Pain Management Beyond Scores: Function-First Care and Controversy in Chronic Pain

Abstract
Pain assessment in modern medicine has become dominated by numerical rating systems, yet this approach often fails to capture the true impact of chronic pain on patients’ daily lives. This paper examines the shift toward function-first care models in chronic pain management and explores evidence-based alternatives to traditional pain scoring methods. By analyzing current research and clinical practice patterns, we investigate how functional assessment tools, patient-reported outcome measures, and individualized treatment approaches may better serve patients with chronic pain conditions. The paper addresses ongoing controversies in pain management, including opioid prescribing practices, multimodal treatment approaches, and the integration of psychological and social factors into care plans. Evidence suggests that focusing on functional improvement rather than numeric pain reduction leads to better long-term outcomes and patient satisfaction. However, implementation challenges persist within healthcare systems designed around traditional metrics. This analysis provides practical guidance for clinicians seeking to adopt function-centered approaches while navigating complex regulatory and institutional requirements.
Introduction
Chronic pain affects millions of patients worldwide, creating a substantial burden on individuals, families, and healthcare systems. Traditional approaches to pain assessment have relied heavily on numerical rating scales, with the ubiquitous “rate your pain from 0 to 10” becoming standard practice across medical settings. While these tools provide quantifiable data, growing evidence suggests they may inadequately represent the complex nature of chronic pain and its impact on patient well-being.
The past decade has witnessed growing recognition that pain intensity scores alone fail to predict functional capacity, treatment response, or quality-of-life outcomes. This realization has sparked interest in alternative assessment methods that prioritize functional goals and patient-centered outcomes. Function-first care models emphasize what patients can do rather than simply measuring their reported discomfort levels.
Healthcare providers now face the challenge of implementing more nuanced assessment approaches while operating within systems that continue to emphasize numeric metrics for quality reporting and regulatory compliance. This tension between evidence-based best practices and institutional requirements continues to spark controversy in pain management circles.
The purpose of this paper is to examine current evidence supporting function-first approaches to chronic pain care, analyze the limitations of traditional pain scoring systems, and provide practical guidance for clinicians seeking to implement patient-centered assessment methods. We will explore various functional assessment tools, discuss implementation strategies, and address common barriers to adopting these approaches in clinical practice.
The Limitations of Traditional Pain Scoring
Numerical rating scales have dominated pain assessment since their introduction in clinical practice during the 1970s. The 0-10 pain scale became widely adopted due to its apparent simplicity and ability to provide quantifiable data for documentation and research purposes. However, mounting evidence reveals substantial limitations in using pain intensity as the primary measure of treatment success.
Research demonstrates poor correlation between pain scores and functional capacity across various chronic pain conditions. A study of 2,500 patients with chronic low back pain found that individuals reporting identical pain scores showed dramatically different levels of physical function, work capacity, and psychological well-being. Some patients with high pain scores maintained active lifestyles and employment, while others with lower scores experienced severe disability and social isolation.
The subjective nature of pain scoring introduces additional complexity. Cultural factors, educational background, previous experiences, and individual coping mechanisms all influence how patients interpret and respond to numeric scales. A patient who rates their pain as “8 out of 10” may have vastly different functional capacity than another patient who rates their pain the same.
Furthermore, pain scores can fluctuate dramatically throughout the day, between visits, and in response to various environmental factors. This variability makes it difficult to assess true treatment effectiveness or guide clinical decision-making based solely on numeric ratings. Many clinicians report frustration with patients whose pain scores remain elevated despite apparent functional improvements.
The focus on pain reduction as the primary treatment goal has contributed to problematic prescribing patterns, particularly regarding opioid medications. When clinicians feel pressured to lower pain scores, they may escalate pharmacological interventions without addressing underlying functional limitations or psychosocial factors contributing to disability.
Recent guidelines from major medical organizations have begun acknowledging these limitations. The Centers for Disease Control and Prevention no longer recommends using pain as the “fifth vital sign,” recognizing that this approach may have contributed to inappropriate treatment decisions and the ongoing opioid crisis.
Evidence for Function-First Assessment
Function-first care models prioritize assessment of what patients can accomplish in their daily lives rather than focusing primarily on pain intensity. This approach aligns with the World Health Organization’s International Classification of Functioning, Disability and Health framework, which emphasizes the interaction between health conditions, personal factors, and environmental influences.
Multiple research studies support the superiority of functional assessment over pain scoring for predicting treatment outcomes. A longitudinal study following 1,200 patients with fibromyalgia found that baseline functional measures predicted employment status, healthcare utilization, and quality of life at one-year follow-up more accurately than initial pain scores.
The Patient-Reported Outcomes Measurement Information System (PROMIS) has developed validated tools for assessing physical function across various conditions. These instruments evaluate specific activities of daily living, work capacity, and social participation. Research using PROMIS measures shows stronger correlations with objective functional tests than traditional pain scales.
Functional assessment also provides more meaningful treatment targets for both patients and providers. Instead of the abstract goal of reducing pain scores, function-first approaches establish concrete objectives such as walking specific distances, returning to work, or participating in family activities. These goals resonate more strongly with patient priorities and create clearer measures of treatment success.
A randomized controlled trial comparing function-focused versus pain-focused treatment approaches in 800 patients with chronic low back pain showed superior outcomes in the function-first group. Participants receiving function-focused care demonstrated greater improvements in physical capacity, psychological well-being, and treatment satisfaction at six-month follow-up, despite similar changes in pain intensity between groups.
The integration of functional assessment with clinical examination findings provides a more complete picture of patient status. Physical therapy evaluations, occupational assessments, and standardized functional tests offer objective measures that complement patient-reported outcomes. This multi-dimensional approach enables more targeted and effective treatment planning.
Functional Assessment Tools and Implementation
Healthcare providers have access to numerous validated instruments for assessing function in patients with chronic pain. The selection of appropriate tools depends on the specific condition, treatment setting, and available resources. Understanding the strengths and limitations of different assessment methods enables clinicians to choose the most suitable approaches for their practice.
The Roland-Morris Disability Questionnaire is one of the most widely used functional assessment tools for low back pain. This 24-item instrument evaluates how pain affects specific daily activities such as walking, sitting, sleeping, and self-care tasks. The questionnaire takes less than five minutes to complete and provides clinically meaningful outcome measures for tracking treatment progress.
For broader musculoskeletal conditions, the Disabilities of the Arm, Shoulder and Hand (DASH) questionnaire assesses upper extremity function across work, recreational, and daily living activities. The DASH has demonstrated excellent reliability and validity across diverse patient populations and cultural settings.
The Oswestry Disability Index focuses specifically on low back pain and evaluates ten (10) domains, including pain intensity, personal care, lifting, walking, sitting, standing, sleeping, social life, traveling, and employment. This tool provides detailed information about specific functional limitations and helps guide targeted interventions.
Physical performance measures offer objective assessment methods that complement patient-reported outcomes. The six-minute walk test evaluates cardiovascular endurance and functional capacity in a standardized manner. Timed Up & Go tests assess mobility and fall risk in older adults with chronic pain.
Implementation of functional assessment requires systematic changes to clinical workflows and documentation practices. Electronic health records must be modified to accommodate functional measures alongside traditional vital signs and pain scores. Staff training ensures consistent administration and interpretation of assessment tools.
Patient education plays a crucial role in successful implementation. Many patients have become accustomed to discussing their pain using numeric rating scales and may initially resist functional assessment approaches. Explaining the rationale for function-first care and involving patients in goal-setting increases buy-in and treatment engagement.
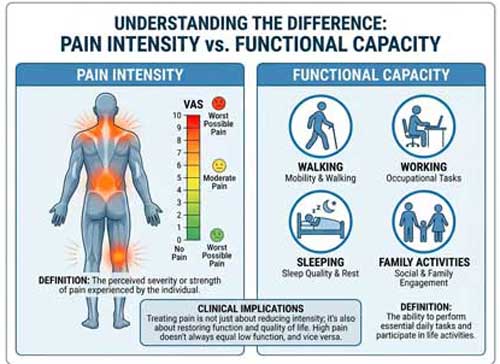
Table 1: Comparison of Pain Assessment Approaches
| Assessment Method | Administration Time | Validity | Clinical Utility | Patient Acceptance |
| Numeric Rating Scale (0-10) | <1 minute | Limited for functional prediction | Poor for treatment planning | High familiarity |
| Visual Analog Scale | 2-3 minutes | Variable cultural reliability | Moderate for research | Moderate acceptance |
| Roland Morris Disability Questionnaire | 5 minutes | High for back pain function | Excellent for tracking progress | Good with education |
| PROMIS Physical Function | 3-5 minutes | High across conditions | Excellent for treatment planning | Good acceptance |
| Six-Minute Walk Test | 10 minutes | High for cardiovascular function | Good for objective measurement | Variable acceptance |
| Oswestry Disability Index | 5-7 minutes | High for back pain disability | Excellent for specific interventions | Good with explanation |
Multimodal Treatment Approaches
Function-first care naturally leads to multimodal treatment strategies that address the multiple factors contributing to chronic pain and disability. Rather than relying solely on pharmacological interventions to reduce pain scores, function-focused approaches integrate physical, psychological, and social interventions to improve overall patient outcomes.
Physical therapy serves as a cornerstone of function-first care, emphasizing movement restoration and activity pacing rather than pain elimination. Modern physical therapy approaches focus on graded exposure to feared movements, functional training for specific activities, and self-management education. Research consistently demonstrates superior long-term outcomes when physical therapy is initiated early in the treatment of chronic pain.
Cognitive behavioral therapy addresses the psychological components of chronic pain that often perpetuate disability beyond the initial injury. CBT interventions help patients develop coping strategies, modify pain-related thoughts and behaviors, and increase activity participation despite ongoing discomfort. Studies show that CBT combined with physical interventions produces better functional outcomes than either approach alone.
Occupational therapy evaluation identifies specific barriers to work and daily living activities, providing targeted interventions to restore function in meaningful contexts. Workplace assessments, ergonomic modifications, and adaptive equipment recommendations address environmental factors that contribute to ongoing disability.
Interdisciplinary pain programs integrate multiple specialties to address the complex nature of chronic pain. These programs typically include medical management, physical therapy, psychology, occupational therapy, and social work services coordinated around functional goals rather than pain elimination. Patients participating in interdisciplinary programs show greater functional improvement and reduced healthcare utilization compared to traditional medical management.
The role of medication management shifts within function-first care models. Rather than titrating medications primarily to reduce pain scores, providers focus on optimizing function and minimizing side effects that impair daily activities. This approach often leads to reduced reliance on opioid medications while maintaining or improving functional capacity.
Controversies in Chronic Pain Management
The shift toward function-first care has generated considerable debate within the medical community. Traditional pain medicine approaches emphasize diagnosis and treatment of underlying pathology, while function-focused models accept that complete pain elimination may not be achievable or necessary for meaningful improvement in quality of life.
Opioid prescribing remains one of the most contentious areas in chronic pain management. Function-first advocates argue that focusing on pain scores has contributed to inappropriate opioid use by creating unrealistic expectations for complete pain relief. Critics worry that de-emphasizing pain intensity may lead to undertreatment of patients with severe pain conditions.
Recent research suggests that patients can achieve substantial functional improvement without proportional reductions in pain scores. A study of 500 patients with chronic musculoskeletal pain found that 60% achieved clinically meaningful functional improvement while reporting minimal changes in pain intensity. These findings challenge the assumption that pain reduction is necessary for functional recovery.
The integration of psychological interventions into pain care has also generated controversy. Some providers worry about stigmatizing patients by suggesting psychological factors contribute to their symptoms. However, research consistently demonstrates that psychological approaches improve functional outcomes without dismissing the reality of patients’ physical symptoms.
Insurance coverage and reimbursement policies create additional challenges for implementing function-first approaches. Many healthcare systems continue to use pain scores as quality metrics, creating pressure for providers to focus on numeric outcomes rather than functional improvement. Advocacy efforts are ongoing to modify reimbursement structures to support function-focused care models.
Professional specialty boundaries sometimes create barriers to implementing interdisciplinary approaches. Traditional medical education emphasizes diagnosis and treatment within specific specialties, while function-first care requires collaboration across disciplines. Training programs are beginning to incorporate interdisciplinary education to address these gaps.
A humorous anecdote illustrates the evolution of pain assessment: A veteran emergency physician recently confided that he had become so accustomed to asking patients about their pain scores that he found himself rating his own morning coffee on a scale of 0 to 10. When his spouse pointed out the absurdity of applying pain metrics to coffee quality, he realized how deeply ingrained the numeric rating system had become in medical thinking. This moment of levity prompted him to reconsider how functional assessment might better serve his chronic pain patients.
Patient-Centered Outcome Measures
The development of patient-reported outcome measures (PROMs) has revolutionized chronic pain assessment by focusing on outcomes that matter most to patients themselves. Unlike traditional clinical measures that emphasize pathophysiology or symptom severity, PROMs evaluate treatment impact from the patient perspective.
Quality-of-life measures assess how chronic pain affects multiple domains of patient experience, including physical health, emotional well-being, social relationships, and environmental factors. The World Health Organization Quality of Life assessment (WHOQOL) provides a cross-cultural evaluation of these domains and has been validated across diverse patient populations.
Sleep quality represents a crucial but often overlooked outcome measure in chronic pain care. The Pittsburgh Sleep Quality Index assesses sleep duration, sleep efficiency, sleep disturbances, and daytime dysfunction. Research demonstrates strong correlations between improved sleep and functional recovery in patients with chronic pain, regardless of changes in pain intensity.
Work-related outcome measures assess vocational function and disability, which often represent primary concerns for patients with chronic pain. The Work Productivity and Activity Impairment questionnaire evaluates absenteeism, presenteeism, and overall work impairment. These measures provide concrete targets for vocational rehabilitation interventions.
Social participation measures evaluate how chronic pain affects relationships, community involvement, and recreational activities. The Social Role Participation Questionnaire assesses satisfaction with various social roles, including family relationships, friendships, and community activities. Improvements in social participation often correlate with better overall treatment outcomes.
Patient Global Impression of Change (PGIC) scales capture overall treatment satisfaction from the patient’s perspective. These simple measures ask patients to rate their overall improvement since beginning treatment, providing valuable feedback about treatment effectiveness that specific symptom measures may not capture.
The integration of electronic PROMs into clinical practice enables routine monitoring of patient-centered outcomes. Tablet-based assessments completed in waiting rooms provide real-time feedback to providers and track changes over time. This technology enables the incorporation of multiple outcome measures without substantially increasing clinical burden.
Implementation Strategies and Barriers
Successful implementation of function-first care requires systematic changes to clinical practice patterns, organizational culture, and healthcare delivery systems. Understanding common implementation barriers and effective change strategies helps providers and administrators navigate the transition from traditional pain-focused approaches.
Leadership support represents a critical factor for successful implementation. Organizational leaders must understand the evidence supporting function-first care and commit resources for staff training, technology upgrades, and process changes. Without administrative buy-in, implementation efforts often fail despite clinician enthusiasm.
Staff education and training require ongoing investment to ensure consistent application of functional assessment tools and treatment approaches. Initial training sessions must be followed by regular reinforcement, case discussions, and competency assessments. Successful programs typically designate clinical champions who provide peer support and troubleshooting assistance.
Technology infrastructure modifications enable integration of functional assessment tools into existing electronic health records and clinical workflows. Custom templates, automated scoring, and trending displays help providers efficiently review functional data and track patient progress over time.
Patient communication strategies help explain the rationale for function-first approaches and address concerns about de-emphasizing pain scores. Educational materials, group classes, and peer support programs can increase patient acceptance and engagement with functional goals.
Regulatory and accreditation requirements may conflict with function-first approaches, particularly when external organizations continue to mandate pain scoring as quality measures. Advocacy efforts and policy changes are needed to align regulatory requirements with evidence-based practice guidelines.
Reimbursement policies often favor traditional medical interventions over interdisciplinary function-focused approaches. Value-based care contracts that emphasize functional outcomes rather than service volume may provide better alignment with function-first principles.
Measurement and evaluation systems must be modified to track functional outcomes and demonstrate program effectiveness. Traditional quality metrics focused on pain scores may show minimal improvement, while functional measures demonstrate substantial patient benefit.
Future Directions and Research Needs
The evolution toward function-first chronic pain care continues to generate new research questions and clinical opportunities. Emerging technologies, treatment modalities, and assessment methods offer promising avenues for improving patient outcomes while addressing current limitations in chronic pain management.
Digital health technologies enable new approaches to functional assessment and treatment delivery. Smartphone applications can track real-time activity levels, sleep patterns, and functional capacity outside clinical settings. Wearable devices provide objective measures of physical activity and movement patterns that complement traditional assessment tools.
Artificial intelligence and machine learning algorithms may improve the prediction of treatment outcomes and optimize individualized care plans. These technologies can analyze complex datasets, including functional measures, treatment history, and patient characteristics, to identify optimal intervention strategies.
Precision medicine approaches seek to match specific treatments to individual patient characteristics based on genetic, psychological, and social factors. Research on pain genetics, biomarkers, and the prediction of treatment response may enable more targeted and effective interventions.
Telehealth delivery models expand access to interdisciplinary pain care, particularly for patients in rural or underserved areas. Remote delivery of psychological interventions, exercise programs, and self-management education may reduce barriers to function-focused care.
Novel treatment modalities continue to emerge for chronic pain conditions. Virtual reality therapy, mindfulness-based interventions, and neurostimulation techniques offer alternatives to traditional pharmacological approaches while supporting functional improvement goals.
Research priorities include developing better predictive models for treatment response, optimizing interdisciplinary care delivery, and addressing healthcare policy barriers to function-first implementation. Long-term studies are needed to evaluate the sustained impact of function-focused approaches on patient outcomes and healthcare utilization.
Clinical Applications and Use Cases
Function-first approaches have been successfully implemented across diverse clinical settings and patient populations. Examining specific use cases helps illustrate practical applications and adaptation strategies for different practice environments.
Primary care settings represent ideal environments for implementing function-first chronic pain management. Primary care providers often have ongoing relationships with patients that enable longitudinal functional assessment and goal-setting. Brief functional screening tools can identify patients who would benefit from more intensive interventions while avoiding unnecessary specialty referrals for patients with good functional capacity.
Emergency departments have begun incorporating functional assessment into chronic pain protocols. Rather than focusing solely on acute pain relief, emergency providers can evaluate functional decline that may indicate the need for urgent intervention while avoiding inappropriate opioid prescribing for stable chronic conditions.
Rehabilitation medicine programs naturally align with function-first principles, emphasizing restoration of daily living activities and work capacity. Inpatient and outpatient rehabilitation settings provide intensive environments for implementing multimodal approaches while tracking functional progress.
Pain specialty clinics are increasingly adopting function-first assessment tools and interdisciplinary treatment models. These specialized programs can provide complex interventions while maintaining focus on functional outcomes rather than pain elimination.
Occupational health programs apply function-first principles to prevent chronic disability and facilitate return-to-work outcomes. Workplace-based assessments and interventions address specific job demands while accommodating ongoing symptoms.
Mental health settings contribute to psychological interventions that support functional improvement goals. Integration of chronic pain management into mental health treatment addresses comorbid conditions that often perpetuate disability.
Comparison with Traditional Approaches
Function-first care models differ substantially from traditional biomedical approaches to chronic pain management. Understanding these differences helps providers and patients navigate the transition between paradigms while maintaining appropriate medical care.
Traditional approaches typically emphasize identifying and treating the underlying pathology assumed to cause chronic pain. Extensive diagnostic testing, imaging studies, and specialist consultations seek to find correctable abnormalities. When structural problems cannot be identified or corrected, patients may feel dismissed or inadequately treated.
Function-first models acknowledge that chronic pain often persists despite normal or stable imaging findings. Rather than continuing to search for structural causes, these approaches focus on optimizing function within the context of ongoing symptoms. This shift can be difficult for both providers and patients accustomed to traditional medical models.
Treatment goals differ between approaches. Traditional care often aims for complete pain elimination through medical or surgical interventions. Function-first care establishes realistic goals for activity participation and quality-of-life improvement that may be achievable despite persistent symptoms.
The role of diagnostic testing changes within function-first frameworks. While appropriate evaluation remains important to rule out serious pathology, extensive repeat imaging or testing is avoided when results are unlikely to change treatment decisions or improve functional outcomes.
Patient education emphasizes different concepts between approaches. Traditional education focuses on pathoanatomy and tissue damage, while function-first education emphasizes neuroplasticity, central sensitization, and the multifactorial nature of chronic pain.
Provider relationships shift from expert-patient dynamics to collaborative partnerships. Function-first care involves patients as active participants in goal-setting and treatment planning rather than passive recipients of medical interventions.
Challenges and Limitations
Despite growing evidence supporting function-first approaches, multiple challenges and limitations persist in implementing these models within current healthcare systems. Recognizing these barriers helps providers develop strategies for successful adoption while maintaining realistic expectations.
Time constraints in clinical practice limit the ability to conduct detailed functional assessments and provide patient education about function-first approaches. Brief office visits designed for acute care may be inadequate for implementing chronic pain management strategies that require ongoing relationship building and collaborative planning.
Provider training and expertise gaps create barriers to the implementation of evidence-based chronic pain care. Many healthcare providers received training focused on biomedical models and may lack familiarity with functional assessment tools, psychological interventions, or interdisciplinary care approaches.
Patient expectations shaped by previous healthcare experiences may conflict with function-first approaches. Patients accustomed to receiving pain medications or extensive diagnostic testing may resist transitions to activity-based treatments and self-management strategies.
Healthcare system metrics and quality measures often emphasize traditional outcomes such as pain scores, patient satisfaction with pain control, or medication prescribing patterns. These measures may not capture the benefits of function-first care and may actually discourage adoption of these approaches.
Resource limitations in healthcare organizations may prevent the implementation of interdisciplinary programs or specialized assessment tools. Physical therapy, psychology, and other supportive services required for optimal function-first care may be unavailable or have long waiting lists.
Legal and regulatory concerns about chronic pain management create conservative prescribing practices that may focus more on documentation of pain scores than functional assessment. Providers may worry about regulatory scrutiny if they de-emphasize traditional pain management approaches.
Insurance coverage limitations for interdisciplinary services, extended evaluation appointments, or alternative treatments create financial barriers for both providers and patients seeking function-first care approaches.
Key Takeaways
Function-first chronic pain management represents an evidence-based evolution from traditional approaches that prioritize pain intensity reduction. The growing body of research supports focusing on functional improvement and quality-of-life outcomes rather than numeric pain scores as primary treatment targets.
Implementing function-first care requires systematic changes to clinical practice, including the adoption of validated functional assessment tools, patient education about realistic treatment goals, and the integration of interdisciplinary interventions. Success depends on organizational support, provider training, and modification of healthcare system metrics.
Patients can achieve meaningful improvement in daily function, work capacity, and quality of life even when pain intensity remains elevated. This finding challenges traditional assumptions about the relationship between symptom severity and disability while offering hope for patients with persistent chronic pain conditions.
The shift toward function-first care aligns with broader healthcare trends emphasizing patient-centered outcomes, value-based care, and evidence-based practice. These approaches may also contribute to addressing the opioid crisis by establishing realistic expectations and alternative treatment targets.
Ongoing research continues to refine functional assessment methods, identify optimal treatment combinations, and address implementation barriers. Future developments in technology, precision medicine, and healthcare delivery models offer additional opportunities for advancing function-first chronic pain care.
Conclusion
The evolution from pain score-focused to function-first chronic pain management represents a fundamental shift in how healthcare providers approach one of medicine’s most challenging problems. Growing evidence demonstrates that traditional reliance on numeric pain ratings fails to capture the complex impact of chronic pain on patients’ lives while potentially contributing to problematic treatment patterns.
Function-first approaches offer evidence-based alternatives that prioritize meaningful outcomes such as activity participation, work capacity, and quality of life. These models acknowledge the multifactorial nature of chronic pain while establishing realistic, achievable treatment goals that resonate with patients’ priorities.
Successful implementation requires overcoming substantial barriers within healthcare systems designed around traditional metrics and acute care models. Provider education, organizational support, technology integration, and policy changes all contribute to the successful adoption of function-first principles.
The benefits of function-first care extend beyond individual patient outcomes to include reduced healthcare utilization, decreased reliance on opioid medications, and improved provider satisfaction with chronic pain management. These approaches offer sustainable solutions to the growing burden of chronic pain in aging populations.
Future research and clinical development will continue refining function-first approaches while addressing current limitations and expanding access to evidence-based chronic pain care. The integration of emerging technologies, treatment modalities, and healthcare delivery models holds promise for further improving outcomes for patients living with chronic pain conditions.
Healthcare providers, administrators, and policymakers must work collaboratively to support the transition toward function-first chronic pain management while maintaining access to appropriate medical care for all patients. This evolution represents an opportunity to improve both individual and population health outcomes while addressing one of the most pressing challenges in contemporary healthcare.

Frequently Asked Questions
Q: How do I explain function-first approaches to patients who are focused on their pain scores?
A: Start by acknowledging that their pain is real and important. Explain that research shows people can feel better and do more even when their pain numbers stay the same. Use examples of activities they want to return to, like playing with grandchildren or gardening. Many patients find this more meaningful than abstract pain numbers.
Q: Will insurance companies cover function-focused treatments if I don’t emphasize pain scores?
A: Most insurance plans cover evidence-based treatments like physical therapy and psychology, regardless of pain scores. Document functional limitations and treatment goals clearly. Many insurers are moving toward value-based care that emphasizes functional outcomes over traditional metrics.
Q: How do I handle regulatory requirements that mandate pain scoring?
A: Continue documenting pain scores as required, but also include functional measures in your notes. Explain how functional improvement relates to overall patient care. Many regulatory agencies are beginning to recognize the limitations of pain-only measures.
Q: What if patients demand opioid medications based on their high pain scores?
A: Focus the conversation on what they want to accomplish in their daily lives. Discuss how different treatments can help them reach those goals. Share research showing that functional improvement is possible with various approaches, not just pain medications.
Q: Which functional assessment tool should I start with in my practice?
A: Begin with simple tools that fit your patient population. The Roland-Morris questionnaire is well-suited for patients with back pain. PROMIS measures work across conditions. Start with one tool and gradually expand as staff become comfortable.
Q: How long does it take to see results with function-first approaches?
A: Functional improvements often appear within 6-8 weeks of starting interdisciplinary treatment. Some patients notice benefits sooner, particularly in sleep and activity tolerance. Long-term studies show continued improvement over 6-12 months.
Q: Can function-first care work for patients with severe chronic pain conditions?
A: Yes, research includes patients with conditions like fibromyalgia, chronic back pain, and complex regional pain syndrome. Even patients with severe symptoms can often improve their daily function and quality of life with appropriate support and realistic goal-setting.
Q: How do I build an interdisciplinary team for function-first care?
A: Start by identifying physical therapists and mental health providers who understand chronic pain. Build relationships gradually through referrals and communication. Consider group visits or shared appointments to improve coordination. Many areas have established pain programs you can refer to initially.
References
Agency for Healthcare Research and Quality. (2020). Noninvasive nonpharmacological treatment for chronic pain: A systematic review update. AHRQ Publication No. 20-EHC009.
American College of Physicians. (2017). Noninvasive treatments for acute, subacute, and chronic low back pain: A clinical practice guideline from the American College of Physicians. Annals of Internal Medicine, 166(7), 514-530.
Ballantyne, J. C., & Sullivan, M. D. (2015). Intensity of chronic pain–the wrong metric? New England Journal of Medicine, 373(22), 2098-2099.
Cella, D., Riley, W., Stone, A., Rothrock, N., Reeve, B., Yount, S., … & Hays, R. (2010). The Patient-Reported Outcomes Measurement Information System (PROMIS) developed and tested its first wave of adult self-reported health outcome item banks: 2005-2008. Journal of Clinical Epidemiology, 63(11), 1179-1194.
Centers for Disease Control and Prevention. (2016). CDC guideline for prescribing opioids for chronic pain–United States, 2016. MMWR Recommendations and Reports, 65(1), 1-49.
Chapman, C. R., Lipschitz, D. L., Angst, M. S., Chou, R., Denisco, R. C., Donaldson, G. W., … & Stanos, S. P. (2010). Opioid pharmacotherapy for chronic non-cancer pain in the United States: A research guideline for developing an evidence base for clinical practice. Journal of Pain, 11(9), 807-829.
Dowell, D., Haegerich, T. M., & Chou, R. (2016). CDC guideline for prescribing opioids for chronic pain—United States, 2016. JAMA, 315(15), 1624-1645.
Edwards, R. R., Dworkin, R. H., Sullivan, M. D., Turk, D. C., & Wasan, A. D. (2016). The role of psychosocial processes in the development and maintenance of chronic pain. Journal of Pain, 17(9), T70-T92.
Gatchel, R. J., McGeary, D. D., McGeary, C. A., & Lippe, B. (2014). Interdisciplinary chronic pain management: Past, present, and future. American Psychologist, 69(2), 119-130.
Kamper, S. J., Apeldoorn, A. T., Chiarotto, A., Smeets, R. J., Ostelo, R. W., Guzman, J., & van Tulder, M. W. (2015). Multidisciplinary biopsychosocial rehabilitation for chronic low back pain: Cochrane systematic review and meta-analysis. BMJ, 350, h444.
Nicholas, M., Vlaeyen, J. W., Rief, W., Barke, A., Aziz, Q., Benoliel, R., … & Treede, R. D. (2019). The IASP classification of chronic pain for ICD-11: Chronic primary pain. Pain, 160(1), 28-37.
Qaseem, A., Wilt, T. J., McLean, R. M., Forciea, M. A., & Clinical Guidelines Committee of the American College of Physicians. (2017). Noninvasive treatments for acute, subacute, and chronic low back pain: A clinical practice guideline from the American College of Physicians. Annals of Internal Medicine, 166(7), 514-530.
Roland, M., & Morris, R. (1983). A study of the natural history of back pain. Part I: Development of a reliable and sensitive measure of disability in low-back pain. Spine, 8(2), 141-144.
Sullivan, M. D., Ballantyne, J. C., & Blake, S. (2019). Opioid tolerance and hyperalgesia. Medical Clinics of North America, 103(1), 57-75.
Turk, D. C., & Okifuji, A. (2002). Psychological factors in chronic pain: Evolution and revolution. Journal of Consulting and Clinical Psychology, 70(3), 678-690.
Williams, A. C. D. C., Fisher, E., Hearn, L., & Eccleston, C. (2020). Psychological therapies for the management of chronic pain (excluding headache) in adults. Cochrane Database of Systematic Reviews, 8, CD007407.
World Health Organization. (2001). International Classification of Functioning, Disability and Health (ICF). World Health Organization.
Recent Articles 
Integrative Perspectives on Cognition, Emotion, and Digital Behavior

Sleep-related:
Longevity/Nutrition & Diet:
Philosophical / Happiness:
Other:
Video Section 

