iStent Combination Therapy for Glaucoma and Cataracts
Considering that glaucoma is the most common cause of irreversible vision loss and the third most common cause of vision loss worldwide, with cataracts and refractive error being the most prevalent causes, iStent combination therapy to treat glaucoma and cataracts has high therapeutic value. According to the American Academy of Ophthalmology, glaucoma prevention and treatment has been a major focus of international directives, including the World Health Organization’s Vision 2020 campaign. While this initiative saw a successful decrease in worldwide blindness, most of the improvement was due to widespread adoption of cataract surgery and spectacles provision. As reported by the BrightFocus Foundation, more than three million Americans are living with glaucoma, 2.7 million of whom—aged 40 and older—are affected by its most common form, open-angle glaucoma. In 2020, about 80 million people have glaucoma worldwide, and this number is expected to increase to over 111 million by 2040. Per a 2020 systematic review of global cataract prevalence data published in Eye, studies indicate that 36 million people are blind worldwide, and over 12 million of them are due to cataracts.
Current Treatments
The most common form of glaucoma is open-angle, and the primary treatment strategies involve reducing the abnormally elevated intraocular pressure (IOP). Usually, glaucoma can be managed at its onset with topical therapies, but some patients become refractory and require surgical intervention. In initial treatment phases, combination eye drop therapies are also being developed. Trabeculectomy is a well established surgical treatment option that improves IOP elevation in about 60-80% of patients for a period of a few years. Due to its invasive nature, and risk of postsurgical complications, improvements or alternatives to trabeculectomy have been the subject of research for over a decade. Similarly, cataracts are treated surgically, and efforts to improve these procedures are always a research focus.
iStent Combination Therapy Device Development
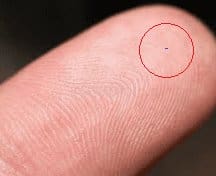
A new device by Glaukos Corporation aims to treat glaucoma and cataracts simultaneously. iStent is an L-shaped bio-titanium device (with a size of 1mm by 0.33mm) covered with heparin that has a 120 micrometer snorkel. The snorkel of this device is implanted in the anterior chamber and anchored in the Schlemm’s canal, and allows for a reduction in IOP. iStent can be placed during cataract surgery, giving patients the option to treat both glaucoma and cataracts with one procedure. Previous studies have demonstrated the effectiveness of iStent at long-term IOP reduction. Size approximation of the iStent device is shown here.
iStent Combination Therapy Study Details
The chief objective of this study was to evaluate the post-operative IOP reduction in patients after iStent and cataract phacoemulsification combination surgery.
Patients
Eligible study participants were experiencing mild to moderate open-angle glaucoma and at least one cataract. 57 patients (and 78) eyes participated in this study, all of which were 40 or greater years old (with mean age of 77). 67% of study participants were female. Inclusion criteria included cataract presence with visual field disturbance and either glaucoma progression or intolerance to current treatment. Exclusion criteria included severe proliferative diabetic retinopathy, corneal clouding, advanced-stage macular degeneration, closed or narrow-angle glaucoma, previous glaucoma surgeries (including trabeculoplasty), and the use of more than four medications to regulate IOP.
Methods
All tenets of the Declaration of Helsinki were observed. This study was approved by the Bioethics Committee at the Military Institute of Medicine and the Bioethics Committee of Medical University of Bialystok. Patients completed written informed consent prior to study initiation. This study was registered under number NCT03807869 at ClinicalTrials.gov.
All procedures were performed by two surgeons at two centers (Department of Ophthalmology, Military Medical Institute in Warsaw and Department of Ophthalmology Medical University in Bialystok). Patients underwent cataract phacoemulsification first (posterior-chamber artificial lens insertion) followed by insertion of a first-generation iStent. Patients received intracameral cefuroxime at the end conclusion of the iStent combination therapy, and were treated with moxifloxacin eye drops for two weeks as well as loteprednol eye drops for four weeks post-op. Follow-up appointments were scheduled for day 1, week 1, and months 1, 3, 6, 12 and 24. Patients were not allowed to use IOP reducing medications after surgery. Eye exams were completed at appointments and included IOP measurement, visual acuity via Snellen chart, and biomicroscopic exam of anterior segment and fundus, as well as assessment of the retina and optic nerve disc. All post-operative complications were noted.
Effective IOP reduction was defined as greater than 20% reduction. Complete surgical success was defined as IOP less than or equal to 15 mmHg without medications.
Statistical Analysis
R program, version 3.5.1 was used to perform statistical analysis on study variables. Shapiro-Wilk test was used to analyze the normality of the distribution of quantitative variables. Leven testing was used to verify the equality of variance within parameters. Significance level of 0.05 and 95% confidence intervals were used throughout.
Results
iStent Combination Therapy and IOP
Pre-surgical IOP mean was 18.44 +/-3.5 mmHg. IOP change at month 12 post-operative was -2.33 +/-3.81 mmHg, and IOP change was -2.7 +/- 4.18 mmHg at month 24. Preoperative IOP pressures were statistically different from those of month 12 and 24 (p<0.0001). Zero eyes had a preoperative IOP of less than 15 mmHg, and 23.4% of postoperative eyes achieved this IOP. Effective IOP treatment was achieved in 64% of patients. Surgical success was achieved in 51.9% of patients.
iStent Combination Therapy and Medication Burden
At post-operative month 24, medication burden reduction was statistically significant (p<0.0001). The following changes were observed: 10.8% of patients reduced medication use by 3 medications, 21% of patients reduced use by 2 medications, 49% of patients reduced medications by one, 12.8% of patients did not change the amount of medication used. In 87.2% of patients, IOP and the number of medications used were reduced at month 24 compared to preoperative use. In 94.7% of patients, IOP was reduced or stayed the same and the number of medications was reduced or stay the same as preoperative use. Preoperatively, 2.6% of eyes were medication free, and at postoperative month 24, 68% of eyes were medication free (p<0.05).
Safety Results
No allergies, inflammation, or significant surgical complications were reported during iStent implantation or the cataract procedure. Seven cases of microhyphema in the anterior chamber and corneal edema with Descent’s fold were observed at week 1, but all spontaneously resolved without additional treatment.
Discussion: iStent Combination Therapy
In this study, iStent implantation and cataract phacoemulsification provided a statistically significant IOP reduction in patients. The average 2.7 mmHg reduction in IOP is clinically important considering that every 1 mmHg reduction in IOP decreases glaucoma progression risk by 10%. Medication burden was also reduced as a result of this intervention. This is highly desirable as patients tend to become refractory to medication therapies in time, and can be at risk for allergies and ocular surface impairment. Medication burden reduction is always highly valuable to patients, who rely on adherence to treatment plans to maintain IOP reduction. 68% of eyes using no medication at the end of this study is an important finding. The low rate of safety results further enhance these results.
This study was conducted in a Polish Caucasian patient population, but these results are similar to those reported by other researchers in the United Kingdom, in Asian populations, and Arabic patients. The safety profiles were also similar in these study populations.
Disclosure
No conflicts of interest were reported.
Navigation
Ophthalmology Related Tables and Apps
- Ophthalmic anesthetics
- Ophthalmic Antibacterials and combination products
- Ophthalmic Anti-allergy agents
- Ophthalmic Antivirals
- Ophthalmic Corticosteroids
- Ophthalmic – Dry eye disease (DED)
- Ophthalmic – Glaucoma
- Ophthalmic Mydriatics
- Ophthalmic NSAIDs
Glaucoma
- New Glaucoma Drug Selection tool – Medical App
- Potency of Glaucoma drops – Medical App
- Glaucoma – BAK-free and Preservative-free drops Medical App
- Medical Treatment of Dry Eye Disease (Ophthalmic drops)- Medical App
Other
Latest Research

