Seronegative Rheumatoid Arthritis vs Early Spondyloarthritis Which Diagnosis Is Right

Key Takeaways
Differentiating seronegative rheumatoid arthritis (RA) from early spondyloarthritis (SpA) remains one of the most challenging diagnostic tasks in contemporary rheumatology. Both conditions may present with inflammatory joint symptoms in the absence of definitive serologic markers, creating substantial clinical overlap during early disease stages. Evidence suggests that diagnostic misclassification affects nearly 9 percent of patients initially labeled with seronegative RA, often resulting in delayed initiation of appropriate therapy and suboptimal long term outcomes. Accurate early differentiation is therefore essential to guide targeted treatment strategies and prevent irreversible structural damage.
Seronegative rheumatoid arthritis refers to patients who meet clinical criteria for RA despite negative rheumatoid factor and anti cyclic citrullinated peptide antibodies. In contrast, spondyloarthritis encompasses a spectrum of inflammatory disorders characterized by axial involvement, enthesitis, and extra articular manifestations. Because antibody testing does not assist in distinguishing these entities, clinicians must rely heavily on careful pattern recognition supported by imaging and longitudinal clinical assessment.
Clinical presentation remains the most important initial diagnostic discriminator. Seronegative RA typically manifests as symmetrical polyarthritis predominantly affecting the small joints of the hands and feet, particularly the metacarpophalangeal and proximal interphalangeal joints. Persistent synovitis, prolonged morning stiffness, and progressive joint swelling are common features. By comparison, early spondyloarthritis more often presents with inflammatory back pain, asymmetric peripheral arthritis, enthesitis at tendon insertion sites, dactylitis, and associated conditions such as psoriasis, inflammatory bowel disease, or uveitis. Axial symptoms, improvement with exercise, nocturnal pain, and alternating buttock discomfort should raise suspicion for SpA rather than RA.
Diagnostic revision is not uncommon as disease patterns evolve over time. Longitudinal studies demonstrate that approximately 8.8 percent of patients initially diagnosed with seronegative RA ultimately receive a revised diagnosis of spondyloarthritis. This transition occurs more frequently in male patients and in individuals diagnosed before the age of 50 years, populations in which SpA prevalence is higher. These findings emphasize the importance of maintaining diagnostic flexibility and reassessing patients whose clinical course deviates from expected RA progression.
Therapeutic response patterns further highlight the clinical importance of accurate differentiation. Methotrexate and other conventional disease modifying antirheumatic drugs remain foundational therapies for rheumatoid arthritis and typically produce meaningful improvement in synovitis and disease activity. In contrast, axial spondyloarthritis often responds poorly to conventional synthetic disease modifying agents. Nonsteroidal anti inflammatory drugs serve as first line therapy in SpA, with tumor necrosis factor inhibitors and other biologic agents playing a central role when disease activity persists. Misdiagnosis may therefore expose patients to ineffective therapies while allowing ongoing inflammation and structural damage.
Advances in imaging have significantly improved diagnostic accuracy in antibody negative inflammatory arthritis. Musculoskeletal ultrasound can identify subclinical synovitis, enthesitis, and power Doppler signal indicative of active inflammation before findings become clinically apparent. Magnetic resonance imaging provides even greater sensitivity, particularly for detecting early sacroiliitis and bone marrow edema characteristic of spondyloarthritis. These modalities are especially valuable when physical examination findings are inconclusive and serologic testing does not clarify the diagnosis.
Early intervention remains a critical determinant of long term outcomes. Evidence indicates that initiating treatment within three months of symptom onset more than doubles the likelihood of achieving a favorable disease modifying antirheumatic drug response in seronegative rheumatoid arthritis. Similarly, early recognition and treatment of spondyloarthritis can reduce disease progression, improve functional outcomes, and limit structural damage. Delayed or incorrect diagnosis undermines this therapeutic window and contributes to persistent disease burden.
The diagnostic overlap between seronegative rheumatoid arthritis and early spondyloarthritis explains why confusion frequently arises in clinical practice. Both conditions may present with inflammatory joint pain, stiffness, and functional limitation, particularly during early stages when characteristic features are not fully developed. Nevertheless, careful evaluation of joint distribution, extra articular manifestations, demographic factors, imaging findings, and treatment response patterns enables clinicians to distinguish between these disorders with increasing precision.
Ultimately, establishing the correct diagnosis at the earliest possible stage ensures that patients receive disease specific therapy aligned with underlying pathophysiology. Accurate classification not only prevents unnecessary treatment delays but also improves long term disease control, preserves joint function, and enhances quality of life. As diagnostic tools and imaging technologies continue to advance, a systematic and pattern based approach remains central to optimizing outcomes in patients presenting with seronegative inflammatory arthritis.
Understanding Seronegative Rheumatoid Arthritis
What Makes RA Seronegative
Seronegative rheumatoid arthritis (SNRA) exists when patients display typical RA clinical features without detectable rheumatoid factor (RF) or anti-cyclic citrullinated peptide (ACPA) antibodies in serum [1]. The absence of these autoantibodies does not negate an RA diagnosis, as RF and ACPA presence is not required under current classification criteria [1]. Several mechanisms explain this seronegativity. Some patients produce antibodies at levels too low for standard laboratory detection [2]. Others may develop detectable antibodies later as disease progresses, shifting their diagnosis from seronegative to seropositive status [1].
The immunological basis differs between seronegative and seropositive forms. SNRA appears to rely more heavily on innate immune system activation rather than the adaptive immune responses that generate antibodies in seropositive cases [1]. Genetic patterns also diverge, with the HLA-B08/DRB103 haplotype appearing more frequently in seronegative patients [1]. In contrast, seropositive RA associates with different genetic markers and the shared epitope sequence that triggers anti-CCP antibody production [1].
Citrullination, the process by which smoking and other factors modify joint proteins to trigger autoimmune responses, plays a central role in seropositive disease [1]. The declining prevalence of smoking habits may partially explain rising SNRA incidence, as fewer patients undergo the protein modifications that lead to ACPA formation [1]. Additional factors potentially increasing SNRA rates include population aging, microbiome changes from chronic gut flora triggers, and occupational exposure to crystalline silica [1].
Seronegative Rheumatoid Arthritis Symptoms
Seronegative rheumatoid arthritis symptoms mirror those of seropositive disease. Joint manifestations include tenderness, swelling, and redness affecting hands, wrists, knees, ankles, hips, and elbows [1]. Morning stiffness persisting beyond 30 minutes represents a hallmark feature [1]. Symmetrical polyarthritis, where identical joints on both body sides become inflamed simultaneously, occurs regardless of antibody status [3]. Systemic manifestations extend beyond joints. Fatigue disproportionate to activity level affects most patients [4]. Red or dry eyes may develop [2]. Warmth radiates from inflamed joints upon palpation [3].
The clinical presentation shows subtle differences from seropositive RA. Rheumatoid nodules, firm subcutaneous lumps near affected joints, rarely appear in seronegative patients [2]. Vasculitis risk also decreases in the absence of antibodies [1]. However, claims that seronegative disease follows a milder course remain controversial [1]. Research demonstrates that disease activity scales show no differences between seronegative and seropositive groups [1]. Notably, seronegative patients begin treatment later in life, with disease onset occurring at 54 years versus 43 years in seropositive cases [1].
Ultrasound findings reveal less severe inflammation patterns in seronegative patients. Power Doppler signals appear less frequently in metacarpophalangeal joints of seronegative individuals (9% versus 53%) [1]. Erosions develop less commonly (9% versus 36% in the second MCP joint) [1]. Despite these imaging differences, long-term cardiovascular risk remains equivalent between both forms [1].
How Common Is Seronegative RA
Epidemiological data traditionally placed seronegative RA prevalence at 20 to 30 percent of total RA cases [1]. Approximately 20% of patients with RA test negative for both RF and anti-CCP antibodies [3][1]. Between 60% and 80% of RA patients demonstrate antibody positivity, leaving the remainder seronegative [2][1].
Recent decades show increasing SNRA incidence. Between 1985 and 1994, only 12 per 100,000 RA patients were seronegative [1]. That figure rose to 20 per 100,000 between 2005 and 2014 [1]. Population aging contributes to this trend, as late-onset RA in elderly patients commonly presents without antibodies [1]. The dysregulation of inflammatory processes characteristic of aging may underlie this association [1].
Environmental factors further explain shifting prevalence patterns. Reduced smoking rates decrease citrullination triggers, potentially increasing the ratio of seronegative to seropositive cases [1]. Obesity represents another risk factor associated with seronegative disease development [2][1]. The diagnostic landscape adds complexity to prevalence estimates. Many patients initially labeled with seronegative RA receive revised diagnoses over time. One study of nearly 10,000 seronegative RA patients found that more than 500 actually had spondyloarthritis, 275 had psoriatic arthritis, and 245 had axial spondyloarthritis [5]. This diagnostic drift suggests that reported SNRA prevalence may overestimate true rates, as some cases represent misclassified spondyloarthritis or other conditions.

Understanding Early Spondyloarthritis
Spondyloarthritis represents a heterogeneous disease family sharing clinical manifestations, radiological features, and genetic traits. The classification system divides this group into axial and peripheral forms based on predominant anatomic involvement, though approximately 30% of patients demonstrate both patterns simultaneously [1]. Understanding these distinctions becomes essential when differentiating spondyloarthritis vs rheumatoid arthritis, as misclassification rates exceed 8% in patients initially labeled with seronegative RA.
Types of Spondyloarthritis
Axial spondyloarthritis encompasses two clinically defined subsets. Ankylosing spondylitis (AS), also termed radiographic axial SpA, produces visible bone damage on plain radiographs through sacroiliitis and syndesmophyte formation [1]. Nonradiographic axial spondyloarthritis (nr-axSpA) presents identical inflammatory symptoms without radiographic evidence of structural changes, though MRI detects active inflammation [6]. These conditions occupy different regions on a disease spectrum rather than representing sequential stages, as many nr-axSpA patients never progress to AS [1]. Results from current studies indicate approximately half of all axial SpA patients have the nonradiographic form [6].
Peripheral spondyloarthritis includes distinct but related conditions. Psoriatic arthritis affects small joints in hands and feet, with 82% of patients presenting psoriasis at SpA onset [7]. Up to 70% of PsA patients demonstrate combined peripheral and spinal inflammation [1]. Enteropathic arthritis accompanies inflammatory bowel diseases like ulcerative colitis and Crohn’s disease, frequently affecting the spine while rarely causing joint destruction [1]. Reactive arthritis develops following intestinal or urinary tract infections, with symptoms typically subsiding within three to twelve months [8]. Undifferentiated spondyloarthritis applies when patients display SpA features without fitting specific subtype criteria [9].
Early Signs of SpA
Inflammatory back pain constitutes the primary manifestation across SpA subtypes. This pain develops gradually, persists beyond three months, and improves with physical activity rather than rest [8]. Morning stiffness lasting more than 30 minutes characterizes the condition [6]. The pain typically localizes deep in the lower back or buttocks, reflecting sacroiliac joint inflammation [8]. Initial symptoms manifest differently across SpA types. Back pain represents the first symptom in 72% of AS patients and 56% of undifferentiated SpA cases [7]. In contrast, lower limb arthritis appears first in 57% of psoriatic SpA patients and 35% of undifferentiated SpA patients [7].
Axial spondyloarthritis predominantly affects younger individuals, with average symptom onset at 28 years [6]. Most cases develop between ages 18 and 40 [10]. Males experience AS more frequently, while nr-axSpA affects both sexes equally [6]. Patients with axial SpA show earlier disease onset at 32 years compared to peripheral SpA patients at 38 years [1].
Enthesitis emerges as a distinguishing feature, affecting 28% of undifferentiated SpA patients at onset compared to under 13% in other groups [7]. Common sites include the heel (Achilles tendon), plantar fascia, and rib-sternum junctions [10]. Dactylitis, producing swollen “sausage digits,” appears in 10% of psoriatic SpA cases and 7% of undifferentiated SpA cases at disease onset [7].
Extra-articular manifestations frequently accompany SpA. Anterior uveitis affects 9% of AS patients and 7% of undifferentiated SpA patients [7]. Between 30% and 40% of all SpA patients develop eye inflammation [1]. Fatigue represents a common systemic symptom [10].
Peripheral vs Axial Involvement
Classification criteria specify that patients with current back pain plus peripheral manifestations receive axial SpA designation regardless of disease burden distribution [1]. This creates overlap, as 51% of patients classified as axial SpA also demonstrate peripheral arthritis, enthesitis, or dactylitis [1]. These combined presentations generate higher disease activity scores than pure axial or peripheral forms [1].
Peripheral manifestations dominated early presentations in specific subtypes. Arthritis constituted the initial symptom in 67% of early SpA patients, more frequently in lower limbs (38%) than upper limbs (29%) [7]. Upper limb arthritis appeared significantly more often in early AS (15%) compared to established disease (3%) [7]. Peripheral joint involvement affected 51% of psoriatic SpA patients versus only 20-21% of AS and undifferentiated SpA patients [7].
Genetic and demographic patterns differ between axial and peripheral forms. Patients with axial SpA demonstrate higher HLA-B27 prevalence and uveitis rates but lower frequencies of psoriasis and IBD compared to peripheral SpA [1]. The diagnostic delay remains substantial, averaging nine years from symptom onset to AS diagnosis [6].
Key Clinical Differences Between Seronegative RA and SpA 
Distinguishing clinical features separate seronegative RA from early spondyloarthritis, though overlapping manifestations complicate diagnosis. Joint inflammation, pain, and functional impairment occur in both conditions, yet specific patterns of involvement provide diagnostic clarity when systematically evaluated.
Joint Involvement Patterns
Anatomic distribution differs markedly between these conditions. RA primarily targets metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints of the hands, along with wrists, shoulders, elbows, knees, ankles, and metatarsophalangeal joints. Office extremity MRI reveals synovitis at MCP joints more frequently in RA patients compared to psoriatic arthritis [1]. In contrast, SpA affects distal interphalangeal (DIP) joints of hands and feet, with ultrasound findings of synovitis and erosions at these distal sites appearing exclusively in PsA versus RA [1]. Large joints of lower extremities receive more involvement in SpA, particularly knees and ankles in asymmetric patterns [11].
The underlying pathology diverges between conditions. Joint damage in RA comprises widespread destruction with minimal repair indications, whereas damage in AS typically accompanies remodeling and new bone formation [7][1]. Periosteal inflammation at the first interphalangeal joint appears exclusively among PsA patients rather than RA patients [1]. Registry analysis demonstrated similarities in swollen joint counts and tender joint counts between seronegative RA and SpA populations, though patients with SpA showed lower tender joint counts versus RA patients overall [1].
Inflammatory Back Pain in SpA
Inflammatory back pain serves as the hallmark manifestation distinguishing axial spondyloarthritis from RA. This chronic pain concentrates in the axial spine and sacroiliac joints, characterized by insidious onset before age 40, persistence beyond three months, and morning stiffness lasting 30 minutes or longer [12]. Unlike mechanical back pain, IBP improves with exercise rather than rest and often causes nocturnal awakening during the second half of the night [12][13]. Patients typically experience dull aches deep in the lower back or alternating buttock pain reflecting sacroiliac inflammation [12][13].
Diagnostic sensitivity reaches 70.3% and specificity 81.2% when back pain lasting three months combines with two of four clinical features: morning stiffness exceeding 30 minutes, improvement with exercise but not rest, alternating buttock pain, and awakening due to back pain during the night’s second half [13]. Only one study evaluated IBP as a primary focus, finding patients with axSpA demonstrated higher Bath Ankylosing Spondylitis Disease Activity Index and Functional Index scores than RA patients [7].
Enthesitis: A Distinguishing Feature
Inflammation at entheses, where tendons and ligaments insert into bone, theoretically distinguishes SpA from RA [12][14]. Common sites include Achilles tendon, plantar fascia, and patellar ligament insertions [11]. Enthesitis affects 35% of PsA patients but remains uncommon in RA [11]. However, ultrasonography studies challenge this distinction. Patients with SpA and RA demonstrated similar prevalence of painful enthesis at examined sites (17% versus 14%) [6][15]. At least one ultrasound enthesis abnormality appeared with comparable frequency (46% versus 48% of sites) [6][15]. Mean MASEI scores showed no difference between RA (8.5±7.3) and SpA patients (7.8±6.5) [6][15].
Given that the majority of comparative studies (14 of those reporting enthesitis) found higher prevalence in SpA versus RA cohorts [16], the conflicting ultrasonographic data suggests entheseal features may have low specificity in inflammatory joint conditions [6][15].
Dactylitis and Psoriasis in SpA
Dactylitis, producing fusiform swelling of entire digits, occurs exclusively in SpA populations. This “sausage digit” manifestation affects up to 50% of PsA patients compared to approximately 5% of RA patients [11]. Among early SpA patients, 9.5% currently or previously experienced dactylitis [7]. Dactylitis affected 48% of PsA patients at some point during disease course [7]. Toes receive more frequent involvement than fingers, with 66% of affected patients demonstrating pedal involvement only [7].
Psoriasis and nail psoriasis appear exclusively in SpA versus RA across all comparative studies [7][1][16]. Skin disease precedes joint symptoms in 84% of PsA patients, with up to 96% having current, previous, or family history of psoriasis [11].
Symmetry of Joint Symptoms
RA characteristically produces symmetrical polyarthritis affecting identical joints bilaterally [14][14]. This hallmark pattern aids diagnosis when metacarpophalangeal joints on both hands or knees bilaterally demonstrate simultaneous inflammation. Conversely, joint involvement in PsA remains typically asymmetric, though symmetry tends to increase as affected joint numbers rise [11]. SpA commonly presents as asymmetric oligoarthritis of lower extremities, particularly affecting knees [13][14].
Seronegative Rheumatoid Arthritis Diagnosis Methods
Diagnosing seronegative rheumatoid arthritis requires a multimodal approach combining laboratory evaluation, physical examination, and disease activity assessment. The absence of characteristic antibodies necessitates greater reliance on clinical judgment and imaging techniques compared to seropositive cases.
Laboratory Tests and Biomarkers
Serological testing forms the foundation of RA classification. RF positivity requires values ≥25 IU/mL, while ACPA positivity requires ≥10 IU/mL [17]. Patients testing negative for both antibodies fall into the seronegative category, representing the diagnostic challenge. However, RF demonstrates limited specificity, as 5% of healthy individuals test positive while 20% of confirmed RA patients remain RF-negative [18]. ACPA offers superior specificity at 97% for RA when present, though 20% of RA patients never develop these antibodies [18].
Inflammatory markers provide supportive but imperfect evidence. ESR normal ranges span 0-15 mm/hr to 0-20 mm/hr for men and 0-20 mm/hr to 0-30 mm/hr for women, with age-dependent variations [18]. CRP levels below 1.0 mg/L typically indicate absence of inflammation [18]. Registry data reveals that over half of RA patients maintain normal ESR and CRP despite ongoing disease activity determined by joint counts [12]. Correspondingly, 49.4% of patients with normal CRP (<5 mg/L) demonstrated histological inflammation on synovial biopsy [12].
Novel biomarkers address diagnostic gaps in seronegative disease. Anti-RA33 antibodies appear in 16% of seronegative RA patients, with IgG demonstrating 99% specificity versus healthy controls [13]. The 14-3-3η protein, elevated in 60-75% of RA patients with 78-93% specificity, shows particular value when combined with RF and ACPA testing to achieve sensitivity exceeding 80% for early RA [13]. Anti-carbamylated protein antibodies identify 16-30% of ACPA-negative patients and confer 2-3-fold increased risk of radiographic progression [13]. Calprotectin correlates strongly with disease activity (r = 0.5-0.7 with DAS28) and outperforms CRP in detecting subclinical synovitis [13]. Lipidomic profiling identified a panel of ten serum lipids differentiating RA from osteoarthritis with 79% accuracy, 71% sensitivity, and 86% specificity, regardless of seropositivity [13].
Physical Examination Findings
Clinical assessment focuses on symmetrical polyarticular involvement. Examiners document swelling, tenderness, and warmth in hands, wrists, knees, elbows, ankles, hips, and feet [19]. Joint counts include 44 swollen joints and tender joint assessments using the Ritchie Articular Index [17]. Metacarpophalangeal and proximal interphalangeal joint involvement supports RA diagnosis over SpA [6]. Morning stiffness persisting beyond 30 minutes indicates inflammatory rather than mechanical pathology [19].
Disease Activity Scores
The DAS28 incorporates joint counts, patient global assessment, and either ESR or CRP. DAS28-CRP consistently produces lower scores than DAS28-ESR, with mean differences of 0.54-0.57 points [15]. A DAS28-CRP cut-off of 4.6 corresponds to the validated DAS28-ESR threshold of 5.1 for high disease activity [15]. Alternative measures include CDAI and SDAI, which assess disease activity without laboratory components [20]. The multi-biomarker disease activity score measures 12 serum proteins, categorizing activity as low (<30), moderate (30-44), or high (>44) [13]. Notably, over 50% of patients classified in remission by DAS28 demonstrate persistent synovitis on ultrasound or MRI [12].
Imaging Techniques for Accurate Diagnosis 
Advanced imaging modalities overcome the diagnostic limitations inherent to seronegative rheumatoid arthritis diagnosis, where absent antibodies necessitate objective confirmation of inflammatory changes. Musculoskeletal ultrasound and MRI detect subclinical inflammation earlier than physical examination, facilitating timely differentiation between seronegative RA and spondyloarthritis.
Ultrasound Detection of Synovitis and Enthesitis
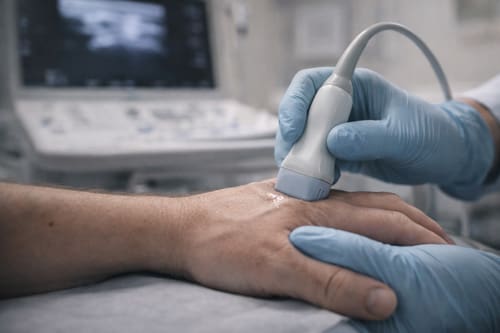
Musculoskeletal ultrasound facilitates diagnostic and therapeutic decisions in rheumatic diseases through real-time visualization, good patient tolerability, rapid multi-joint assessment, cost-effectiveness, and absence of ionizing radiation [21]. The modality accurately distinguishes inflammatory from non-inflammatory joint pain, with ultrasound-detected synovitis predicting RA development independent of antibody status [21]. In individuals with RA-related antibodies but no clinical synovitis, ultrasound-detected inflammation conferred a 3-fold risk of inflammatory arthritis development [21].
Power Doppler ultrasound demonstrates superior sensitivity for detecting enthesitis in spondyloarthropathy, achieving 76% sensitivity and 81% specificity in suspected SpA [7]. Cross-sectional studies reveal distinct ultrasonographic signatures differentiating early disease. Extensor enthesitis at distal interphalangeal joints, peritendon inflammation of finger extensor tendons, and tissue edema occur more frequently in early psoriatic arthritis, whereas extensor carpi ulnaris tenosynovitis predominates in RA [21].
High-resolution musculoskeletal ultrasound reveals inflammatory changes in 85% of clinically affected joints and 20% of apparently healthy joints [22]. Flexor tenosynovitis affects approximately one-third of PsA patients, while RA patients demonstrate extensor tendon involvement in 63% of cases [22]. Correspondingly, musculoskeletal ultrasound captures the inflammatory and erosive phenotype of seronegative RA with power Doppler signal correlating with DAS28 only in seronegative disease [23]. Advanced imaging techniques allowed more accurate distinction between SpA and RA in 70 of 79 publications [24][25].
MRI for Early Inflammation
MRI revolutionized axial spondyloarthritis detection through superior sensitivity for inflammatory changes. The modality achieved 90% sensitivity and specificity for SpA diagnosis, rising to 97.2% sensitivity and 94.2% specificity when sacroiliitis combines with clinical features in young adults with chronic back pain [14]. Fat-suppressed T2-weighted or STIR images optimally visualize active inflammatory lesions without requiring gadolinium contrast [7][14].
Bone marrow edema on STIR sequences indicates active sacroiliitis, with diagnostic criteria requiring one lesion on two consecutive slices or multiple lesions on one slice [11][14]. The presence of both bone marrow edema and erosions achieved 94% specificity and 75% sensitivity for sacroiliitis diagnosis [14]. MRI detected active sacroiliitis in 39.5% of patients without radiographic changes while ruling out active lesions in 60.4% of cases with radiographic sacroiliitis [11].
Structural lesions including erosions, subchondral fat replacement, backfill, and ankylosis distinguish SpA from mimics [26]. MRI spatial analysis demonstrated seronegative RA patients exhibit preferential scaphoid and lunate erosions, whereas seropositive patients show capitate and hamate involvement [23]. Novel sequences including volumetric interpolated breath-hold examination and synthetic CT create radiodensity maps without ionizing radiation [26].
X-ray Findings: Erosions vs New Bone Formation
Conventional radiography remains the primary clinical modality for established SpA, though sensitivity reaches only 19% for detecting active sacroiliitis [11]. Radiographic sacroiliitis varies with disease stage, progressing from joint widening and erosion in early disease to sclerosis and fusion in late disease [1]. Syndesmophytes predict development of new syndesmophytes in ankylosing spondylitis, though radiographic damage shows poor sensitivity to change [7][26].
Joint destruction in RA demonstrates widespread damage with minimal repair, contrasting with AS where damage accompanies remodeling and new bone formation [1]. Low-dose CT detects erosions with equivalent radiation exposure to radiography while providing superior sensitivity [26].
When to Use Advanced Imaging
When peripheral SpA is suspected, ultrasound or MRI detects peripheral enthesitis, arthritis, tenosynovitis, and bursitis supporting diagnosis [7]. MRI of sacroiliac joints and spine assesses disease activity in axial SpA, with STIR sequences sufficient for inflammation detection [7]. Dual-energy CT differentiates calcium from hydrogen, enabling bone marrow edema visualization in patients contraindicated for MRI [26].
Common Misdiagnosis Scenarios
Classification of seronegative arthritides poses substantial challenges in clinical practice. Misclassification delays appropriate SpA diagnosis and leads to suboptimal therapeutic outcomes [16]. The overlap between seronegative RA and spondyloarthritis manifestations creates diagnostic uncertainty that evolves over extended follow-up periods.
Why Seronegative RA Gets Confused with SpA
The absence of reliable serologic testing forces clinicians to rely on pattern recognition and clinical judgment [27]. This dependence introduces cognitive biases including availability heuristics, framing effects, and anchoring that influence decision making toward premature diagnostic closure [27]. Chronic synovitis represents a nonspecific feature appearing across numerous diseases including connective tissue diseases, crystal arthropathies, infection-related inflammatory polyarthritis, and spondyloarthropathy [28].
Seronegative RA and SpA share overlapping clinical characteristics including joint inflammation, pain, diminished functional ability, and disability [16]. Due to these similarities, clinical disease misclassification could occur despite differences in SpA manifestation prevalence [16]. Chronic back pain from ankylosing spondylitis may be mistaken for mechanical pain, while psoriatic arthritis gets confused with osteoarthritis when skin lesions remain inconspicuous [6]. Seronegative RA may fundamentally represent a different condition that behaves more like spondyloarthritis than classic RA [6].
Diagnosis Changes Over Time
Long-term follow-up reveals substantial diagnostic heterogeneity. Among patients initially diagnosed with seronegative arthritis, 24% eventually received SpA diagnoses including PsA, peripheral SpA, nr-axSpA, AS, IBD, and reactive arthritis [18]. By 10 years, 12.8% of seronegative RA patients experienced diagnosis changes, most commonly to spondyloarthritis with a cumulative incidence rate of 4.0% [29]. Another cohort demonstrated 15.1% ten-year cumulative incidence of diagnostic revision [30].
Correspondingly, in one analysis of nearly 10,000 seronegative RA patients, more than 500 actually had spondyloarthritis, 275 had psoriatic arthritis, and 245 had axial spondyloarthritis [5]. One study with 23-year follow-up found that over 60% of patients initially classified as seronegative RA turned out to have SpA [17]. Evidently, 70% of rheumatologists reported observing diagnosis changes from seronegative RA to other diseases during follow-up [28].
Risk Factors for Misclassification
Male patients and those diagnosed with seronegative RA before age 50 appear more prone to diagnostic changes toward SpA over time [18]. By comparison, older age associates with reduced risk for diagnosis revision, though this relationship reached only borderline statistical significance [29].
Differential Diagnosis of Rheumatoid Arthritis vs SpA
Step-by-Step Diagnostic Approach
The diagnostic approach aims to estimate disease probability rather than apply classification criteria, which require established diagnosis beforehand [13]. For that reason, clinicians must systematically exclude other explanations for back pain including degenerative disorders, infection, and tumors before diagnosing axial SpA [13]. Inflammatory back pain presence serves as an initial screening step for preselecting high-probability axial SpA patients among those with chronic back pain, though IBP alone remains insufficient for diagnosis [13]. Good response to NSAIDs frequently accompanies IBP and increases the probability of true inflammatory disease [13].
Diagnostic certainty increases with accumulated clinical features rather than single findings. In typical chronic low back pain populations presenting to primary care, meeting IBP criteria increases AS or axial SpA probability by a factor of 3, rising from less than 5% at baseline to only 14% [19]. Essentially, three or more red flags elevate diagnostic probability to the comfort zone exceeding 90% [19]. Physical examination should include checking for sacroiliac joint tenderness through stress maneuvers, assessing spinal mobility and chest expansion, and identifying enthesitis at vertebral spinal processes, iliac crest, anterior chest wall, calcaneus, ischial tuberosities, and greater trochanters [19]. Women tend to have milder or slower disease courses with neck and thoracic pain resembling fibromyalgia or early RA [19].
Red Flags That Point to SpA
Back pain onset before age 45 lasting more than three months warrants SpA evaluation [31]. An index combining chronic inflammatory back pain, thoracic spine pain, and anterior chest wall pain demonstrated 83.1% sensitivity and 87.2% specificity for axial SpA [19]. Acute anterior uveitis occurred more commonly in first-degree relatives with axSpA (38.2%) than those without (11.6%), suggesting AAU serves as a useful screening indicator [19]. Patients with initial normal sacroiliac MRI may require symptomatic management and regular follow-up with wait-and-see attitudes [19].
When to Refer to a Rheumatologist
Prompt rheumatology referral becomes critical when inflammatory low back pain is recognized [32]. Studies indicate 5 to 6-year delays between symptom onset and diagnosis [32]. Chronic lower back pain lasting greater than 3 months with onset before age 45 should raise autoimmune disorder suspicion [32].
Extra-Articular Manifestations to Consider
Acute anterior uveitis represents the most common extra-musculoskeletal manifestation, occurring in approximately 20% of SpA patients [13]. Psoriasis appears in about 10% of SpA patients, while clinically manifest IBD affects 2% to 7% [13]. Family history carries weight, as SpA presence in first or second-degree relatives associates with increased disease risk [13].
Treatment Implications of Getting the Diagnosis Right 
Therapeutic outcomes diverge substantially between seronegative RA and spondyloarthritis, making accurate differential diagnosis of rheumatoid arthritis essential for optimal management. Treatment initiation within three months of symptom onset more than doubles the likelihood of DMARD response in seronegative RA, with an odds ratio of 2.41 [33]. In contrast, very early seronegative RA presents with minor disease activity and requires less aggressive therapy, including fewer biologic agents and corticosteroids compared to seropositive disease [34].
First-Line Treatments for Each Condition
Methotrexate constitutes first-line therapy for RA regardless of serologic status, though evidence demonstrates reduced efficacy in seronegative disease [17]. Specifically, MTX shows inferior effectiveness in improving biologic drug retention rates among seronegative patients [17]. NSAIDs serve as initial pharmacologic therapy for SpA, with maximal dosing required before advancing to biologics [35]. Non-biologic DMARDs like methotrexate and sulfasalazine remain ineffective in axial disease but provide second-line treatment for peripheral SpA [35].
Response to TNF Inhibitors
Anti-TNF molecule survival extends longer in SpA patients than RA patients [36]. When initial TNFi fails due to inefficacy in RA, switching to non-TNF biologics produces more substantial disease activity improvement than trying a second TNFi [36]. Conversely, when discontinued because of drug intolerance, switching to either rituximab or another TNFi shows similar effectiveness [36]. Seronegative RA generally responds positively to switching to a second anti-TNF after first-agent failure, often not requiring different cytokine-targeted therapies [17].
Why Other Biologics Work Differently
Drugs targeting B or T cells, such as anti-CD20 or anti-CD80/CD86 biologics, demonstrate low efficacy in seronegative RA compared to seropositive patients [17]. This supports the hypothesis that adaptive immunity plays a lesser role in seronegative disease [17]. For SpA, IL-17 inhibitors including secukinumab and ixekizumab provide effective alternatives when TNF inhibitors prove intolerable [35].
Long-Term Management Strategies
Seronegative RA demonstrates more favorable long-term radiographic outcomes than seropositive disease [17]. Drug-free remission proves achievable in 27% of seronegative RA patients within 10 years [15].
Conclusion 

Distinguishing seronegative rheumatoid arthritis from early spondyloarthritis remains diagnostically challenging, yet getting it right matters considerably. With this in mind, 8.8% of patients initially diagnosed with seronegative RA eventually receive revised SpA diagnoses, underscoring the need for systematic evaluation. Pattern recognition holds the key. Symmetrical small joint involvement, morning stiffness, and MCP synovitis point toward seronegative RA. Inflammatory back pain, enthesitis, dactylitis, and psoriasis indicate spondyloarthritis. Treatment responses diverge substantially between these conditions. Methotrexate serves seronegative RA patients adequately, while NSAIDs and TNF inhibitors constitute first-line SpA therapy. Regular reassessment proves essential, as diagnoses evolve over time. Clinicians who recognize red flags early and refer appropriately optimize patient outcomes through condition-specific management strategies.
Frequently Asked Questions: 
FAQs
Q1. Are spondyloarthritis and seronegative arthritis the same condition? While these terms are sometimes used interchangeably, they describe related but distinct conditions. Spondyloarthritis is a family of inflammatory diseases that can affect the spine and peripheral joints, and all types test negative for rheumatoid factor, which is why they’re also called seronegative arthritis. However, not all seronegative arthritis is spondyloarthritis—seronegative rheumatoid arthritis is a separate condition that lacks these antibodies but has different clinical features.
Q2. What are the main differences in joint involvement between RA and spondyloarthritis? Rheumatoid arthritis typically affects small peripheral joints symmetrically, particularly the hands and feet, and rarely involves the spine. Spondyloarthritis primarily targets the spine and sacroiliac joints, with less frequent involvement of peripheral joints. When peripheral joints are affected in spondyloarthritis, the pattern is usually asymmetric and may include the distal finger joints, which RA typically spares.
Q3. How do doctors diagnose seronegative rheumatoid arthritis without antibody markers? Diagnosis relies on clinical presentation including persistent joint pain, swelling, and morning stiffness lasting more than 30 minutes. Doctors look for symmetrical polyarthritis affecting multiple joints, elevated inflammatory markers like ESR and CRP, and characteristic findings on imaging such as X-rays showing erosions or ultrasound detecting synovitis. The combination of these features helps establish the diagnosis even without positive antibody tests.
Q4. What distinguishes seronegative RA from seropositive RA? The primary difference is the absence of rheumatoid factor and anti-CCP antibodies in blood tests. Despite this serological difference, both forms can present with similar symptoms including joint pain, swelling, and stiffness. However, seronegative RA patients tend to have later disease onset, fewer rheumatoid nodules, and may show less severe inflammation on imaging compared to seropositive patients.
Q5. Why does inflammatory back pain suggest spondyloarthritis rather than RA? Inflammatory back pain is a hallmark of spondyloarthritis and rarely occurs in rheumatoid arthritis. This type of pain develops gradually before age 40, improves with exercise rather than rest, causes morning stiffness lasting over 30 minutes, and often wakes patients during the second half of the night. The pain typically affects the lower back and buttocks due to sacroiliac joint inflammation, which is characteristic of spondyloarthritis but not RA.
References: 
[2] – https://www.webmd.com/rheumatoid-arthritis/seronegative-for-rheumatoid-arthritis
[3] – https://ucfhealth.com/our-services/rheumatology/seronegative-rheumatoid-arthritis/
[4] – https://lucidaclinical.com/blogs/what-is-seronegative-rheumatoid-arthritis/
[5] – https://www.arthritis.org/diseases/more-about/what-type-of-ra-do-you-have
[6] – https://arthritissj.com/why-seronegative-rheumatic-diseases-are-difficult-to-diagnose/
[7] – https://ard.bmj.com/content/74/7/1327
[8] – https://spondylitis.org/about-spondylitis/overview-of-spondyloarthritis/
[9] – https://my.clevelandclinic.org/health/diseases/spondyloarthritis-spondyloarthropathy
[10] – https://www.nhs.uk/conditions/ankylosing-spondylitis/symptoms/
[11] – https://jbsr.be/articles/10.5334/jbr-btr.1393
[12] – https://www.frontiersin.org/journals/medicine/articles/10.3389/
fmed.2018.00185/full
[13] – https://pmc.ncbi.nlm.nih.gov/articles/PMC7566535/
[14] – https://ajronline.org/doi/10.2214/AJR.12.8858
[15] – https://www.droracle.ai/articles/687804/what-is-the-initial-treatment-approach-for-a-patient
[16] – https://ard.bmj.com/content/79/Suppl_1/1141
[17] – https://pmc.ncbi.nlm.nih.gov/articles/PMC10660552/
[18] – https://pmc.ncbi.nlm.nih.gov/articles/PMC8121445/
[19] – https://www.healio.com/clinical-guidance/ankylosing-spondylitis/early-diagnosis-presentation-and-diagnosis
[20] – https://pmc.ncbi.nlm.nih.gov/articles/PMC9424641/
[21] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12546444/
[22] – https://esmed.org/musculoskeletal-ultrasound-in-diagnosing-arthritis-types/
[23] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12821548/
[24] – https://pmc.ncbi.nlm.nih.gov/articles/PMC8964901/
[25] – https://link.springer.com/article/10.1007/s40744-021-00407-8
[26] – https://www.jrheum.org/content/51/12/1241
[27] – https://www.rheumatologyadvisor.com/features/diagnosing-seronegative-rheumatic-diseases/
[28] – https://journals.lww.com/cmii/fulltext/2021/19040/classification_
criteria_for_seronegative.4.aspx
[29] – https://www.medscape.com/viewarticle/seronegative-ra-diagnostic-changes-outcomes-over-10-years-2026a10002tx
[30] – https://acrabstracts.org/abstract/long-term-outcomes-in-seronegative-rheumatoid-arthritis/
[31] – https://spondylitis.org/about-spondylitis/could-i-have-spondyloarthritis/
[32] – https://now.aapmr.org/seronegative-spondyloarthropathy/
[33] – https://www.medpagetoday.com/rheumatology/arthritis/83435
[34] – https://ard.bmj.com/content/78/Suppl_2/1616.2
[35] – https://www.ncbi.nlm.nih.gov/books/NBK459356/
[36] – https://www.rheumatologyadvisor.com/features/comparing-tumor-necrosis-factor-inhibitors-for-ra-and-spa-overview-expert-interview/
Video Section
Check out our extensive video library (see channel for our latest videos)
Recent Articles


