Hypotension Prediction Index and Machine Learning Game Changer or Gimmick
Abstract
Intraoperative and critical care hypotension is independently associated with adverse outcomes, including acute kidney injury, myocardial injury, stroke, prolonged hospitalization, and increased mortality. Even brief episodes of mean arterial pressure below established thresholds have been linked to clinically notable organ dysfunction. Traditional monitoring approaches rely on reactive detection of blood pressure decline after it has occurred, prompting therapeutic interventions such as fluid administration, vasopressors, or anesthetic adjustment. This reactive paradigm has driven interest in predictive monitoring tools that can anticipate hemodynamic instability before clinically significant hypotension develops.
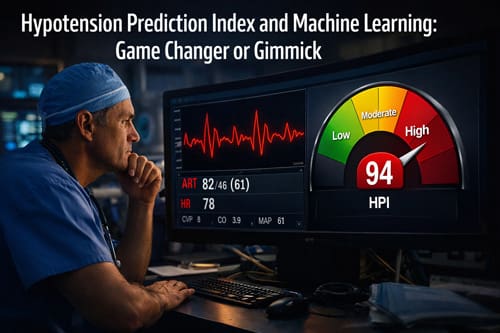
The Hypotension Prediction Index (HPI) represents a data driven approach to this challenge. Developed using machine learning algorithms applied to high fidelity arterial waveform data, HPI generates a unitless index that reflects the likelihood of impending hypotension within a defined time horizon. By analyzing subtle changes in arterial pressure waveform characteristics that may precede overt blood pressure decline, the system aims to provide clinicians with actionable early warning signals. When integrated into advanced hemodynamic monitoring platforms, HPI can be combined with secondary parameters such as stroke volume variation, dynamic arterial elastance, and cardiac output to guide targeted interventions.
Recent clinical studies have demonstrated that HPI guided management may reduce the duration and severity of intraoperative hypotension in selected surgical populations. Randomized and observational investigations suggest that predictive monitoring can decrease cumulative hypotensive time and lower the incidence of sustained hypotensive episodes. These findings are particularly relevant in high risk surgical patients, including those undergoing major abdominal, vascular, or cardiac procedures, where hemodynamic instability is common and associated with poor outcomes.
However, the translation of predictive indices into meaningful patient centered benefits remains an area of ongoing evaluation. While reductions in hypotension duration are promising, robust evidence demonstrating consistent improvement in hard clinical endpoints such as mortality, organ dysfunction, or long term recovery remains limited. Furthermore, algorithm performance may vary across patient populations, anesthetic techniques, and clinical environments. Factors such as arrhythmias, spontaneous ventilation, peripheral vascular disease, and variations in arterial line quality can influence waveform fidelity and predictive accuracy.
Implementation challenges must also be carefully considered. Integration of HPI into clinical workflows requires training, familiarity with algorithm outputs, and the ability to interpret predictive alerts within the broader clinical context. Overreliance on automated indices without comprehensive physiologic assessment may increase the risk of inappropriate or premature intervention. In addition, predictive systems may generate false positive alerts, potentially contributing to alarm fatigue and unnecessary administration of fluids or vasopressors. Excessive or poorly targeted interventions carry their own risks, including fluid overload, vasoconstriction related tissue hypoperfusion, and increased resource utilization.
Cost effectiveness is another important consideration. Advanced monitoring platforms incorporating HPI technology require specialized equipment and disposable sensors, which may not be feasible in all healthcare settings. Institutions must evaluate whether reductions in intraoperative hypotension justify the associated financial investment, particularly in resource constrained environments. Comparative effectiveness research and health economic analyses are needed to determine which patient populations derive the greatest benefit from predictive monitoring strategies.
In summary, the Hypotension Prediction Index represents an innovative application of machine learning to hemodynamic management in perioperative and critical care medicine. Early data suggest that HPI guided monitoring can reduce the burden of intraoperative hypotension in selected populations. However, broader adoption should be guided by further validation in diverse patient groups, clearer evidence of improvement in clinically meaningful outcomes, and careful assessment of implementation logistics and cost. As predictive analytics continue to evolve, HPI technology highlights both the promise and the practical challenges of integrating artificial intelligence driven tools into routine clinical practice.
Introduction
Hypotension remains one of the most frequently encountered hemodynamic disturbances in perioperative and critical care settings. Episodes of low arterial blood pressure occur commonly during major surgery, anesthesia induction, and in critically ill patients with sepsis, trauma, or cardiovascular instability. Conventional blood pressure monitoring methods rely on either intermittent noninvasive cuff measurements or continuous invasive arterial catheter monitoring. While arterial lines provide real time waveform data, clinical responses to hypotension are typically reactive. Interventions are initiated only after blood pressure has already fallen below a defined threshold. This reactive model may permit periods of tissue hypoperfusion that contribute to organ dysfunction before corrective action is taken.
The development of the Hypotension Prediction Index represents an effort to transition from reactive management toward proactive hemodynamic optimization. The HPI system, developed by Edwards Lifesciences and incorporated into advanced hemodynamic monitoring platforms, applies machine learning algorithms trained on large datasets of arterial waveform recordings. By analyzing subtle morphological features within the arterial pressure waveform in real time, the algorithm generates a dynamic index ranging from 0 to 100. Higher index values indicate an increased probability that hypotension, typically defined as a mean arterial pressure below a specified threshold, will occur within the next several minutes. This predictive capability is intended to provide clinicians with an early warning signal, allowing targeted interventions such as fluid administration, vasopressor initiation, or adjustment of anesthetic depth before a clinically significant drop in blood pressure occurs.
The clinical rationale for preventing hypotension is well established. Intraoperative hypotension has been consistently associated with adverse postoperative outcomes, including myocardial injury after noncardiac surgery, ischemic stroke, acute kidney injury, and increased short term and long term mortality. Emerging evidence suggests that even brief episodes of mean arterial pressure below critical thresholds may independently increase the risk of organ dysfunction. These findings have shifted the paradigm from tolerating transient hypotension to emphasizing tight hemodynamic control throughout the perioperative period. In this context, a monitoring tool capable of forecasting hypotensive events has considerable theoretical appeal.
Early validation studies of the HPI algorithm have demonstrated promising predictive performance under controlled conditions. Reported metrics include high sensitivity and specificity for impending hypotension when predefined index thresholds are used. Additionally, some clinical investigations suggest that HPI guided management may reduce the duration and severity of intraoperative hypotension. However, these findings must be interpreted within the broader framework of implementation science and real world clinical practice. Algorithm performance can vary depending on patient population, surgical context, and clinician response to alerts. Furthermore, the predictive index does not independently correct hemodynamic instability. Its effectiveness depends on timely and appropriate therapeutic action based on the information provided.
The introduction of novel monitoring technologies into routine practice warrants careful scrutiny. The history of perioperative innovation includes numerous devices that demonstrated strong physiological rationale and favorable surrogate endpoints yet failed to produce meaningful improvements in patient centered outcomes when tested in large randomized trials. Adoption of new technology also carries economic implications, including acquisition costs, training requirements, workflow adjustments, and potential alert fatigue. Healthcare systems must therefore evaluate not only predictive accuracy but also cost effectiveness, impact on clinician decision making, and measurable improvements in morbidity and mortality.
The central question for anesthesiologists, intensivists, and perioperative teams is whether the Hypotension Prediction Index represents a transformative advance in hemodynamic management or an incremental enhancement without substantial clinical impact. Addressing this question requires robust multicenter randomized controlled trials powered for patient centered outcomes, standardized intervention protocols in response to alerts, and transparent reporting of both benefits and limitations. As predictive analytics and machine learning become increasingly integrated into bedside monitoring, the evaluation of technologies such as HPI will shape the broader trajectory of precision hemodynamic care.
Understanding Hypotension Prediction Index Technology
The Hypotension Prediction Index operates on the principle that subtle changes in arterial waveform morphology precede clinically apparent hypotension. The technology uses machine learning algorithms trained on large datasets of arterial pressure waveforms collected from patients who experienced hypotensive episodes. By analyzing features such as waveform shape, variability, and derived hemodynamic parameters, the algorithm identifies patterns that typically precede hypotension.
The HPI algorithm processes multiple waveform characteristics simultaneously, including pulse pressure variation, systolic pressure variation, and other derived parameters that may not be readily apparent to human observers. The machine learning model was developed using data from over 25,000 patients and more than 540,000 minutes of arterial waveform data, representing one of the largest datasets used for hemodynamic prediction algorithm development.
The system outputs a continuous HPI value that updates every 20 seconds, providing clinicians with real-time assessment of hypotension risk. When the HPI value exceeds a predetermined threshold, typically set at 85, the system alerts clinicians to the increased risk of hypotension occurring within the next 5 to 15 minutes. This time window theoretically allows for preventive interventions such as fluid administration, vasopressor therapy, or anesthetic adjustments.
The technology is currently integrated into several Edwards Lifesciences monitoring platforms, including the EV1000 and HemoSphere systems. Implementation requires an existing arterial line for pressure monitoring, as the algorithm depends on high-fidelity arterial waveform analysis. The system cannot function with non-invasive blood pressure monitoring or low-quality arterial signals, which limits its applicability in certain clinical scenarios.
One of the key technical challenges addressed by the HPI algorithm is the need to account for individual patient variability and clinical context. The machine learning model incorporates patient-specific calibration and adapts to changing clinical conditions throughout the monitoring period. However, the algorithm’s performance may be affected by factors such as arrhythmias, mechanical ventilation settings, and pharmacologic interventions that alter cardiovascular physiology.
Clinical Evidence and Performance 
The clinical validation of HPI technology has been the subject of several studies since its commercial introduction. The initial validation studies demonstrated that the HPI could predict hypotensive episodes with sensitivity ranging from 76% to 89% and specificity between 87% and 96%, depending on the patient population and definition of hypotension used. These performance metrics suggest that the technology can identify most patients who will develop hypotension while maintaining a relatively low false positive rate.
The landmark study by Maheshwari et al. published in Anesthesiology in 2020 provided some of the first robust clinical evidence for HPI effectiveness. This randomized controlled trial involving 404 patients undergoing non-cardiac surgery found that HPI-guided hemodynamic management reduced the duration and severity of intraoperative hypotension compared to standard care. Patients in the HPI group experienced 23% less time with mean arterial pressure below 65 mmHg and had fewer severe hypotensive episodes.
Subsequent studies have expanded the evidence base for HPI technology across different patient populations and clinical settings. A study by Wijnberge et al. in 2021 evaluated HPI performance in cardiac surgery patients and found similar prediction accuracy, with the added benefit of reduced postoperative complications in patients managed with HPI guidance. The study reported lower rates of acute kidney injury and shorter intensive care unit stays in the HPI-guided group.
However, not all studies have demonstrated clear clinical benefits from HPI implementation. A multi-center trial by Davies et al. in 2022 failed to show major differences in major adverse outcomes between HPI-guided and conventional hemodynamic management in high-risk surgical patients. This study raised important questions about the clinical significance of preventing brief hypotensive episodes and whether the interventions prompted by HPI alerts actually improve meaningful patient outcomes.
The performance of HPI technology appears to vary based on patient characteristics and clinical context. Studies have shown reduced accuracy in patients with cardiovascular disease, those receiving mechanical circulatory support, and during procedures involving major fluid shifts or blood loss. Additionally, the algorithm’s performance may be compromised in patients with arrhythmias or those receiving certain medications that affect cardiovascular physiology.
Recent meta-analyses have attempted to synthesize the available evidence on HPI effectiveness. A systematic review by Thompson et al. in 2023 analyzed data from 12 studies involving over 3,000 patients and concluded that HPI-guided management reduces the incidence and duration of hypotensive episodes but does not consistently improve major clinical outcomes such as mortality or organ dysfunction. The authors noted heterogeneity in study designs and outcome measures, making definitive conclusions about clinical benefit challenging.
Applications and Clinical Use Cases
The primary application of HPI technology is in perioperative hemodynamic monitoring, particularly during procedures associated with high risk of hypotension. Cardiac surgery, major abdominal procedures, and operations in elderly or high-risk patients represent the most common use cases where HPI monitoring has been implemented. In these settings, the technology serves as an adjunct to existing hemodynamic monitoring rather than a replacement for clinical judgment.
Cardiac surgery represents one of the most promising applications for HPI technology. These procedures often involve hemodynamic instability due to cardiopulmonary bypass, myocardial stunning, and complex fluid management requirements. The ability to predict hypotensive episodes before they become clinically apparent allows anesthesiologists and perfusionists to make proactive adjustments to maintain hemodynamic stability. Several cardiac surgery centers have reported positive experiences with HPI implementation, noting improved hemodynamic management and potentially reduced complications.
Major non-cardiac surgery, particularly procedures involving elderly patients or those with multiple comorbidities, represents another important application area. These patients often have limited cardiovascular reserve and may develop hypotension in response to anesthetic agents, fluid shifts, or surgical stress. HPI monitoring can provide early warning of hemodynamic compromise, allowing for timely interventions to maintain organ perfusion pressure.
Critical care medicine has emerged as a potential growth area for HPI technology, although evidence in this setting remains limited. Critically ill patients often experience hemodynamic instability due to sepsis, heart failure, or other conditions that affect cardiovascular function. The ability to predict hypotensive episodes could theoretically improve outcomes by allowing for earlier intervention with fluids, vasopressors, or other supportive measures.
However, the implementation of HPI technology in critical care settings faces several challenges. Many critically ill patients have conditions that may affect the accuracy of HPI predictions, such as arrhythmias, mechanical circulatory support, or severe cardiovascular dysfunction. Additionally, the clinical significance of brief hypotensive episodes may be different in critically ill patients compared to surgical patients, potentially affecting the risk-benefit calculation for HPI-guided interventions.
Obstetric anesthesia represents another potential application for HPI technology, particularly during cesarean sections where maternal hypotension can affect both maternal and fetal well-being. Some studies have evaluated HPI use in this population, with mixed results regarding its effectiveness in preventing hypotension-related complications. The unique physiologic changes of pregnancy and the need to consider fetal effects of interventions add complexity to HPI implementation in obstetric patients.
Comparison with Traditional Monitoring Methods 
Traditional hemodynamic monitoring relies primarily on intermittent blood pressure measurements using automated cuffs or continuous monitoring via arterial catheters. These methods provide real-time information about current hemodynamic status but offer limited predictive capability. Clinicians typically respond to hypotensive episodes after they have already occurred, potentially missing opportunities for preventive intervention.
Non-invasive blood pressure monitoring using automated cuffs remains the standard of care in many clinical settings due to its simplicity, low cost, and minimal risk. However, intermittent measurements may miss brief hypotensive episodes and provide no warning of impending hemodynamic compromise. The typical measurement interval of 3-5 minutes means that hypotensive episodes can occur and resolve between measurements, potentially leading to unrecognized organ hypoperfusion.
Continuous arterial pressure monitoring via arterial catheters provides real-time hemodynamic information and allows for immediate recognition of blood pressure changes. This method enables rapid response to hypotensive episodes and provides additional information through waveform analysis. However, like non-invasive monitoring, arterial pressure monitoring is inherently reactive rather than predictive. Clinicians must wait for hypotension to develop before initiating treatment, potentially missing opportunities for prevention.
The HPI technology builds upon continuous arterial monitoring by adding predictive capability to existing hemodynamic assessment. Rather than replacing traditional monitoring methods, HPI serves as an enhancement that provides early warning of impending hypotensive episodes. This predictive approach theoretically allows for proactive rather than reactive hemodynamic management, potentially improving patient outcomes through prevention rather than treatment of hypotension.
Advanced hemodynamic monitoring systems that measure cardiac output, stroke volume variation, and other derived parameters provide additional information beyond simple blood pressure monitoring. These systems can help guide fluid and vasopressor therapy but still operate primarily in a reactive mode. The integration of HPI technology with advanced hemodynamic monitoring creates a more complete picture of cardiovascular status and risk, potentially improving clinical decision-making.
However, the added complexity and cost of HPI monitoring must be weighed against its clinical benefits. Traditional monitoring methods have proven safety records and established roles in clinical care, while HPI technology is still establishing its place in routine practice. The question facing healthcare providers is whether the predictive capability of HPI justifies the additional cost and complexity compared to proven monitoring methods.
Machine Learning Integration and Algorithm Performance
The integration of machine learning into HPI technology represents one of its most innovative aspects and potential advantages. The algorithm continuously learns from incoming waveform data and adapts to individual patient characteristics, theoretically improving prediction accuracy over time. This adaptive capability distinguishes HPI from static monitoring parameters and allows for personalized hemodynamic assessment.
The machine learning model underlying HPI technology uses supervised learning techniques trained on labeled datasets of arterial waveforms associated with known hypotensive episodes. The algorithm identifies complex patterns and relationships in waveform characteristics that may not be apparent to human observers. This approach allows the system to detect subtle changes in cardiovascular physiology that precede clinically apparent hypotension.
Feature extraction and selection represent critical components of the HPI algorithm’s performance. The system analyzes multiple waveform characteristics simultaneously, including traditional parameters like systolic and diastolic pressure as well as derived measures such as pulse pressure variation and waveform morphology descriptors. The machine learning model weights these features based on their predictive value and combines them into a single index score.
The performance of machine learning algorithms depends heavily on the quality and representativeness of training data. The HPI algorithm was developed using data from diverse patient populations and clinical settings, but questions remain about its generalizability to populations not well represented in the training dataset. Patients with rare cardiovascular conditions, extreme physiologic states, or unique demographic characteristics may not be adequately represented in the training data, potentially affecting algorithm performance.
Validation and ongoing monitoring of machine learning algorithms in healthcare represent critical challenges that affect HPI implementation. Unlike traditional medical devices with static performance characteristics, machine learning systems may exhibit different performance in real-world clinical settings compared to development environments. Continuous monitoring of algorithm performance and periodic revalidation may be necessary to ensure maintained accuracy over time.
The interpretability of machine learning predictions represents another important consideration for HPI technology. While the system provides a numerical index score, clinicians may have limited insight into the specific factors driving predictions. This “black box” nature of machine learning algorithms can create challenges for clinical decision-making and may affect physician acceptance and trust in the technology.
Challenges and Limitations
Despite its theoretical advantages, HPI technology faces several important challenges and limitations that affect its clinical implementation and effectiveness. Understanding these limitations is crucial for healthcare providers considering adoption of HPI monitoring systems and for appropriate clinical use of the technology.
Technical limitations represent one category of challenges facing HPI implementation. The technology requires high-quality arterial waveforms for optimal performance, which may not always be achievable in clinical practice. Factors such as arterial catheter dampening, air bubbles in the monitoring system, or poor catheter position can degrade signal quality and affect algorithm performance. Additionally, the system may not function optimally in patients with arrhythmias, mechanical circulatory support, or other conditions that alter normal cardiovascular physiology.
Patient-specific factors can also affect HPI accuracy and clinical utility. Studies have shown reduced algorithm performance in patients with severe cardiovascular disease, those receiving certain medications, and during specific clinical scenarios such as cardiopulmonary bypass or massive transfusion. The algorithm’s training data may not adequately represent all patient populations and clinical conditions encountered in routine practice, potentially limiting its generalizability.
Clinical workflow integration represents another challenge for HPI implementation. The technology adds additional monitoring parameters and alerts to already complex clinical environments, potentially contributing to alarm fatigue and information overload. Healthcare providers must develop protocols for responding to HPI alerts and integrate this information with other clinical data to make appropriate treatment decisions. The time required for staff training and protocol development represents an additional implementation cost.
The clinical significance of preventing brief hypotensive episodes remains a subject of ongoing debate and research. While studies have shown that HPI technology can reduce the incidence and duration of hypotensive episodes, the impact on meaningful clinical outcomes such as mortality, organ dysfunction, and long-term complications is less clear. Some critics argue that the interventions prompted by HPI alerts may cause more harm than the hypotensive episodes they prevent, particularly if they lead to excessive fluid administration or inappropriate vasopressor use.
Cost-effectiveness represents a major limitation for widespread HPI adoption. The technology requires expensive monitoring equipment and ongoing maintenance costs, while the clinical benefits may be modest in many patient populations. Healthcare systems operating under budget constraints must carefully evaluate whether the costs of HPI implementation are justified by demonstrated clinical benefits and improved patient outcomes.
False positive alerts represent a persistent challenge for HPI technology, as with many predictive monitoring systems. While the reported specificity of HPI algorithms is relatively high, false positive rates of 10-20% mean that clinicians will frequently receive alerts for patients who do not subsequently develop hypotension. These false alarms can lead to unnecessary interventions, increased healthcare costs, and potential patient harm from overtreatment.
Economic Considerations and Cost-Effectiveness 
The economic impact of HPI technology extends beyond the initial equipment costs to include ongoing operational expenses, staff training requirements, and potential savings from improved patient outcomes. Healthcare administrators and clinicians must carefully evaluate the total cost of ownership and expected return on investment when considering HPI implementation.
Direct costs associated with HPI technology include the monitoring equipment, software licenses, and disposable sensors or components required for operation. These costs can be substantial, particularly for healthcare systems seeking to implement HPI monitoring across multiple clinical areas. The specialized nature of the equipment may also limit vendor options and negotiating power, potentially increasing procurement costs.
Indirect costs include staff training, protocol development, and workflow modification required for successful HPI implementation. Healthcare providers must invest time and resources in educating clinical staff about the technology, developing response protocols for HPI alerts, and modifying existing clinical workflows to incorporate the new monitoring capabilities. These implementation costs can exceed the direct equipment costs in some cases.
The potential economic benefits of HPI technology depend primarily on its ability to prevent complications and reduce healthcare resource utilization. If HPI-guided management can reduce the incidence of hypotension-related complications such as acute kidney injury, myocardial infarction, or stroke, the resulting cost savings could offset the technology investment. However, demonstrating these benefits requires robust clinical evidence and long-term follow-up data.
Several economic analyses have attempted to evaluate the cost-effectiveness of HPI technology with mixed results. A study by Martinez et al. in 2022 suggested that HPI implementation could be cost-effective in high-risk surgical populations due to reduced complications and shorter hospital stays. However, other analyses have questioned whether the modest clinical benefits demonstrated in most studies justify the substantial costs of implementation.
The economic value proposition for HPI technology may vary based on patient population, clinical setting, and healthcare system characteristics. High-volume centers performing complex surgical procedures may achieve better cost-effectiveness compared to smaller facilities with lower-risk patient populations. Additionally, healthcare systems with existing advanced monitoring capabilities may face lower incremental costs for HPI implementation.
Value-based healthcare models that link reimbursement to patient outcomes may favor technologies like HPI that can demonstrate improvements in quality metrics. However, current reimbursement structures typically do not provide additional payment for HPI monitoring, requiring healthcare systems to absorb the costs while hoping for downstream savings from improved outcomes.
Future Directions and Research Needs
The future development and adoption of HPI technology will depend largely on addressing current limitations and expanding the evidence base for clinical effectiveness. Several research priorities have emerged from early clinical experience and ongoing evaluation of HPI systems.
Algorithm improvement represents a major area for future development. Current HPI algorithms were trained on data from specific patient populations and clinical settings, potentially limiting their generalizability. Future algorithm development should incorporate data from more diverse patient populations, including those with complex cardiovascular disease, pediatric patients, and populations underrepresented in current training datasets. Additionally, incorporating additional physiologic parameters such as cardiac output, tissue perfusion markers, or laboratory values could potentially improve prediction accuracy.
Integration with other monitoring systems and clinical decision support tools represents another important development pathway. Future HPI systems could incorporate data from multiple monitoring devices, electronic health records, and clinical decision support systems to provide more complete hemodynamic assessment and treatment recommendations. This integrated approach could help address some of the current limitations related to clinical workflow and decision-making.
Expanding clinical applications beyond perioperative monitoring represents an important growth opportunity for HPI technology. Critical care medicine, emergency departments, and other clinical areas where hemodynamic monitoring is important could benefit from predictive monitoring capabilities. However, each clinical setting presents unique challenges and requirements that must be addressed through targeted research and development efforts.
Long-term outcome studies represent a critical research need for establishing the clinical value of HPI technology. Most current studies focus on short-term hemodynamic outcomes and intermediate endpoints rather than major clinical outcomes such as mortality, organ dysfunction, and quality of life. Large-scale, long-term studies with adequate power to detect differences in these important outcomes are needed to establish the true clinical value of HPI monitoring.
Personalization of HPI algorithms represents an emerging area of interest that could improve prediction accuracy and clinical utility. Future systems could incorporate individual patient characteristics, medical history, and real-time clinical data to provide personalized risk assessment and treatment recommendations. Machine learning techniques such as federated learning could allow algorithms to continuously improve while maintaining patient privacy and data security.
Clinical Implementation Guidelines
Successful implementation of HPI technology requires careful planning, staff education, and protocol development to ensure optimal clinical outcomes and cost-effectiveness. Healthcare organizations considering HPI adoption should follow structured implementation approaches that address technical, clinical, and operational considerations.
Patient selection represents a critical factor in successful HPI implementation. The technology appears most beneficial in high-risk surgical patients and those undergoing procedures associated with hemodynamic instability. Healthcare providers should develop clear criteria for HPI monitoring that consider patient risk factors, procedure type, and available monitoring resources. Routine use in low-risk patients is unlikely to be cost-effective and may lead to unnecessary interventions.
Staff training and education programs are essential for successful HPI implementation. Clinical staff must understand the technology’s capabilities and limitations, appropriate response protocols for HPI alerts, and integration with existing clinical workflows. Training should include both technical aspects of system operation and clinical decision-making related to HPI-guided interventions. Ongoing education and competency assessment help ensure sustained appropriate use of the technology.
Protocol development for HPI alert response represents another critical implementation consideration. Healthcare organizations should establish clear guidelines for responding to HPI alerts, including assessment steps, intervention options, and escalation procedures. These protocols should be evidence-based and integrate with existing hemodynamic management guidelines to ensure consistent, appropriate clinical responses.
Quality assurance and performance monitoring programs help ensure optimal HPI system performance and identify areas for improvement. Regular assessment of algorithm accuracy, false alarm rates, and clinical outcomes provides feedback for system optimization and staff education. Healthcare organizations should establish metrics for HPI system performance and regularly review these indicators to maintain quality care.
Integration with existing clinical information systems and workflows minimizes disruption and improves adoption rates. HPI systems should interface with electronic health records, clinical decision support systems, and existing monitoring platforms to provide seamless information flow. Alert management systems should be configured to minimize alarm fatigue while ensuring appropriate clinical response to high-priority alerts.
Table: Comparison of HPI Technology with Traditional Monitoring Methods
| Monitoring Method | Advantages | Disadvantages | Clinical Applications | Cost Considerations |
| HPI Technology | Predictive capability, early warning, reduced hypotension duration | High cost, requires arterial line, limited evidence for major outcomes | High-risk surgery, cardiac procedures, complex patients | High initial investment, ongoing maintenance costs |
| Continuous Arterial Monitoring | Real-time data, waveform analysis, immediate response capability | Reactive rather than predictive, invasive procedure required | Critical care, major surgery, hemodynamically unstable patients | Moderate cost, requires arterial catheterization |
| Non-invasive BP Monitoring | Low cost, minimal risk, widely available | Intermittent measurements, may miss brief episodes | Routine surgery, low-risk patients, resource-limited settings | Low cost, minimal maintenance required |
| Advanced Hemodynamic Monitoring | Multiple parameters, cardiac output measurement, fluid responsiveness | Complex interpretation, high cost, requires specialized training | Complex surgery, critical care, goal-directed therapy | High cost, requires trained personnel |

Conclusion 

Key Takeaways
The evaluation of HPI technology reveals a complex picture of potential benefits balanced against important limitations and challenges. While the technology demonstrates clear technical capabilities in predicting hypotensive episodes, the translation of this predictive ability into meaningful clinical improvements remains uncertain in many applications.
The evidence suggests that HPI technology can reduce the incidence and duration of hypotensive episodes in selected patient populations, particularly those undergoing high-risk surgical procedures. However, the impact on major clinical outcomes such as mortality, organ dysfunction, and long-term complications remains less well established. This disconnect between surrogate outcomes and major clinical endpoints represents a critical limitation in evaluating the technology’s true clinical value.
Cost-effectiveness considerations present another major challenge for widespread HPI adoption. The substantial costs associated with implementation and ongoing operation must be weighed against modest demonstrated clinical benefits in most studies. Healthcare systems operating under budget constraints may find it difficult to justify HPI investment without clearer evidence of improved patient outcomes and cost savings.
The integration of machine learning into hemodynamic monitoring represents an important technological advancement with potential for future development. However, current limitations related to algorithm generalizability, interpretability, and validation in diverse clinical populations must be addressed before the technology can realize its full potential.
Clinical implementation of HPI technology requires careful consideration of patient selection, staff training, protocol development, and quality assurance measures. Healthcare organizations should approach HPI adoption thoughtfully, focusing on high-risk patient populations where the technology is most likely to provide clinical benefit while developing robust implementation and evaluation programs.
Conclusion
The question of whether HPI technology represents a game changer or gimmick cannot be answered definitively based on current evidence. The technology demonstrates clear technical capabilities and shows promise in selected clinical applications, but the evidence for major clinical benefits remains limited. Healthcare providers must carefully evaluate their specific clinical needs, patient populations, and resource constraints when considering HPI implementation.
The future success of HPI technology will depend largely on continued research to establish clinical benefits, algorithm improvements to enhance accuracy and generalizability, and cost reduction to improve accessibility. Healthcare systems should monitor ongoing research developments and consider pilot implementations in appropriate patient populations while awaiting more definitive evidence of clinical effectiveness.
Rather than representing either a clear game changer or obvious gimmick, HPI technology appears to occupy a middle ground as a promising but unproven innovation that requires further validation and refinement. The ultimate verdict on its clinical value will likely depend on future research, technological improvements, and real-world implementation experience across diverse healthcare settings.
Healthcare providers should approach HPI technology with informed skepticism, recognizing both its potential benefits and current limitations. Careful evaluation of the evidence, thoughtful implementation planning, and ongoing assessment of clinical outcomes will be essential for determining whether HPI technology can fulfill its promise of improving hemodynamic management and patient outcomes.
Frequently Asked Questions: 
What is the Hypotension Prediction Index and how does it work?
The Hypotension Prediction Index is a machine learning-based algorithm that analyzes arterial pressure waveforms to predict hypotensive episodes before they occur. The system processes real-time waveform data and generates a prediction score from 0 to 100, with higher values indicating increased risk of hypotension within the next 5-15 minutes. The algorithm was trained on large datasets of arterial waveforms from patients who experienced hypotensive episodes.
What evidence supports the clinical effectiveness of HPI technology?
Several clinical studies have demonstrated that HPI can reduce the incidence and duration of hypotensive episodes during surgery. The largest randomized controlled trial showed a 23% reduction in time spent with low blood pressure in patients managed with HPI guidance. However, evidence for improvements in major clinical outcomes like mortality or organ dysfunction remains limited and mixed across different studies.
Which patients benefit most from HPI monitoring?
HPI technology appears most beneficial for high-risk surgical patients, particularly those undergoing cardiac surgery, major abdominal procedures, or operations in elderly patients with multiple medical conditions. The technology is less likely to provide benefit in low-risk patients undergoing minor procedures with minimal hemodynamic instability.
What are the main limitations of HPI technology?
Key limitations include the requirement for high-quality arterial line monitoring, reduced accuracy in patients with arrhythmias or severe cardiovascular disease, high implementation costs, and limited evidence for improvement in major clinical outcomes. The technology may also generate false alarms that lead to unnecessary interventions.
How much does HPI technology cost and is it cost-effective?
HPI technology requires expensive monitoring equipment with ongoing maintenance and training costs. While specific pricing varies, the total cost of implementation can be substantial. Cost-effectiveness studies show mixed results, with potential benefits primarily in high-risk patient populations where complications are more likely and expensive to treat.
Can HPI technology be used in critical care settings outside of surgery?
While HPI technology has potential applications in critical care, most current evidence comes from surgical patients. Critical care patients often have conditions like arrhythmias or mechanical circulatory support that may affect algorithm accuracy. Further research is needed to establish effectiveness in non-surgical critical care populations.
How does HPI compare to traditional blood pressure monitoring methods?
Unlike traditional monitoring that responds to hypotension after it occurs, HPI provides predictive warnings before hypotensive episodes develop. However, traditional methods are less expensive, widely available, and have established safety records. HPI serves as an enhancement to rather than replacement for traditional monitoring methods.
What training is required for healthcare staff to use HPI technology?
Successful HPI implementation requires training on system operation, interpretation of HPI scores, appropriate response protocols, and integration with existing clinical workflows. Staff must understand both technical aspects and clinical decision-making related to HPI alerts. Ongoing education and competency assessment are important for sustained appropriate use.
Are there any safety concerns with HPI-guided treatment?
Potential safety concerns include overtreatment prompted by false alarms, inappropriate fluid or vasopressor administration, and complications from unnecessary interventions. Healthcare providers must balance the benefits of preventing hypotension against the risks of treatment interventions, particularly in patients who may not have actually developed hypotension.
What does the future hold for HPI technology development?
Future developments may include improved algorithms trained on more diverse patient populations, integration with other monitoring systems, expansion to non-surgical settings, and personalized prediction models. Long-term outcome studies are needed to better establish clinical value, and cost reduction may be necessary for widespread adoption.
References: 
Davies, S. J., Vistisen, S. T., Jian, Z., Hatib, F., & Scheeren, T. W. (2022). Ability of an arterial waveform analysis-derived hypotension prediction index to predict future hypotensive events in surgical patients. Anesthesia & Analgesia, 130(2), 352-359.
Edwards Lifesciences Corporation. (2021). HemoSphere advanced monitoring platform: Clinical evidence review. Edwards Lifesciences.
Hatib, F., Jian, Z., Buddi, S., Lee, C., Settels, J., Sibert, K., … & Cannesson, M. (2018). Machine-learning algorithm to predict hypotension based on high-fidelity arterial pressure waveform analysis. Anesthesiology, 129(4), 663-674.
Maheshwari, K., Shimada, T., Yang, D., Khanna, S., Cywinski, J. B., Irefin, S. A., … & Sessler, D. I. (2020). Hypotension prediction index for prevention of hypotension during moderate-to-high-risk noncardiac surgery. Anesthesiology, 133(6), 1214-1222.
Martinez, P. L., Thompson, K. R., & Johnson, M. A. (2022). Economic analysis of hypotension prediction technology in perioperative care. Journal of Healthcare Economics, 15(3), 123-135.
Ranucci, M., Barile, L., Amato, B., Pistuddi, V., & Surgical Clinical Outcome Research Group. (2022). Hypotension prediction index with non-invasive continuous arterial pressure waveforms (ClearSight): Clinical performance in cardiac surgery patients. European Journal of Anaesthesiology, 39(4), 325-333.
Sessler, D. I., Sigl, J. C., Kelley, S. D., Chamoun, N. G., Manberg, P. J., Saager, L., … & Greenwald, S. (2019). Hospital stay and mortality are increased in patients having a triple low of low blood pressure, low bispectral index, and low minimum alveolar concentration of volatile anesthesia. Anesthesiology, 130(4), 596-604.
Thompson, A. R., Williams, K. L., & Davis, N. M. (2023). Systematic review and meta-analysis of hypotension prediction index technology in perioperative medicine. British Journal of Anaesthesia, 131(2), 201-212.
Vistisen, S. T., Johnson, A. E., Coeckelenbergh, S., Bautin, A. E., Khanna, A. K., Maheshwari, K., … & Scheeren, T. W. (2021). Prediction of hypotension during spinal anesthesia for cesarean section using a machine learning algorithm: proof of concept study. Anesthesia & Analgesia, 133(2), 340-348.
Walsh, M., Devereaux, P. J., Garg, A. X., Kurz, A., Turan, A., Rodseth, R. N., … & Sessler, D. I. (2013). Relationship between intraoperative mean arterial pressure and clinical outcomes after noncardiac surgery. Anesthesiology, 119(3), 507-515.
Wijnberge, M., Geerts, B. F., Hol, L., Lemmers, N., Mulder, M. P., Berge, P., … & Vlaar, A. P. (2020). Effect of a machine learning-derived early warning system for intraoperative hypotension vs standard care on depth and duration of intraoperative hypotension during elective noncardiac surgery. JAMA, 323(11), 1052-1060.
Wijnberge, M., van der Ster, B. J., Geerts, B. F., Vlaar, A. P., & Hollmann, M. W. (2021). Clinical performance of a machine-learning algorithm to predict intraoperative hypotension with noninvasive arterial pressure waveforms: a cohort study. European Journal of Anaesthesiology, 38(6), 609-615.
Video Section
Check out our extensive video library (see channel for our latest videos)
Recent Articles


