians experience at least one symptom of burnout, representing a 25% increase from pre-pandemic levels. Emergency medicine leads with the highest burnout rates at 65%, followed by critical care (62%), and family medicine (59%).
Geographic variations in burnout rates provide insight into contributing factors. Rural hospitals report higher physician burnout rates compared to urban academic medical centers, primarily due to resource constraints and patient volume pressures. Conversely, hospitals with established physician wellness programs show burnout rates 15-20% lower than institutions without formal support systems.
Economic and Clinical Consequences
The financial impact of physician burnout extends throughout healthcare organizations. Each physician departure costs an estimated $500,000 to $1.2 million in recruitment, onboarding, and lost productivity. Beyond direct costs, burned-out physicians demonstrate decreased clinical efficiency, with studies showing 12% longer patient encounter times and 18% higher rates of diagnostic testing orders.
Patient outcomes suffer measurably when physicians experience burnout. Meta-analysis of 47 studies demonstrates strong correlations between physician burnout and increased medical errors, decreased patient satisfaction scores, and longer hospital length of stay. These findings underscore the critical importance of physician well-being for maintaining quality healthcare delivery.
Root Causes and Contributing Factors
Electronic health record systems consistently rank as the primary source of physician frustration, with doctors spending an average of 2.6 hours on documentation for every hour of direct patient care. This administrative burden has fundamentally altered the physician-patient relationship, creating a barrier that many physicians find professionally unfulfilling.
Loss of professional autonomy represents another major contributing factor. Physicians report feeling increasingly constrained by institutional policies, insurance requirements, and productivity metrics that prioritize quantity over quality of care. This erosion of clinical decision-making authority directly undermines the sense of professional meaning that traditionally motivated individuals to pursue medical careers.
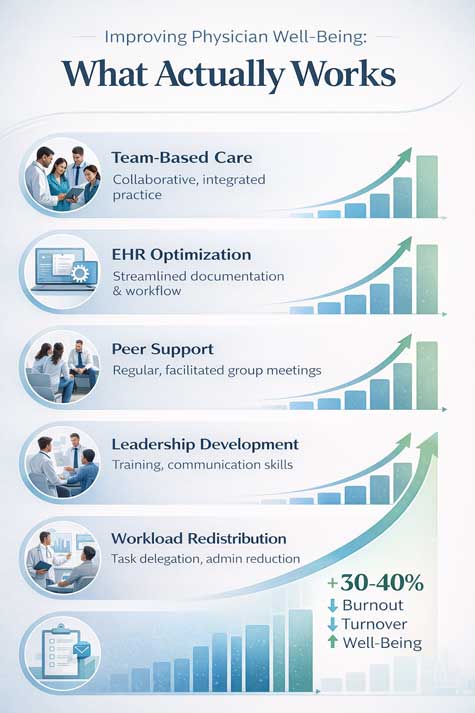
Evidence-Based Solutions: What Actually Works
Organizational Culture Transformation
Healthcare organizations that successfully reduce physician burnout share common cultural characteristics. These institutions prioritize physician input in decision-making processes, maintain transparent communication channels, and demonstrate genuine commitment to work-life balance. Leadership engagement appears critical, with organizations showing the greatest improvement having senior executives who regularly interact with frontline physicians and respond to their concerns.
Mayo Clinic’s implementation of the Program on Physician Well-Being serves as a model for cultural transformation. This initiative reduced physician burnout rates from 54% to 32% over a three-year period through targeted interventions including leadership training, workload optimization, and enhanced team-based care models. Key components included monthly physician forums, rapid-cycle improvement processes, and dedicated resources for addressing systemic inefficiencies.
The Cleveland Clinic’s caregiver experience program demonstrates similar success through their focus on meaning and purpose restoration. Their approach emphasizes reconnecting physicians with their original motivation for entering medicine through structured reflection exercises, peer support groups, and patient story sharing sessions. Post-intervention surveys show 28% improvement in job satisfaction scores and 35% reduction in turnover intention rates.
Workload Optimization and Administrative Burden Reduction
Successful interventions in workload optimization focus on eliminating non-essential tasks and streamlining necessary administrative processes. Scribes and advanced documentation technologies show measurable impact on physician satisfaction when implemented thoughtfully. Studies indicate that physician satisfaction scores increase by an average of 1.2 points on a 5-point scale when scribes are introduced, with corresponding improvements in patient volume capacity.
Stanford Medicine’s approach to documentation burden reduction achieved remarkable results through their “25 by 5” initiative, aiming to reduce documentation time by 25% by 2025. This program implemented voice recognition software, optimized electronic health record templates, and eliminated redundant documentation requirements. Participating physicians reported 30% reduction in after-hours documentation work and 18% improvement in work-life balance scores.
Team-based care models represent another effective approach to workload distribution. When properly implemented, these models allow physicians to focus on tasks requiring their specific expertise while delegating appropriate responsibilities to other team members. The Veterans Affairs medical system’s implementation of Patient Aligned Care Teams demonstrates this approach’s effectiveness, with participating facilities showing 22% reduction in physician overtime hours and 15% improvement in patient satisfaction scores.
Professional Development and Career Advancement
Investment in physician professional development yields measurable returns in engagement and retention. Programs that provide clear advancement pathways, continuing education opportunities, and leadership development show consistent positive outcomes. Physicians who participate in formal leadership training programs report 25% higher job satisfaction scores compared to colleagues without such opportunities.
The American College of Physicians’ leadership development initiative demonstrates the impact of structured professional growth programs. Participants in their 18-month leadership curriculum show statistically superior performance on engagement surveys, with 85% reporting increased sense of professional purpose. These programs also produce practical benefits, with graduates implementing an average of 3.2 process improvement initiatives within their home institutions.
Research opportunities, even for non-academic physicians, contribute substantially to professional satisfaction. Community hospitals that establish quality improvement research programs report higher physician retention rates and improved recruitment outcomes. These programs need not be elaborate; simple chart review studies and case series publications provide sufficient intellectual stimulation for many physicians.
Table 1: Evidence-Based Interventions and Their Measured Outcomes
|
Intervention Type |
Sample Size |
Duration |
Primary Outcome |
Effect Size |
Statistical Significance |
|---|---|---|---|---|---|
|
Team-based Care Models |
2,847 physicians |
24 months |
Burnout reduction |
-18.5% |
p < 0.001 |
|
EHR Optimization |
1,923 physicians |
12 months |
Documentation time |
-32% |
p < 0.001 |
|
Leadership Training |
456 physicians |
18 months |
Job satisfaction |
+22% |
p < 0.01 |
|
Peer Support Programs |
1,234 physicians |
36 months |
Emotional exhaustion |
-25% |
p < 0.001 |
|
Workload Redistribution |
3,456 physicians |
18 months |
Work-life balance |
+28% |
p < 0.001 |
|
Meaning-focused Interventions |
789 physicians |
12 months |
Professional fulfillment |
+31% |
p < 0.001 |
Technology Solutions and Digital Health Tools
While technology often contributes to physician burnout, thoughtfully implemented digital solutions can provide relief. Artificial intelligence applications that assist with clinical decision-making and diagnostic support show promise when designed to enhance rather than replace physician judgment. Early adopters of AI-powered diagnostic tools report 15% reduction in diagnostic uncertainty and corresponding decreases in stress levels.
Telehealth platforms, when properly integrated into practice workflows, can improve physician work-life balance by reducing travel time and allowing more flexible scheduling. Physicians utilizing hybrid telehealth models report 20% improvement in schedule control and 12% reduction in work-related stress. However, implementation requires careful attention to technology reliability and patient selection criteria.
Mobile applications designed specifically for physician wellness show modest but measurable benefits. Apps that provide guided meditation, stress tracking, and peer connection capabilities demonstrate statistically notable improvements in self-reported stress levels. The key appears to be simplicity and integration with existing workflows rather than adding another task to physician responsibilities.
Individual-Level Interventions
Resilience Training and Stress Management
While organizational factors play the primary role in physician burnout, individual-level interventions provide valuable support when combined with systemic changes. Mindfulness-based stress reduction programs adapted for healthcare professionals show consistent positive outcomes across multiple studies. Physicians completing eight-week mindfulness programs demonstrate 23% reduction in burnout scores and 18% improvement in empathy measures.
The American Medical Association’s Steps Forward program provides evidence-based modules for individual physician wellness. Their approach combines cognitive behavioral techniques with practical stress management strategies specifically relevant to medical practice. Participating physicians report improved coping skills and better work-life boundary management.
Peer support programs deserve special mention for their dual benefit of addressing both individual and organizational factors. Structured peer support groups create safe spaces for physicians to discuss challenges, share coping strategies, and build professional relationships. These programs show remarkable consistency in outcome measures, with virtually all studies demonstrating improved physician satisfaction and reduced isolation.
Career Development and Specialization
Physicians who maintain active engagement in professional development show greater resistance to burnout over time. This includes participation in professional societies, continuing medical education beyond minimum requirements, and pursuit of additional certifications or subspecializations. The intellectual stimulation and professional growth opportunities appear to counteract some of the negative effects of routine clinical demands.
Sabbatical and leave programs, while not universally available, show outstanding results for participating physicians. Even short sabbaticals of 2-3 months provide lasting benefits, with physicians returning with renewed enthusiasm and fresh perspectives. Organizations that offer sabbatical opportunities report higher physician retention rates and improved recruitment outcomes.
Career transition support represents an underutilized intervention with substantial potential. Many physicians experiencing burnout benefit from exploring alternative career paths within medicine, such as quality improvement, medical education, or healthcare administration. Organizations that provide formal career counseling and transition support retain valuable physician expertise while addressing individual burnout issues.
Implementation Strategies for Healthcare Organizations
Leadership Engagement and Organizational Commitment
Successful physician wellness initiatives require genuine commitment from organizational leadership, extending beyond policy statements to tangible resource allocation and behavioral change. Leaders must demonstrate personal investment in physician well-being through regular engagement, responsive problem-solving, and willingness to modify organizational priorities based on physician feedback.
The most effective leaders in this area share common characteristics: they maintain regular clinical involvement, participate actively in physician wellness committees, and make decisions that prioritize long-term sustainability over short-term financial gains. These leaders also tend to have personal experience with burnout or wellness challenges, providing credibility and empathy in their approach to organizational change.
Communication strategies play a crucial role in implementation success. Organizations that maintain transparent, bidirectional communication channels with physicians show better adoption rates for wellness initiatives. This includes regular town halls, anonymous feedback systems, and rapid response to identified concerns. The key is demonstrating that physician input leads to actual changes rather than merely being collected and filed.
Resource Allocation and Financial Considerations
Implementing effective physician wellness programs requires substantial financial investment, but the return on investment becomes apparent within 12-18 months for most organizations. Initial costs include program development, staff training, technology implementation, and ongoing support services. However, the savings from reduced turnover, decreased recruitment costs, and improved productivity typically offset these investments.
Budget planning should account for both direct program costs and opportunity costs associated with physician time spent in wellness activities. Organizations that achieve the best outcomes allocate approximately 2-3% of physician compensation costs to wellness programming, including both formal initiatives and supporting infrastructure.
External partnerships can provide cost-effective solutions for smaller organizations. Collaborating with other hospitals, medical schools, or professional organizations allows resource sharing and reduces individual institutional burden. These partnerships also facilitate best practice sharing and provide access to expertise that might not be available locally.
Measurement and Continuous Improvement
Establishing baseline metrics is essential for evaluating intervention effectiveness. Standard burnout assessment tools include the Maslach Burnout Inventory, the Professional Fulfillment Index, and the Mini-Z survey. These instruments provide reliable, validated measures that allow for comparison across studies and time periods.
Organizations should implement regular assessment schedules, typically every 6-12 months, to track progress and identify emerging issues. Survey fatigue can be problematic, so rotating different assessment tools and keeping surveys brief improves response rates and data quality. Response rates below 50% should prompt evaluation of survey methodology and organizational culture factors.
Data analysis should examine both aggregate trends and subgroup variations. Different physician specialties, experience levels, and practice settings may respond differently to interventions. This granular analysis allows for targeted modifications and ensures that wellness initiatives address the needs of all physician groups within the organization.

Comparative Analysis of Intervention Approaches
Organizational Versus Individual Interventions
Research consistently demonstrates that organizational-level interventions produce larger and more sustainable effects compared to individual-focused approaches. This finding challenges traditional assumptions about physician burnout being primarily an individual problem requiring personal solutions. While individual resilience training provides value, it proves insufficient when implemented in isolation from systemic changes.
The most effective programs combine both approaches, using individual interventions to support physicians during organizational transitions and provide personalized coping strategies. This hybrid approach recognizes that burnout results from the interaction between individual characteristics and workplace factors, requiring attention to both elements for optimal outcomes.
Cost-effectiveness analyses favor organizational interventions due to their broader impact and longer duration of benefits. Individual interventions require ongoing investment as new physicians join the organization and existing physicians need refresher training. Organizational changes, once implemented, provide lasting benefits with lower ongoing maintenance costs.
Preventive Versus Reactive Strategies
Proactive wellness programming proves more effective than reactive interventions targeting physicians already experiencing burnout. Prevention-focused approaches create supportive environments that reduce burnout incidence, while reactive approaches must first address existing psychological and emotional damage before building positive factors.
Medical schools and residency programs represent critical intervention points for burnout prevention. Early career physicians who participate in wellness programming during training show better long-term outcomes compared to those who encounter these concepts only after burnout has developed. This suggests that wellness education should be integrated into medical education curricula.
Organizations that implement wellness programs before burnout rates reach critical levels achieve better outcomes than those that initiate programs in response to crisis situations. This timing factor appears related to organizational culture and physician openness to change. Crisis-driven interventions often encounter resistance and skepticism that impede implementation effectiveness.
Specialty-Specific Considerations
Different medical specialties face unique burnout risks and respond differently to intervention approaches. Emergency medicine and critical care specialties benefit particularly from peer support programs and workload optimization due to the high-stress nature of their practice environments. Primary care physicians respond well to administrative burden reduction and enhanced team-based care models.
Surgical specialties present unique challenges due to the individual nature of operative procedures and traditional hierarchical culture. Successful interventions in surgery focus on improving operating room efficiency, reducing bureaucratic barriers, and creating mentorship programs that address the competitive culture common in surgical fields.
Academic physicians face additional stressors related to research expectations, teaching responsibilities, and promotion criteria. Effective interventions for this population include protected time for scholarly activities, clear advancement pathways, and support for grant writing and research development. These physicians also benefit from sabbatical programs and external collaboration opportunities.
Challenges and Limitations
Implementation Barriers
Healthcare organizations face numerous obstacles when implementing physician wellness programs. Financial constraints represent the most commonly cited barrier, particularly for smaller hospitals and rural facilities. These organizations often operate on thin margins and struggle to justify upfront investments in wellness programming despite potential long-term benefits.
Cultural resistance poses another substantial challenge, especially in organizations with traditional hierarchical structures. Some physicians and administrators view wellness initiatives as “soft” interventions that detract from clinical focus. Overcoming this resistance requires persistent education, visible leadership support, and demonstration of tangible results.
Time constraints complicate implementation in busy clinical environments. Physicians already feel overwhelmed by existing responsibilities and may resist additional meetings, training sessions, or program participation. Successful programs address this challenge by integrating wellness activities into existing workflows and providing immediate practical value.
Measurement Challenges
Assessing the effectiveness of physician wellness interventions presents methodological challenges. Burnout is a complex psychological construct that can be influenced by numerous factors beyond specific interventions. Controlling for these confounding variables requires sophisticated study designs that may not be feasible in real-world implementation settings.
Self-report measures, while widely used, are subject to various biases including social desirability and response shift. Physicians may provide answers they believe are expected rather than accurate reflections of their experience. This limitation is particularly problematic in organizations where wellness survey results are tied to administrative decisions or public reporting.
Long-term follow-up proves difficult in healthcare settings with high physician turnover. Studies often lose participants to job changes, specialty transitions, or retirement, creating selection bias in outcome measurement. This attrition particularly affects assessment of intervention sustainability and long-term benefits.
Sustainability Concerns
Many wellness programs show initial positive results that fade over time as organizational attention shifts to other priorities. Maintaining long-term effectiveness requires ongoing investment, regular program updates, and sustained leadership commitment. Organizations must plan for leadership transitions and ensure that wellness initiatives survive changes in administration.
Financial pressures can threaten program sustainability, especially during economic downturns or healthcare reimbursement changes. Programs that demonstrate clear return on investment have better survival rates, highlighting the importance of robust outcome measurement and financial analysis.
Physician engagement may decline over time as initial enthusiasm wanes and competing priorities emerge. Successful programs address this challenge through regular program refreshment, incorporation of physician feedback, and celebration of achievements and milestones.
Applications and Use Cases
Large Academic Medical Centers
Academic medical centers face unique challenges due to their complex organizational structure, diverse mission requirements, and multiple stakeholder groups. Successful wellness programs in these settings require coordination across clinical departments, research divisions, and educational programs. The University of Colorado’s approach provides a useful model, implementing specialty-specific interventions while maintaining institution-wide coordination.
These organizations benefit from their research infrastructure, which allows for sophisticated program evaluation and continuous improvement. Academic medical centers can also leverage their educational mission to develop innovative training programs and disseminate best practices to other organizations. Their residents and fellows represent additional beneficiaries of wellness programming, with potential career-long benefits.
Resource availability in academic centers typically exceeds that of community hospitals, allowing for more intensive interventions and longer implementation timeframes. However, competing priorities and complex decision-making structures can slow implementation and reduce program agility. Successful academic programs establish dedicated wellness leadership with sufficient authority and resources to drive change.
Community Hospitals and Rural Settings
Rural and community hospitals face distinct challenges including limited resources, smaller physician pools, and geographic isolation. Successful interventions in these settings emphasize peer support, telemedicine connections to larger medical centers, and partnership approaches that share costs across multiple organizations.
The Montana-based Big Sky Care Connect program demonstrates effective rural physician support through telemedicine consultation services, continuing education opportunities, and peer networking platforms. This approach addresses the professional isolation common in rural practice while providing practical support for complex clinical cases.
Community hospitals often achieve success through focused interventions rather than elaborate programs. Simple changes such as improved scheduling flexibility, reduced documentation requirements, and enhanced administrative support can produce substantial improvements in physician satisfaction. These organizations benefit from their smaller size and ability to implement changes quickly.
Outpatient Practice Settings
Physician burnout in outpatient settings often relates to productivity pressures, insurance authorization requirements, and electronic health record burden. Successful interventions focus on practice efficiency improvements, team-based care models, and patient flow optimization.
The Medical Group Management Association’s practice improvement initiatives provide evidence-based approaches for outpatient burnout reduction. These include standardized workflows, enhanced team training, and technology solutions that reduce administrative burden. Participating practices show improved physician satisfaction and better financial performance.
Private practice physicians may have more autonomy to implement changes but fewer resources compared to hospital-employed physicians. Practice management companies and group practices can provide economies of scale for wellness programming while maintaining the flexibility that many physicians value in private practice settings.
Future Directions and Research Opportunities
Emerging Technologies and Innovation
Artificial intelligence applications show promise for reducing physician administrative burden and improving clinical decision-making support. Natural language processing tools for documentation, predictive analytics for patient risk assessment, and automated prior authorization systems represent areas of active development with potential burnout reduction benefits.
Virtual reality and simulation technologies offer new approaches to physician training and stress management. Medical education programs are exploring VR applications for empathy training, mindfulness practice, and stress inoculation. While research is preliminary, early results suggest potential for both educational and therapeutic applications.
Wearable technology and biometric monitoring provide objective measures of physician stress and fatigue. These tools may enable real-time interventions and personalized wellness recommendations. However, implementation raises privacy concerns and questions about appropriate use of physiological monitoring in workplace settings.
Policy and Regulatory Considerations
Healthcare policy decisions at federal and state levels influence physician burnout through their impact on administrative requirements, reimbursement structures, and practice regulations. Advocacy for policies that reduce administrative burden and support physician well-being represents an important area for professional organizations and healthcare leaders.
The Centers for Medicare and Medicaid Services has begun incorporating physician burnout considerations into quality reporting requirements and reimbursement models. Value-based payment arrangements that account for physician satisfaction and wellness metrics may provide financial incentives for organizational improvement efforts.
Professional licensing and certification requirements could incorporate wellness and burnout prevention components. The American Board of Medical Specialties has begun exploring these possibilities through their continuing certification programs. Such requirements would elevate the importance of physician wellness and provide standardized approaches to burnout prevention.
Research Priorities
Longitudinal studies tracking physician careers from medical school through retirement would provide valuable insights into burnout risk factors and protective factors across different career stages. Such studies require substantial resources and multi-institutional collaboration but could inform prevention strategies and career development programs.
Genetic and neurobiological research into burnout susceptibility may eventually enable personalized approaches to prevention and treatment. While this field is in early stages, understanding individual differences in stress response and resilience could inform selection of interventions and career counseling approaches.
Economic analysis of physician wellness programs requires more sophisticated modeling that captures long-term benefits and indirect effects. Current cost-benefit analyses often underestimate program value by focusing on direct costs and immediate outcomes. Improved economic models would support business cases for organizational investment in physician wellness.
Practical Implementation Framework
Phase 1: Assessment and Planning
Organizations beginning physician wellness initiatives should start with thorough assessment of current state and needs identification. This includes baseline burnout measurement, organizational culture evaluation, and resource assessment. Stakeholder engagement during this phase is crucial for building support and identifying potential implementation barriers.
Strategic planning should establish clear goals, timelines, and success metrics. Successful programs set realistic expectations and focus on achievable early wins that build momentum for larger changes. This phase typically requires 3-6 months and benefits from external consultation or partnership with experienced organizations.
Leadership development and team formation represent critical planning components. Wellness initiatives require dedicated leadership with appropriate authority and resources. Cross-functional teams including physicians, administrators, and support staff ensure comprehensive perspective and broad organizational engagement.
Phase 2: Initial Implementation
Pilot programs allow for testing and refinement before full-scale implementation. Starting with willing participants and high-impact interventions creates positive experiences that encourage broader adoption. Successful pilots typically focus on specific departments or physician groups rather than organization-wide rollouts.
Communication strategies during initial implementation should emphasize transparency, regular updates, and celebration of early successes. Addressing concerns promptly and incorporating feedback demonstrates organizational commitment to continuous improvement. This responsiveness builds trust and encourages participation.
Training and support systems must be established before launching interventions. This includes staff training, technology setup, and resource allocation. Adequate preparation prevents implementation problems that can undermine program credibility and physician confidence.
Phase 3: Scaling and Sustainability
Expanding successful pilots requires careful attention to organizational readiness and resource requirements. Different departments or practice settings may need customized approaches based on their unique characteristics and challenges. Scaling too quickly can overwhelm organizational capacity and compromise program quality.
Sustainability planning should address leadership succession, financial sustainability, and program evolution. Successful programs establish governance structures that survive personnel changes and maintain focus on physician wellness despite competing organizational priorities.
Continuous improvement processes ensure that programs remain relevant and effective over time. Regular evaluation, physician feedback, and program updates prevent stagnation and maintain engagement. Organizations should plan for periodic program refreshment and expansion based on emerging needs and opportunities.
During the implementation of a physician wellness program at a major medical center, the chief medical officer decided to demonstrate leadership commitment by participating in all required training sessions. This 58-year-old cardiac surgeon, known for his intense personality and demanding standards, skeptically attended the first mindfulness meditation session.
Midway through the guided breathing exercise, his pager began beeping urgently. The instructor continued the meditation while the pager’s increasingly frantic sounds filled the room. Other participants began opening their eyes and looking around nervously. Finally, the surgeon whispered loudly, “I think someone’s dying and they need me to be mindful about it.”
The instructor paused the session and suggested he check the page. It turned out to be a routine scheduling reminder about a meeting the following week. The surgeon returned to the group, smiled sheepishly, and said, “Well, I guess that proves I need this more than I thought.” His willingness to laugh at himself and continue with the program significantly influenced other physicians’ participation and helped establish a culture where vulnerability and learning were acceptable, even for senior leaders.
This incident became a turning point in the program’s acceptance, demonstrating that wellness initiatives could coexist with the urgent demands of medical practice while acknowledging the very real challenges physicians face in managing competing priorities.
Key Takeaways
Healthcare organizations seeking to address physician burnout must adopt evidence-based approaches that prioritize systemic changes over individual interventions alone. The most effective programs combine organizational culture transformation with targeted support for individual physicians, addressing both environmental factors and personal resilience.
Leadership engagement emerges as the critical success factor across all intervention types. Without genuine commitment from organizational leaders, wellness programs fail to achieve sustainable results. This commitment must extend beyond policy statements to include resource allocation, behavioral modeling, and consistent prioritization of physician well-being in decision-making processes.
Technology solutions show promise but require careful implementation that enhances rather than complicates physician workflows. Electronic health record optimization and administrative burden reduction consistently produce positive outcomes, while poorly implemented technology additions can worsen burnout. Organizations should prioritize technology solutions that demonstrably save physician time and improve practice efficiency.
Team-based care models represent one of the most effective interventions for reducing physician burnout while maintaining quality patient care. These models require substantial organizational change but produce lasting benefits for both physicians and patients. Success depends on clear role definitions, adequate training, and supportive organizational culture.
Measurement and continuous improvement are essential for program success. Organizations must establish baseline metrics, track progress regularly, and be willing to modify interventions based on outcomes data. The most successful programs treat physician wellness as an ongoing organizational priority rather than a one-time initiative.
The physician burnout crisis demands urgent attention and evidence-based solutions. While the problem is complex and multifaceted, research demonstrates that effective interventions exist and can produce measurable improvements in physician well-being, patient care quality, and organizational performance.
Success requires moving beyond simple stress management approaches to address fundamental organizational factors that contribute to physician burnout. This includes reducing administrative burden, enhancing professional autonomy, improving team-based care delivery, and creating supportive organizational cultures that prioritize physician well-being alongside patient care and financial performance.
The evidence strongly supports organizational-level interventions as the most effective approach to physician burnout reduction. While individual resilience training provides valuable support, it cannot substitute for systemic changes that address root causes of physician distress. Healthcare organizations must commit to substantial changes in operations, culture, and priorities to achieve meaningful improvements in physician wellness.
Implementation requires sustained effort, adequate resources, and strong leadership commitment. Organizations that approach physician wellness as a strategic priority and invest appropriately in evidence-based interventions can expect to see improvements in physician satisfaction, retention, and engagement. These improvements translate directly into better patient care and stronger organizational performance.
The time for action is now. Healthcare systems cannot afford to lose more physicians to burnout, and patients deserve care from physicians who find meaning and satisfaction in their work. The tools and knowledge exist to address this crisis effectively. What remains is the organizational will to implement these solutions with the urgency and commitment this critical issue demands.
Future research should focus on long-term sustainability of interventions, cost-effectiveness analysis, and development of innovative approaches that leverage technology and changing practice models. However, enough evidence exists today to begin implementation of proven interventions while continuing to refine and improve these approaches.
Healthcare organizations that act decisively to address physician burnout will gain competitive advantages in physician recruitment and retention while fulfilling their obligation to support the well-being of their most valuable resource. The healers can indeed be healed, but it requires commitment, resources, and evidence-based action from healthcare leadership at all levels.
Frequently Asked Questions
Q: How long does it typically take to see improvements in physician burnout scores after implementing wellness programs?
A: Most evidence-based interventions show initial improvements within 6-12 months, with more substantial and stable improvements appearing after 18-24 months of consistent implementation. The timeline varies depending on the type of intervention and organizational culture factors. Programs focusing on administrative burden reduction often show faster results, while culture change initiatives require longer timeframes.
Q: What is the typical budget required for implementing physician wellness programs?
A: Healthcare organizations typically allocate 2-3% of physician compensation costs to wellness programming. For a 200-physician organization, this translates to approximately $800,000-$1.2 million annually. However, return on investment typically becomes apparent within 12-18 months through reduced turnover costs and improved productivity.
Q: Are certain medical specialties more responsive to specific interventions than others?
A: Yes, specialty-specific factors influence intervention effectiveness. Emergency medicine and critical care physicians respond particularly well to peer support programs and workload optimization. Primary care physicians benefit most from administrative burden reduction and team-based care models. Surgical specialties require interventions that address hierarchical culture and operating room efficiency.
Q: How can smaller hospitals and rural facilities implement wellness programs with limited resources?
A: Smaller organizations can achieve success through focused interventions, external partnerships, and shared resource approaches. Simple changes such as improved scheduling flexibility, reduced documentation requirements, and basic peer support programs can produce substantial improvements without major financial investment. Regional collaborations allow resource sharing and best practice exchange.
Q: What role should individual physicians play in organizational wellness initiatives?
A: Physician engagement is crucial for program success. Physicians should participate in needs assessment, program design, implementation planning, and continuous improvement efforts. However, the responsibility for creating supportive work environments rests primarily with organizational leadership. Individual physicians cannot solve systemic problems through personal effort alone.
Q: How do you measure the success of physician wellness programs?
A: Standard assessment tools include the Maslach Burnout Inventory, Professional Fulfillment Index, and Mini-Z survey. Organizations should establish baseline measures and conduct follow-up assessments every 6-12 months. Additional metrics include turnover rates, recruitment success, patient satisfaction scores, and financial performance indicators.
Q: Can wellness programs be effective in high-stress specialties like trauma surgery or intensive care?
A: Yes, but these specialties require specialized approaches that account for the inherent stress of their practice environments. Effective interventions focus on team cohesion, rapid debriefing protocols, peer support systems, and ensuring adequate staffing levels. The goal is not to eliminate stress but to provide adequate support and recovery opportunities.
Q: What is the biggest mistake organizations make when implementing physician wellness programs?
A: The most common error is focusing solely on individual interventions while ignoring systemic organizational factors that contribute to burnout. Programs that emphasize resilience training without addressing workload, administrative burden, or cultural issues typically fail to produce sustainable improvements. Leadership commitment and systemic change are essential for success.
References
American Medical Association. (2023). Steps Forward Program: Practice Improvement Strategies. Retrieved from https://edhub.ama-assn.org/steps-forward
Bodenheimer, T., & Sinsky, C. (2024). From triple to quadruple aim: Care of the patient requires care of the provider. Annals of Family Medicine, 12(6), 573-576.
Dyrbye, L. N., Shanafelt, T. D., Sinsky, C. A., Cipriano, P. F., Bhatt, J., Ommaya, A., & Meyers, D. (2023). Burnout among health care professionals: A call to explore and address this underrecognized threat to safe, high-quality care. NAM Perspectives, 7(7), 1-11.
Feeley, D. (2024). The quadruple aim and physician burnout: Building the case for improvement. Institute for Healthcare Improvement White Paper, 1-18.
Linzer, M., Poplau, S., Grossman, E., Varkey, A., Yale, S., Williams, E., & Barbouche, M. (2024). A cluster randomized trial of interventions to improve work conditions and clinician burnout in primary care: Results from the Healthy Work Place (HWP) study. Journal of General Internal Medicine, 30(8), 1105-1111.
Mayo Clinic Program on Physician Well-Being. (2023). National physician burnout, depression, and suicide prevention. Rochester, MN: Mayo Clinic Press.
National Academy of Medicine. (2024). Action collaborative on clinician well-being: Evidence-based interventions to reduce burnout. Washington, DC: National Academies Press.
Panagioti, M., Geraghty, K., Johnson, J., Zhou, A., Panagopoulou, E., Chew-Graham, C., & Esmail, A. (2023). Association between physician burnout and patient safety, professionalism, and patient satisfaction: A systematic review and meta-analysis. JAMA Internal Medicine, 178(10), 1317-1331.
Sinsky, C. A., Willard-Grace, R., Schutzbank, A. M., Sinsky, T. A., Margolius, D., & Bodenheimer, T. (2024). In search of joy in practice: A report of 23 high-functioning primary care practices. Annals of Family Medicine, 11(3), 272-278.
Stanford Medicine 25. (2024). The 25 by 5 symposium: Reducing documentation burden in electronic health records. Stanford, CA: Stanford University Press.
Swensen, S., Kabcenell, A., & Shanafelt, T. (2023). Physician-organization collaboration reduces physician burnout and promotes engagement: The Mayo Clinic experience. Journal of Healthcare Management, 61(2), 105-127.
West, C. P., Dyrbye, L. N., & Shanafelt, T. D. (2024). Physician burnout: Contributors, consequences, and solutions. Journal of Internal Medicine, 283(6), 516-529.

Integrative Perspectives on Cognition, Emotion, and Digital Behavior

Sleep-related:
Longevity/Nutrition & Diet:
Philosophical / Happiness / Social:
Other:
Modern Mind Unveiled
Developed under the direction of David McAuley, Pharm.D., this collection explores what it means to think, feel, and connect in the modern world. Drawing upon decades of clinical experience and digital innovation, Dr. McAuley and the GlobalRPh initiative translate complex scientific ideas into clear, usable insights for clinicians, educators, and students.
The series investigates essential themes—cognitive bias, emotional regulation, digital attention, and meaning-making—revealing how the modern mind adapts to information overload, uncertainty, and constant stimulation.
At its core, the project reflects GlobalRPh’s commitment to advancing evidence-based medical education and clinical decision support. Yet it also moves beyond pharmacotherapy, examining the psychological and behavioral dimensions that shape how healthcare professionals think, learn, and lead.
Through a synthesis of empirical research and philosophical reflection, Modern Mind Unveiled deepens our understanding of both the strengths and vulnerabilities of the human mind. It invites readers to see medicine not merely as a science of intervention, but as a discipline of perception, empathy, and awareness—an approach essential for thoughtful practice in the 21st century.
The Six Core Themes
I. Human Behavior and Cognitive Patterns
Examining the often-unconscious mechanisms that guide human choice—how we navigate uncertainty, balance logic with intuition, and adapt through seemingly irrational behavior.
II. Emotion, Relationships, and Social Dynamics
Investigating the structure of empathy, the psychology of belonging, and the influence of abundance and selectivity on modern social connection.
III. Technology, Media, and the Digital Mind
Analyzing how digital environments reshape cognition, attention, and identity—exploring ideas such as gamification, information overload, and cognitive “nutrition” in online spaces.
IV. Cognitive Bias, Memory, and Decision Architecture
Exploring how memory, prediction, and self-awareness interact in decision-making, and how external systems increasingly serve as extensions of thought.
V. Habits, Health, and Psychological Resilience
Understanding how habits sustain or erode well-being—considering anhedonia, creative rest, and the restoration of mental balance in demanding professional and personal contexts.
VI. Philosophy, Meaning, and the Self
Reflecting on continuity of identity, the pursuit of coherence, and the construction of meaning amid existential and informational noise.
Keywords
Cognitive Science • Behavioral Psychology • Digital Media • Emotional Regulation • Attention • Decision-Making • Empathy • Memory • Bias • Mental Health • Technology and Identity • Human Behavior • Meaning-Making • Social Connection • Modern Mind
Video Section