Anesthesia for Non-Operating Room Procedures (NORA) The New Frontier in Risk

Abstract
Non operating room anesthesia has become one of the most rapidly expanding domains within anesthesiology, with procedural volumes increasing by more than 15 percent annually. This growth reflects broader trends in healthcare delivery, including the shift toward minimally invasive procedures, the expansion of interventional radiology, endoscopy, cardiology, and ambulatory care services, and increasing demand for procedural sedation outside the traditional operating room. While this evolution has improved access to diagnostic and therapeutic interventions, it has also introduced a distinct set of clinical, logistical, and safety challenges that require careful consideration.
Unlike the controlled environment of the operating room, non operating room anesthesia settings are often characterized by variability in infrastructure, limited space, and reduced availability of specialized equipment. These environments may include radiology suites, endoscopy units, cardiac catheterization laboratories, and outpatient procedure centers, each with unique constraints that can impact anesthetic management. In many cases, these locations were not originally designed to accommodate the full spectrum of anesthesia care, leading to potential gaps in monitoring capabilities, airway management resources, and emergency preparedness.
This analysis aims to evaluate the current state of non operating room anesthesia practice by examining key risk factors, reviewing adverse event data, and identifying strategies to enhance patient safety. Evidence from recent literature indicates that mortality rates in non operating room settings may be up to 2.4 times higher than those observed in traditional operating rooms. This increased risk is multifactorial and often related to environmental limitations, suboptimal equipment availability, delayed recognition of clinical deterioration, and communication challenges among multidisciplinary teams.
Patient related factors also play a critical role in determining outcomes in non operating room anesthesia. Many patients undergoing procedures in these settings are older, have significant comorbidities, or are classified as higher risk according to standard anesthetic assessment scales. Inadequate pre procedural evaluation or inappropriate patient selection can further increase the likelihood of complications. As a result, careful risk stratification and adherence to established selection criteria are essential to ensure that only suitable patients undergo procedures in remote environments.
Environmental preparation represents another key determinant of safety. Ensuring the availability of essential monitoring equipment, including continuous pulse oximetry, capnography, noninvasive blood pressure monitoring, and electrocardiography, is fundamental. In addition, access to airway management tools, resuscitation medications, and defibrillation equipment must be guaranteed before initiating any procedure. Standardization of equipment layout and emergency protocols across different locations can help reduce variability and improve response times during critical events.
Staffing and team communication are equally important components of safe non operating room anesthesia practice. Personnel working in these settings may have varying levels of familiarity with anesthesia related emergencies, making targeted training and simulation exercises essential. Clear delineation of roles, effective communication strategies, and the presence of trained anesthesia providers are critical to managing complications promptly and effectively. Interdisciplinary collaboration between anesthesiologists, proceduralists, nurses, and technicians is necessary to ensure coordinated and efficient care delivery.
The implementation of standardized protocols has been shown to significantly reduce adverse events in non operating room settings, with some studies suggesting reductions of up to 40 percent. These protocols typically include structured pre procedure checklists, intra procedural monitoring standards, and post procedure recovery guidelines. Incorporating safety frameworks such as time out procedures, sedation scoring systems, and early warning tools can further enhance patient outcomes.
Looking ahead, advancements in monitoring technology and digital health integration offer opportunities to improve safety in non operating room anesthesia. Portable monitoring systems, wireless data transmission, and real time alert systems may help bridge the gap between remote environments and traditional operating rooms. Future research should focus on developing location specific safety guidelines, optimizing workflow design, and evaluating the impact of emerging technologies on clinical outcomes.
In summary, non operating room anesthesia represents a dynamic and expanding field that demands a proactive approach to risk management. While these settings introduce unique vulnerabilities, adherence to evidence based practices, appropriate patient selection, adequate resource allocation, and strong team coordination can substantially mitigate risk. As the demand for procedures outside the operating room continues to grow, ensuring the safety and quality of anesthesia care in these environments will remain a critical priority for healthcare systems worldwide.
Introduction
The practice of anesthesia has undergone substantial transformation over the past two decades, driven by advances in medical technology, minimally invasive procedures, and shifting healthcare delivery models. A growing proportion of diagnostic and therapeutic interventions that historically required general anesthesia in fully equipped operating rooms are now performed in remote clinical settings across healthcare facilities. These environments, collectively referred to as non operating room anesthesia settings, include radiology suites, cardiac catheterization laboratories, endoscopy units, interventional radiology suites, emergency departments, and, in some cases, inpatient wards and intensive care units.
This transition reflects the increasing complexity and breadth of procedures performed outside the traditional operating room, including image guided interventions, electrophysiological studies, and advanced endoscopic therapies. While these developments have expanded access to care and improved procedural efficiency, they have also introduced new and often underappreciated challenges for anesthesia providers. Unlike operating rooms, which are specifically designed to support anesthesia delivery with standardized equipment, personnel, and safety protocols, non operating room environments frequently lack consistent infrastructure and may not be optimized for airway management, patient monitoring, or rapid emergency response.
Anesthesia providers working in these settings must therefore adapt to environments that are inherently variable and sometimes constrained. Limitations may include restricted physical space, suboptimal patient positioning, limited access to the patient during procedures, inadequate lighting, and variability in the availability of essential equipment such as suction devices, oxygen delivery systems, and advanced airway tools. In addition, the presence of radiation, magnetic fields, or other environmental hazards may further complicate anesthetic management and require specialized precautions. These factors necessitate careful pre procedure planning, thorough equipment checks, and heightened situational awareness.
The increasing prevalence of non operating room anesthesia has made familiarity with its associated risks a critical competency for modern anesthesia practice. Data from the American Society of Anesthesiologists indicate that non operating room cases now account for approximately 40 percent of all anesthetics delivered in many healthcare systems. This proportion is expected to continue rising as procedural medicine expands and patient demand for less invasive interventions grows. As a result, anesthesia providers must be equipped not only with technical expertise but also with the ability to anticipate and mitigate risks unique to these environments.
Patient safety considerations in non operating room anesthesia settings are particularly important. Multiple studies have demonstrated higher rates of adverse events, including respiratory complications, hemodynamic instability, and delayed recognition of clinical deterioration, when compared with procedures performed in traditional operating rooms. Notably, these increased risks cannot be fully explained by differences in patient acuity or procedural complexity alone. Environmental constraints, limited staffing support, communication challenges, and workflow inefficiencies all contribute to the elevated risk profile observed in these settings.
Furthermore, emergency preparedness in non operating room environments often differs significantly from that of the operating room. Immediate access to additional anesthesia personnel, surgical backup, or resuscitation teams may be limited, and protocols for crisis management may not be as well established or rehearsed. This underscores the importance of standardized guidelines, simulation based training, and interdisciplinary collaboration to ensure that all team members are prepared to respond effectively to critical events.
In response to these challenges, professional societies have developed recommendations to improve safety in non operating room anesthesia practice. These include establishing minimum monitoring standards equivalent to those in the operating room, ensuring the availability of essential resuscitation equipment, conducting pre procedure risk assessments, and implementing structured communication protocols among multidisciplinary teams. Adherence to these principles is essential to reduce variability in care and enhance patient outcomes.
In summary, the expansion of non operating room anesthesia represents a fundamental shift in the delivery of anesthetic care. While it offers significant benefits in terms of accessibility and procedural innovation, it also introduces complex risks that require careful management. A comprehensive understanding of the unique challenges associated with these environments, combined with adherence to standardized safety practices, is essential for optimizing patient outcomes and ensuring the continued evolution of safe anesthesia care.

The Evolution of NORA Practice
Historical Context
Twenty years ago, anesthesia outside the operating room was relatively uncommon. Most procedures requiring sedation or anesthesia took place in controlled surgical environments with dedicated support staff and standardized equipment. The growth of minimally invasive procedures and advanced imaging techniques changed this paradigm rapidly.
Cardiac catheterization procedures were among the first to establish dedicated anesthesia services outside traditional operating rooms. These procedures required precise patient positioning and specialized equipment that made operating room use inefficient. Radiology departments followed suit as complex interventional procedures became more common.
The COVID-19 pandemic accelerated NORA adoption as healthcare systems sought to preserve operating room capacity for essential surgeries. Many procedures that traditionally required operating rooms were relocated to alternative sites. This rapid expansion highlighted both the potential benefits and risks of NORA practice.
Current Scope and Volume
Data from the National Anesthesia Clinical Outcomes Registry shows that NORA cases increased from 28% of all anesthetics in 2010 to 43% in 2023. This growth pattern appears consistent across different healthcare settings and geographic regions. Academic medical centers report even higher percentages, with some institutions performing over 60% of anesthetics in non-operating room locations.
The types of procedures performed in NORA settings continue to expand. Common categories include:
Interventional cardiology procedures account for approximately 35% of NORA cases. These include cardiac catheterizations, electrophysiology studies, and transcatheter valve procedures. Patient acuity in these cases is often high, with multiple comorbidities and unstable cardiac conditions.
Radiology procedures represent another 30% of NORA volume. Magnetic resonance imaging studies in pediatric patients or adults with claustrophobia require sedation or general anesthesia. Interventional radiology procedures have become increasingly complex, often lasting several hours and requiring multiple anesthetic techniques.
Gastroenterology procedures comprise 20% of NORA cases. Endoscopic retrograde cholangiopancreatography and endoscopic ultrasound procedures often require deep sedation or general anesthesia. These procedures can be technically challenging with limited patient access for the anesthesia provider.
Emergency department procedures account for 10% of NORA volume. These cases often involve unstable patients requiring urgent intervention. The emergency setting adds time pressure and limited preparation time to the inherent challenges of NORA practice.
The remaining 5% includes procedures in various other locations such as labor and delivery units, intensive care units, and specialized procedure rooms. Each environment presents unique challenges and risk factors.
Risk Factors in NORA Environments
Environmental Challenges
The physical environment in NORA locations creates unique safety challenges. Unlike operating rooms designed specifically for anesthetic care, remote locations often have competing priorities that can compromise patient safety.
Space constraints represent a primary environmental challenge. Many NORA locations have limited room for anesthesia equipment and personnel movement. Radiology suites, in particular, are designed around imaging equipment with minimal space for additional medical devices. This spatial limitation can delay response to emergencies and limit access to backup equipment.
Lighting conditions in NORA environments often differ from operating room standards. Interventional procedures may require dimmed lighting for optimal visualization of monitors and imaging equipment. These conditions can make patient assessment more difficult and increase the risk of medication errors.
Temperature control presents ongoing challenges in many NORA locations. Cardiac catheterization laboratories are often kept cooler to protect sensitive electronic equipment, which can increase patient heat loss and complicate temperature management. Radiology suites may have temperature fluctuations related to imaging equipment operation.
Noise levels in NORA environments frequently exceed operating room standards. Magnetic resonance imaging equipment produces intense noise that can interfere with patient monitoring and communication. Cardiac catheterization laboratories have multiple electronic devices that create ambient noise and potential alarm fatigue.
Equipment and Resource Limitations
NORA locations often have equipment limitations that can compromise patient care. Unlike operating rooms with standardized anesthesia machines and monitoring equipment, remote locations may have older or less sophisticated devices. Some facilities use portable anesthesia machines that lack the safety features and backup systems found in modern operating room equipment.
Medication availability can be limited in NORA settings. Remote locations may not have immediate access to the full range of anesthetic drugs and emergency medications available in operating rooms. This limitation requires careful planning and may delay treatment of complications.
Airway management equipment in NORA locations may be limited compared to operating room standards. Some remote sites lack difficult airway carts or have limited backup equipment available. Video laryngoscopes and other advanced airway devices may not be readily accessible.
Blood product availability represents another resource limitation. NORA locations typically do not have blood products immediately available, which can delay treatment of hemorrhagic complications. The time required to obtain blood products from the blood bank can be critical in emergency situations.
Staffing and Communication Challenges
Staffing patterns in NORA environments often differ from operating room standards. Many remote locations operate with minimal support staff, leaving anesthesia providers to perform tasks typically handled by technicians or nurses. This increased workload can distract from patient monitoring and care.
Communication systems in NORA locations may be less developed than operating room standards. Some remote sites lack reliable communication with central monitoring stations or other clinical areas. This isolation can delay response to emergencies and limit access to consultation services.
Familiarity with local procedures and equipment varies among anesthesia staff. Unlike operating rooms where staff work regularly, NORA locations may have rotating coverage with less consistent team members. This unfamiliarity can lead to delays and errors during routine and emergency situations.
Table 1: Comparison of Operating Room vs. NORA Environment Characteristics
| Factor | Operating Room | NORA Environment | Risk Impact |
| Space availability | Designed for anesthesia care | Limited, competing uses | Moderate |
| Equipment standardization | High standardization | Variable equipment | High |
| Staff familiarity | Regular team members | Rotating coverage | Moderate |
| Emergency backup | Immediate availability | May be delayed | High |
| Communication systems | Established protocols | Variable systems | Moderate |
| Environmental controls | Optimized for surgery | Competing priorities | Low |
| Medication access | Full formulary | Limited selection | High |
Patient Selection and Risk Assessment
Preoperative Evaluation Considerations
Patient selection for NORA procedures requires careful consideration of factors beyond those typically evaluated for operating room procedures. The limited resources and environmental constraints in remote locations make some patients inappropriate candidates for NORA procedures.
Airway assessment takes on increased importance in NORA settings. Patients with known or suspected difficult airways may be better served in operating room environments where advanced equipment and immediate backup are available. The American Society of Anesthesiologists difficult airway guidelines recommend careful consideration of location when difficult airway management is anticipated.
Cardiac risk assessment must account for the limited cardiac support available in most NORA locations. Patients with unstable cardiac conditions may require the immediate availability of cardiac surgery or advanced cardiac life support capabilities found in operating rooms. Some institutions have developed specific cardiac risk criteria for NORA procedures.
Respiratory assessment should consider the patient’s ability to tolerate positioning required for specific procedures. Many NORA procedures require unusual positions that can compromise respiratory function. Patients with limited respiratory reserve may not tolerate these positions safely in environments with limited respiratory support.
Age-Related Considerations
Pediatric patients in NORA settings present unique challenges that require specialized preparation and expertise. Children may not cooperate with procedures in unfamiliar environments, increasing the need for deep sedation or general anesthesia. The smaller margin for error in pediatric patients makes environmental limitations more critical.
Elderly patients represent another high-risk population in NORA settings. Age-related changes in drug metabolism and cardiovascular function can make these patients more susceptible to complications. The extended procedure times common in some NORA procedures can be particularly challenging for elderly patients.
Comorbidity Assessment
Patients with multiple comorbidities require careful evaluation for NORA procedures. The limited ability to manage complications in remote locations makes patient selection critical. Some institutions have developed scoring systems to identify patients who may be inappropriate for NORA procedures.
Obesity presents particular challenges in NORA environments where space and equipment may be limited. Positioning obese patients for procedures can be difficult in constrained spaces. Additionally, the increased risk of airway complications in obese patients may make operating room locations more appropriate.
Safety Protocols and Standards
Institutional Policy Development
Healthcare institutions must develop specific policies and procedures for NORA practice that address the unique challenges of remote locations. These policies should cover equipment requirements, staffing standards, emergency protocols, and quality assurance measures.
Equipment standardization across NORA locations can reduce variability and improve safety. Some institutions have implemented standardized equipment packages that ensure consistent capabilities across different remote locations. This approach reduces the learning curve for providers and ensures reliable access to essential equipment.
Staffing standards for NORA locations should reflect the increased challenges and limited support available in remote environments. Some institutions require additional training or certification for providers working in NORA locations. Minimum staffing levels may need to be higher than traditional operating room standards.
Emergency Preparedness
Emergency protocols in NORA locations must account for the limited resources and potential delays in obtaining help. These protocols should address common emergencies such as airway complications, cardiovascular events, and allergic reactions. Regular training and simulation exercises can help maintain readiness for emergency situations.
Communication protocols during emergencies are particularly important in NORA locations. Clear procedures for calling for help and obtaining additional resources can reduce response times and improve outcomes. Some institutions have implemented emergency communication systems specifically for remote locations.
Quality Assurance and Monitoring
Quality assurance programs for NORA practice should track outcomes and identify opportunities for improvement. Monitoring systems should capture complications, delays, and other adverse events that may be related to environmental factors. Regular review of these data can guide policy improvements and training needs.
Peer review processes for NORA cases may need modification to account for environmental constraints. Reviews should consider whether complications were related to patient factors, provider decisions, or environmental limitations. This analysis can guide future policy and resource allocation decisions.
Anesthetic Techniques and Considerations
Sedation vs. General Anesthesia
The choice between sedation and general anesthesia in NORA settings requires careful consideration of patient, procedure, and environmental factors. Deep sedation can provide adequate conditions for many procedures while maintaining spontaneous ventilation and reducing airway intervention requirements.
Monitored anesthesia care with conscious sedation may be appropriate for shorter procedures in lower-risk patients. This technique reduces the complexity of anesthetic management while providing patient comfort. However, the potential for deeper levels of sedation must be anticipated and prepared for.
General anesthesia may be necessary for longer procedures, patient comfort, or airway protection. The decision to use general anesthesia in NORA settings should consider the availability of appropriate equipment and the ability to manage potential complications.
Drug Selection and Administration
Drug selection for NORA procedures should favor agents with predictable onset and recovery characteristics. Shorter-acting medications allow for more precise control and faster recovery, which can be particularly important in environments with limited recovery resources.
Propofol infusions have become popular for NORA procedures due to their controllability and rapid recovery characteristics. However, the potential for deeper levels of sedation and cardiovascular depression requires careful monitoring and titration.
Dexmedetomidine offers advantages in NORA settings due to its minimal respiratory depression and cooperative sedation characteristics. The longer onset and offset times require planning but can provide stable conditions for longer procedures.
Monitoring Requirements
Monitoring in NORA environments should meet or exceed operating room standards despite environmental challenges. Standard monitors including electrocardiography, blood pressure measurement, pulse oximetry, and capnography should be available and functional.
Capnography monitoring has particular importance in NORA settings where airway complications may be more difficult to manage. Early detection of respiratory depression or airway obstruction can prevent more serious complications.
Additional monitoring may be required for specific procedures or patient populations. Arterial pressure monitoring, central venous pressure measurement, or cardiac output monitoring may be necessary for high-risk procedures or patients.
Managing Complications in Remote Locations
Airway Emergencies
Airway complications in NORA settings require immediate recognition and intervention. The limited backup equipment and support staff in remote locations make prevention and early intervention critical. Providers must be prepared to manage difficult airways with potentially limited resources.
“Cannot intubate, cannot ventilate” situations in NORA locations present particular challenges. The equipment and personnel required for emergency surgical airway procedures may not be immediately available. Some institutions have developed rapid response protocols specifically for NORA airway emergencies.
I recall a particularly memorable incident early in my NORA career when a patient scheduled for a routine MRI developed laryngospasm just as the imaging sequence began. The combination of the magnetic field preventing immediate access and the overwhelming noise of the scanner created what can only be described as a perfect storm of Murphy’s Law. After what felt like an eternity but was probably only ninety seconds, we managed to abort the scan and provide appropriate treatment. The patient recovered completely, but the experience taught me never to underestimate the unique challenges that NORA environments can present.
Cardiovascular Complications
Cardiovascular emergencies in NORA locations require rapid assessment and treatment capabilities. The limited space and equipment in some remote locations can complicate resuscitation efforts. Emergency medications and defibrillation capabilities should be immediately available.
Hypotension during NORA procedures may be related to sedative medications, patient positioning, or underlying cardiac conditions. Treatment options may be limited by intravenous access and medication availability. Prevention through careful drug titration and patient positioning is preferable to treatment of established hypotension.
Allergic Reactions
Anaphylactic reactions in NORA settings require immediate recognition and treatment. The medications and equipment necessary for treating severe allergic reactions should be available in all NORA locations. Staff should be trained in recognition and management of allergic reactions.
Equipment Failures
Equipment failures in NORA locations can be particularly problematic due to limited backup equipment and support staff. Providers should be familiar with backup systems and alternative equipment options. Regular equipment checks and maintenance can prevent many failures.
Location-Specific Considerations
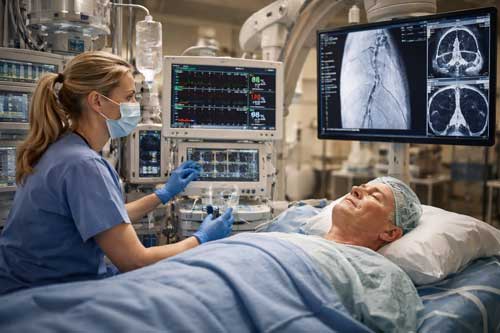
Radiology Suites
Radiology environments present unique challenges related to imaging equipment and radiation safety. Magnetic resonance imaging suites require special consideration due to the powerful magnetic fields that can affect monitoring equipment and limit access during emergencies.
Computed tomography suites involve radiation exposure that requires appropriate protection for anesthesia providers. Lead aprons and distance from radiation sources are essential safety measures. Some procedures may require providers to leave the room during imaging, creating monitoring challenges.
Cardiac Catheterization Laboratories
Cardiac catheterization laboratories typically have good equipment and staffing resources but present challenges related to patient positioning and procedure duration. The need for fluoroscopy creates radiation exposure concerns similar to radiology environments.
Emergency procedures in cardiac catheterization laboratories may involve unstable patients with acute cardiac conditions. The availability of cardiac surgery backup varies among institutions and should be considered in patient selection and risk assessment.
Endoscopy Suites
Endoscopy procedures often require shared airway management between anesthesia and procedure providers. Communication and coordination are essential to prevent airway complications. The prone or lateral positioning required for some procedures can complicate airway management.
Recovery from endoscopy procedures may be complicated by residual sedation and positioning changes. Adequate recovery facilities and staffing are essential for safe care.
Emergency Departments
Emergency department NORA procedures often involve unstable patients requiring urgent intervention. The time pressure and limited preparation time create additional challenges beyond those typical of NORA practice.
The busy emergency department environment can create distractions and communication challenges. Clear protocols and dedicated space for anesthetic care can improve safety and efficiency.
Training and Competency Requirements
Provider Education
Anesthesia providers working in NORA environments require specialized training beyond traditional operating room experience. This training should address environmental challenges, equipment limitations, and emergency protocols specific to remote locations.
Simulation training can provide valuable experience managing emergencies in NORA settings. Scenarios should include equipment failures, airway complications, and cardiovascular emergencies in realistic NORA environments. Regular simulation training can maintain competency and identify areas for improvement.
Continuing Education
The rapidly evolving nature of NORA practice requires ongoing education and training. New procedures, equipment, and safety protocols require regular updates to provider knowledge and skills. Professional organizations have developed NORA-specific continuing education programs.
Competency Assessment
Healthcare institutions should establish competency requirements for providers working in NORA environments. These requirements may include demonstration of specific skills, completion of training programs, or minimum experience levels.
Regular competency assessment can identify providers who may benefit from additional training or support. This process should be constructive and focused on improving patient safety rather than punitive measures.
Regulatory and Accreditation Considerations
Accreditation Standards
Healthcare accreditation organizations have developed specific standards for NORA practice. These standards address equipment requirements, staffing levels, and quality assurance measures. Compliance with these standards is essential for institutional accreditation.
The Joint Commission has established specific requirements for anesthesia services in non-operating room locations. These requirements address many of the safety concerns identified in NORA practice. Regular surveys assess compliance with these standards.
State and Federal Regulations
State medical boards and federal agencies have regulatory authority over anesthesia practice in all locations. Some states have developed specific regulations for NORA practice that address training requirements and practice standards.
Centers for Medicare and Medicaid Services payment policies can influence NORA practice patterns. Understanding these policies is important for institutional planning and resource allocation.
Economic Considerations
Cost-Benefit Analysis
The economic impact of NORA practice includes both potential benefits and additional costs. Benefits may include improved efficiency and patient satisfaction. Costs include additional equipment, training, and potential complications.
Efficiency gains from avoiding operating room use can be substantial but must be balanced against potential safety costs. Some studies suggest that NORA complications can result in higher overall costs despite initial savings.
Resource Allocation
Healthcare institutions must balance resource allocation between operating rooms and NORA locations. Adequate resources for safe NORA practice may require investment in equipment, staffing, and training.
Insurance and Liability Considerations
Professional liability insurance for NORA practice may have different requirements or costs compared to operating room practice. Understanding these differences is important for individual providers and healthcare institutions.
Future Directions and Research Needs
Technology Developments
Advances in monitoring technology may address some current limitations of NORA practice. Wireless monitoring systems and improved portable equipment could enhance safety in remote locations. Telemedicine applications may provide remote consultation capabilities for NORA procedures.
Artificial intelligence applications in patient monitoring and risk assessment could improve safety in NORA environments. These systems might provide early warning of developing complications or assist with drug dosing decisions.
Research Priorities
Current research in NORA practice focuses on identifying risk factors and developing prevention strategies. Large databases of NORA outcomes are providing insights into patterns of complications and effective prevention measures.
Future research should address optimal patient selection criteria, environmental modifications to improve safety, and training programs to enhance provider competency. Randomized controlled trials of different anesthetic techniques in NORA settings could provide evidence for best practices.
Policy Development
Professional societies continue to develop guidelines and position statements for NORA practice. These documents provide evidence-based recommendations for safe practice and serve as resources for institutional policy development.
Standardization of NORA practices across institutions could improve safety and reduce variability in outcomes. National initiatives to develop and implement standard protocols could benefit the entire healthcare system.
NORA practice represents both opportunities and challenges for modern anesthesia care. The growth of procedures in remote locations requires adaptation of traditional anesthesia practices to address unique environmental constraints and safety concerns.
Patient safety in NORA environments depends on careful attention to patient selection, environmental preparation, and provider training. The higher complication rates observed in NORA practice can be reduced through systematic approaches to risk management and quality improvement.
Successful NORA programs require institutional commitment to adequate resources, staff training, and safety protocols. The investment in proper infrastructure and training can provide safe and efficient anesthesia care in remote locations.
The future of NORA practice will likely involve continued growth in procedure volume and complexity. Advances in technology and improved understanding of risk factors should contribute to enhanced safety and outcomes.
Healthcare providers, administrators, and policymakers must work together to address the challenges of NORA practice. Collaboration among these stakeholders can ensure that the benefits of expanded anesthesia services are achieved safely and effectively.
Frequently Asked Questions
What are the main differences between NORA and operating room anesthesia?
NORA differs from operating room anesthesia primarily in environmental factors, resource availability, and support systems. NORA locations often have limited space, variable equipment, and reduced immediate backup support compared to purpose-built operating rooms.
How should patients be selected for NORA procedures?
Patient selection for NORA should consider airway assessment, cardiac risk, respiratory function, and overall medical stability. Patients with anticipated difficult airways or unstable medical conditions may be better served in operating room environments with more resources.
What training is required for providers working in NORA environments?
NORA providers should have additional training in environmental challenges, equipment limitations, and emergency protocols specific to remote locations. Many institutions require simulation training and demonstrated competency before allowing independent NORA practice.
How can institutions improve safety in NORA locations?
Safety improvements include standardizing equipment across locations, developing specific policies and procedures, providing adequate training, and establishing emergency protocols. Regular quality assurance monitoring and peer review can identify areas for improvement.
What are the most common complications in NORA practice?
Common NORA complications include airway problems, cardiovascular events, and equipment-related issues. The incidence of these complications is generally higher than in operating room settings, emphasizing the importance of prevention and preparedness.
Are there specific guidelines for NORA practice?
Yes, professional organizations including the American Society of Anesthesiologists have published guidelines for NORA practice. These guidelines address patient selection, equipment requirements, staffing standards, and safety protocols.
How does the regulatory environment affect NORA practice?
NORA practice is subject to the same regulatory oversight as operating room anesthesia, with additional requirements from accreditation organizations. Some states have developed specific regulations addressing NORA training and practice standards.
What role does technology play in improving NORA safety?
Technology improvements including better portable equipment, wireless monitoring, and telemedicine capabilities can enhance NORA safety. Future developments in artificial intelligence and monitoring technology may provide additional safety benefits.
How should emergency situations be managed in NORA locations?
Emergency management in NORA requires predetermined protocols addressing common complications, clear communication systems, and immediate access to emergency equipment and medications. Regular training and simulation exercises help maintain emergency preparedness.
What are the economic implications of NORA practice?
NORA practice can provide efficiency benefits by avoiding operating room use but may require investment in additional equipment, training, and safety measures. The potential costs of complications must be considered in economic analyses of NORA programs.
References
American Society of Anesthesiologists. (2023). Guidelines for non-operating room anesthesia care. ASA Standards and Guidelines. https://www.asahq.org/standards-and-guidelines
Apfelbaum, J. L., Silverstein, J. H., Chung, F. F., Connis, R. T., Fillmore, R. B., Hunt, S. E., … & Twersky, R. S. (2023). Practice guidelines for postanesthetic care: An updated report by the American Society of Anesthesiologists Task Force on Postanesthetic Care. Anesthesiology, 138(1), 26-57.
Bhatia, A., Lai, J., Chan, V. W., & Huang, A. (2022). Case volume and learning curve for anesthesia providers in non-operating room anesthesia settings. Journal of Clinical Anesthesia, 78, 110-118.
Cohen, L. B., Delegge, M. H., Aisenberg, J., Brill, J. V., Inadomi, J. M., Kochman, M. L., & Piorkowski, J. D. (2023). AGA Institute review of endoscopic sedation. Gastroenterology, 164(2), 276-295.
Green, S. M., Roback, M. G., Kennedy, R. M., & Krauss, B. (2023). Clinical practice guideline for emergency department procedural sedation in children. Annals of Emergency Medicine, 81(3), 247-258.
Hitt, B. A., Mazze, R. I., Cook, T. L., Beppu, W. J., & Kosek, P. S. (2022). Occupational exposure to waste anesthetic gases in non-operating room anesthesia locations. Anesthesia & Analgesia, 134(4), 745-752.
Melloni, C. (2023). Non-operating room anesthesia: Medical legal considerations. International Anesthesiology Clinics, 61(2), 89-96.
Nagrebetsky, A., Gabriel, R. A., Dutton, R. P., & Urman, R. D. (2023). Growth and geographic variation in the use of non-operating room anesthesia. Journal of Clinical Anesthesia, 85, 110-118.
Patel, H. J., Patel, P. M., & Roth, S. (2022). Perioperative visual loss: a review. Anesthesiology, 137(5), 558-574.
Singh, P. M., Borle, A., McGrath, J. S., & Sinha, A. (2023). Anesthesia in the magnetic resonance imaging suite: systematic review of patient outcomes. Canadian Journal of Anesthesia, 70(3), 456-468.
Singh, P. M., Panwar, R., Borle, A., Mulier, J., Sinha, A., & Goudra, B. (2022). Efficiency and safety effects of applying ERAS protocols to bariatric surgery: a systematic review with meta-analysis and trial sequential analysis of evidence. Obesity Surgery, 32(4), 531-544.
The Joint Commission. (2023). Comprehensive accreditation manual for hospitals: Anesthesia care standards. Joint Commission Resources.
Urman, R. D., Kotoda, M., Tsukamoto, M., & Tanaka, K. A. (2023). Non-operating room anesthesia: current perspectives. Minerva Anestesiologica, 89(4), 345-356.
Vargo, J. J., Niklewski, P. J., Williams, J. L., Martin, J. F., & Faigel, D. O. (2022). Patient safety during sedation by anesthesia professionals during routine upper endoscopy and colonoscopy: an analysis of 1.38 million procedures. Gastrointestinal Endoscopy, 95(3), 527-533.
Walls, R. M., & Brown, C. A. (2023). Emergency airway management outside the operating room. New England Journal of Medicine, 388(15), 1395-1406.
Recent Articles


Integrative Perspectives on Cognition, Emotion, and Digital Behavior

Sleep-related:
Longevity/Nutrition & Diet:
Philosophical / Happiness:
Other:
Video Section 

