
Iron Deficiency and Anemia
GlobalRPh student writer
Iron is an essential mineral. Be it forming and oxygenating blood cells and hemoglobin, maintaining the immune system, or contributing to cognitive function, the human body needs iron. This said, iron deficiency is the most common nutritional deficiency in the world. Almost 2 billion people are iron-deficient, according to the stats.
What Is Iron Deficiency
Not having enough iron in the body is known as iron deficiency or sideropenia. Total body iron of an adult is about 4 g and about 70 percent of it is found in hemoglobin and myoglobin. Hemoglobin is the oxygen carrier in red blood cells (RBC) whereas myoglobin is that of muscles. Without sufficient iron, the body can’t make red blood cells. The result: tiredness and lack of energy. Plus, it can lead to many health problems, including iron deficiency anemia.
Signs of Iron Deficiency
The signs and symptoms of iron deficiency vary, depending on its severity, as well as a person’s age and health status. In some cases, it is also possible to be iron deficient and have no symptoms. Common signs include:
- Fatigue: One of the most common symptoms of an iron deficit. This is because less oxygen reaches muscles and tissues, depriving them of energy. Also, the heart tries to pump more oxygenated blood around the body, which can drain a person’s energy.
- Pale skin: Hemoglobin gives blood its color and, thus, the skin its rosy hue. Low iron may be to blame if the gums, inside of lips and bottom eyelids are pale.
- Shortness of Breath: Low hemoglobin levels translate into poor oxygen transportation to muscles and tissues and heightened breathing rate. Blame it on iron deficiency, if you feel out of air while doing easy daily tasks.
- Restless leg syndrome: Approximately 15% of people with restless leg syndrome may have iron deficiency, says John Hopkins Medicine.
- Frequent headaches: Lack of iron can cause the brain arteries to swell, which then translates into headaches, says the National Headache Foundation. This is because the body prioritizes getting more oxygen to the brain.
- Anxiety (for no reason): A lack of oxygen revs up heartbeat and sympathetic nervous system. The result: fight-or-flight mode even when one has every reason to feel ‘Zen’.
- Hair loss: Losing around 100 hairs on a good day is normal. Having iron deficiency inhibits hemoglobin production, which is essential for hair growth. The result: excessive thinning of hair.
- Underactive thyroid gland: Iron is essential for thyroid function, says the National Academy of Hypothyroidism. Iron-deficient people experience low energy levels and sudden weight gain because of an underactive thyroid gland.
- Inflamed tongue (Glossitis): Low iron levels significantly reduce myoglobin, an iron-containing protein in muscle. As a result, iron-deficient people complain of swelling, sores or strangely smooth tongue.
Causes of Iron deficiency
People can have low iron levels for several reasons:
- Iron malabsorption: Age and medications can interrupt the body’s ability to absorb ion even after consuming iron-rich foods. Medical conditions such as inflammatory bowel disease (IBD) or surgical procedures can also contribute to iron deficiency and anemia.
- Blood loss: Chronic blood loss can cause one to lose more red blood cells and iron. Blood loss can be a result of,
- Internal bleeding from ulcers, colon cancer and bleeding disorders such as von Willebrand disease and polycythemia vera.
- Long-term use of aspirin or nonsteroidal anti-inflammatory drugs (NSAIDs)
- Heavy menstrual periods
- Frequent blood tests or donations
- Urinary tract bleeding
- Inadequate dietary intake: Poorly balanced vegetarian or vegan diet and chronic fad dieting can create an imbalance in iron levels in the body. Infants, adolescent girls, pregnant women, and lactating mothers need more iron than others. Consuming iron-fortified formulas and iron-rich foods ensure they get enough iron for bodily functions.
- Exercise: athletes are more prone to iron deficiency anemia because regular workout increases the iron requirement of the body. For instance, hard exercises promote red blood cell production, while the iron is lost through sweat and urine. Mechanical hemolysis (destruction of red blood cells from physical shear) and exercise-induced gastrointestinal bleeding also contribute to iron deficiency in endurance athletes. Furthermore, a high-carb low-fat diet can increase the risk of iron deficiency.
Other causes include obesity, gut infections, urinary tract bleeding, kidney failure, and congestive heart failure.
The Risk Factors
Some iron deficiency risk factors can be managed, while other factors may be beyond control. For example, age, gender, and health status. Also, iron deficiency is much more prevalent in the populations of developing nations, with women and children having an increased risk of developing anemia.
At-Risk Groups
- Pregnant women: Blood volume increases by 30 to 50 percent during pregnancy. This, in turn, increases fetus’ iron demand to produce red blood cells (especially during the third trimester). Women who don’t have enough iron stores can develop iron deficiency anemia. This can be further aggravated with other factors like twin pregnancy, low iron diet, repeated pregnancies or adolescent pregnancy.
- Women with heavy periods: Due to excessive blood loss and increased blood supply demands, this category of women is the most affected ones – with a global prevalence of approximately 42%.
- Adolescent girls: Their often poor or restricted diets – combined with puberty changes – put these girls in the high-risk groups.
- Young children: Toddlers and preschoolers have the highest prevalence of iron deficiency anemia – a whopping 47%, says World Health Organization (WHO). Young children often receive a good supply of cow’s milk, yet it is not sufficient to meet the daily iron requirements. Moreover, cow’s milk can decrease iron absorption and can irritate the intestinal lining.
- People who have gone Surgeries: Surgical procedures can also increase a person’s risk of becoming iron-deficient and anemic.
- Malnourished people: People living in developing nations are another group susceptible to iron deficiency. Incidences of malnutrition and immunodeficiency worsen the situation.
- Frequent blood donors: Studies show that serum ferritin levels of regular blood donors than non donors. Ferritin is an iron-containing protein that is used as a marker to test the iron reserves of the human body.
How Much Iron Is Needed
The recommended daily intake (RDI) isn’t one-size-fits-all, especially for children and women. Adult women between the ages of 19 and 50 require 18 mg of iron a day, with men in that age requiring 20 mg. For pregnant women, the RDI bumps up to 27 mg whereas lactating mothers require only 9 mg. Plus, the heaviness of the period could alter the iron requirements in women. However, after women stop menstruating, the number goes down considerably to 8 mg per day. Since non-heme has a low absorption rate, the RDI for vegans and vegetarians is 1.8X that of meat-eaters.
How To Get More Iron
Of the several nutrients, the human body can’t make six groups essential nutrients on its own. These nutrients (vitamins, minerals, protein, fat, carbohydrate, and water) must come from food. Food has two types of iron – heme (found in animal products) and non-heme (found in plants). Heme iron is easier to absorb- about 30 percent of what one consumes whereas the human body can absorb only 2 to 10 percent of the non-heme iron. Some of the best heme iron foods are:
- Liver (chicken and beef)
- Oysters, clams, and mussels
- Red meat (Lean Beef and lamb)
- Chicken and Turkey
- Tuna and Canned Sardines
Moving onto the best non-heme foods, we have
- Legumes (beans, lentils, and peas)
- Nuts and Seeds (Pumpkin, Flaxseeds, cashews and macadamia nuts)
- Leafy Greens (spinach, kale, swiss chard, collard)
- Whole-grain and enriched bread
- Corn syrup and Maple syrup
Fill the plates with these iron-rich foods to reduce the risk of iron deficiency and anemia.
Iron Regulation
The human body maintains appropriate levels of iron for vital functions, even if the iron consumption rate doesn’t always exactly match with iron loss. Thanks to ferritin, a protein that can store 4500 iron (III) ions per protein molecule. Ferritin stores extra iron (mostly in the liver) and uses it during times when dietary intake is inadequate. Thus, it acts as a ‘buffer’ against iron deficiency and iron overload. Poor dietary intake and diseases can affect the body’s iron regulation. Over time, this results in the depletion of iron stores in the body. Most common effects include:
- Iron depletion: It occurs when the hemoglobin levels are normal but a small amount of stored iron. It usually has no obvious signs and symptoms.
- Iron deficiency: Both iron and hemoglobin levels drop below normal. Iron-deficient people may experience some symptoms, including fatigue, dizziness, and poor appetite.
- Iron deficiency anemia: It is characterized by a lower-than-normal RBC count and insufficient hemoglobin levels. Symptoms include fatigue, shortness of breath, lightheadedness, and palpitations. Cognition impairment and immunodeficiency diseases are also common in anemic patients.
How Iron Deficiency Is Diagnosed
Doctors diagnose iron deficiency with blood tests.
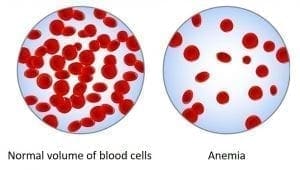
- Complete blood count (CBC): It determines red blood cells (RBCs), white blood cells (WBCs), hemoglobin, hematocrit, and platelets. The CBC also helps to diagnose iron deficiency anemia. Smaller RBCs and low hematocrit and hemoglobin levels are characteristics of iron deficiency anemia.
- Transferrin test: It measures transferrin (iron transporting protein) levels in the blood. Under normal conditions, transferrin is one-third saturated with iron and two-thirds is held in reserve.
- TIBC (total iron-binding capacity): It measures the total amount of iron that can be bound by circulatory proteins. Since transferrin is the primary iron-binding protein, the TIBC test is an alternative to measure transferrin availability.
- Serum iron and ferritin levels: These are indicators of the amount of iron available in the blood and body.
- Fecal occult blood test (FOBT): Iron deficiency due to gastrointestinal bleeding may show a positive FOBT.
Iron Deficiency: Therapeutic Options
Iron deficiency treatment is a two-step approach: first, finding and treating the underlying cause and then bringing back iron levels back to normal. Finding the type of deficiency and what is causing it is important in older patients. Because the risk of developing colorectal cancer and gastrointestinal bleeding gets higher with age. Stats show that about 60% of iron deficient adults may have gastrointestinal disorders leading to heavy blood loss. Next comes oral iron supplementation using iron salts and/or iron-rich foods. The choice of the supplement depends on the severity of iron deficiency, recovery period, and the health profile of the patient. The non-prescription iron supplements come with two forms of iron: ferrous and ferric. Ferrous iron salts (ferrous sulfate, ferrous gluconate, and ferrous fumarate) are faster absorbing forms. Generally, they are administered with ascorbic acid to boost bioavailability. Taking iron supplements with orange and grapefruit juice is also recommended to improve absorption. Eating iron-rich foods also helps to restore iron levels in the body.
Additional notes
Self-diagnosis and self-medication are not recommended. Taking iron supplements when tired or light-headed will not help unless iron deficiency anemia is confirmed.
Fatigue, paleness, and palpitations can be symptomatic of other health conditions, not just iron deficiency or anemia. Some of them could be an early sign of chronic diseases.
Don’t overdo iron supplements. They may interfere with the absorption of other minerals, including copper and zinc.
Nausea, constipation, diarrhea and black stools are the common side effects associated with oral iron replacement therapy.
Iron overdose can be fatal.
Iron Deficiency – Anemia
Tables / Articles / Dilutions
Calculators / Tools

